CPD frameworks
These frameworks, associated with all articles, prompt drafting of personal learning, reflection and planning.
Save your reflective note into your device or cloud
Fillable PDF frameworks
Adobe reader needed for tablets
Word frameworks - for reflective practice
Click to download
Reflection on a journal article
Stages of reflection on a situation
Reflection of a team, practice or group
External reference on reflection
Reflective practice in health care and how to reflect effectively
Koshy K, Limb C et al. International Journal of Surgical Oncology. 2017 2:e20
Musculoskeletal medicine - Special interest
Symposium articles
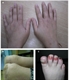 |
|Prompt diagnosis key in improving outcomes in psoriatic arthritis
25 Oct 2022
If left untreated psoriatic arthritis (PsA) can result in progressive, irreversible joint damage causing chronic pain and disability. It is a chronic, autoimmune inflammatory condition that can affect up to 30% of patients with psoriasis. PsA is a multisystem disease affecting other organs such as the eyes, gut and tendons. It is associated with multiple comorbidities such as diabetes mellitus, cardiovascular disease and metabolic syndrome. If PsA is suspected in primary care, routine blood tests should be requested to check for anaemia of chronic disease and raised inflammatory markers. Plain radiographs of hands and feet should be requested prior to referral, although classical changes do not occur early in the disease. If GPs suspect PsA, prompt referral is paramount. Patients should be referred if they have persistent joint symptoms, a positive screening questionnaire (PEST), joint swelling, dactylitis or enthesitis, and/or inflammatory back pain.
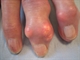 |
|Treat-to-target urate-lowering therapy: the cornerstone of gout management
25 Oct 2022
Gout is a common complex disorder resulting from variable interaction between genetic, constitutional, and environmental factors. Heritability of gout is around 60%, and individual dietary factors account for < 1% of serum urate (SU) variance compared with 24% from the genetic variations currently identified. The most common presentation is a gout flare, characterised by acute onset of one or occasionally more hot, red, swollen joints which are extremely painful. Treat-to-target urate-lowering therapy aims to reduce and maintain urate levels in peripheral joint tissues well below saturation (SU < 360 µmol/L). This prevents further crystal formation and gradually dissolves away existing crystals, after which no further flares occur, and further risk of crystal-induced joint damage is removed.
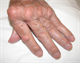 |
|Treating to target will optimise long-term outcomes in RA
24 Nov 2020
Rheumatoid arthritis (RA) classically causes a symmetrical, small joint polyarthritis which left untreated can lead to joint destruction and deformity. NICE recommends that any adult with suspected persistent synovitis of undetermined cause should be referred for a specialist opinion. Patients should be referred urgently (even with a normal acute-phase response, negative anti-CCP antibodies or rheumatoid factor) if any of the following apply: the small joints of the hands or feet are affected; > 1 joint is affected; there has been a delay of = 3 months between onset of symptoms and seeking medical advice.
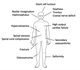 |
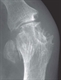
|Diagnosis and management of Paget’s disease of bone
24 Nov 2020
Paget’s disease of bone is a metabolic disease in which focal abnormalities of bone remodelling occur in one or more skeletal sites. The affected bones enlarge and may become deformed and this can lead to complications including bone pain, pathological fractures, secondary osteoarthritis, deafness and nerve compression syndromes. The three main risk factors are age, male gender and family history. People with a first-degree relative with Paget’s disease have a seven-fold increased risk of developing the disease. Patients who have bone deformity or symptoms that might be due to Paget’s disease should be referred to secondary care.
 |
|Education the key to improving outcomes in gout
22 May 2019
The most common presentation of gout is a flare, characterised by acute onset of one, or occasionally more, hot, red, swollen joints which are very painful and tender. Less common is insidious onset of chronic usage related joint pain, especially in joints already affected by osteoarthritis. Subcutaneous tophi can also be the presentation, particulary in older people. In typical cases, clinical assessment alone is sufficient for diagnosis. Gout is also associated with comorbidities such as nephrolithiasis, chronic kidney disease, metabolic syndrome and heart disease, and increased mortality.
Optimising the management of systemic lupus erythematosus
22 May 2019
Systemic lupus erythematosus (SLE) is a multisystem, autoimmune disease. SLE mainly affects women and causes fatigue, rashes (often associated with photosensitivity), hair loss and inflammatory arthritis. However, it can also affect men in whom it is often more severe with a greater likelihood of renal involvement and a greater degree of organ damage. According to the British Society for Rheumatology guideline, the diagnosis of SLE requires a combination of clinical features and the presence of at least one relevant immunological abnormality.
 |
|Managing low back pain in primary care
20 Dec 2018
Chronic low back pain is a common problem. Lifetime adult prevalence rates vary from 50 to 80%, and around a quarter of adults say they have experienced back pain during the past month. One in 40 report disabling back or neck pain. Each year around 7% of patients consult their GP with back pain. In 65-70% of primary care patients with low back pain there is no known pathoanatomical cause. Their pain is described as nonspecific and is postulated to arise from muscle strain or ligamentous injury. A further 15-20% of patients have mechanical low back pain with an identifiable cause such as degenerative disc or joint disease.
Diagnosis and treatment of Sjögren’s syndrome
20 Dec 2018
Primary Sjögren’s syndrome is a chronic systemic immune-mediated condition of unknown aetiology characterised by focal lymphocytic infiltration of exocrine (mainly salivary and lacrimal) glands. It affects 0.1-4.6% of the European population and 90% of cases are female. Although it usually presents in the fifth or sixth decade, it can be seen in younger people who tend to present with systemic disease and are less likely to have classical sicca symptoms. Patients should be referred to a rheumatologist to confirm diagnosis, and this may involve scintigraphy/sialography and/or labial gland biopsy.
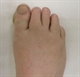 |
|Prompt diagnosis can prevent joint damage in psoriatic arthritis
20 Dec 2017
Psoriatic arthritis (PsA) is a chronic, autoimmune inflammatory condition that can affect up to 30% of patients with psoriasis. It is part of the seronegative spondyloarthropathy group of rheumatic diseases which also includes reactive arthritis and ankylosing spondylitis. It can be a multisystem disease affecting the eyes, the gut and the tendons and is associated with comorbidities such as ischaemic heart disease and metabolic syndrome. Early diagnosis is key as structural joint damage can occur within two years of disease onset.
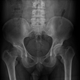 |
|Early recognition pivotal in the management of spondyloarthritis
20 Dec 2017
The spondyloarthritis group is divided into two main subgroups: axial spondyloarthritis and peripheral spondyloarthritis. These may exist as separate entities or coexist in the same patient. Classically, axial spondyloarthritis presents with insidious onset inflammatory lower back pain, which is typically worse in the morning and after rest, and improves with activity. Peripheral spondyloarthritis can present with peripheral joint pain and/or swelling, swelling of the digits (dactylitis), tendon and entheseal pain that is not secondary to a mechanical cause. Early referral of patients with suspected spondyloarthritis to specialist care is strongly recommended as this can improve long-term outcomes.
Special reports
 |
|Psoriatic arthritis often goes unrecognised
21 Dec 2020
Psoriatic arthritis (PsA) is a seronegative systemic disease that belongs to the family of spondyloarthropathies. Its worldwide prevalence ranges from 0.05% to 1%, and it appears in 10-40% of patients with skin psoriasis; however, it is believed to be underdiagnosed. More than 80% of patients who are diagnosed with PsA already have skin disease, mainly in the form of plaque psoriasis. However, 15% of patients present with musculoskeletal involvement prior to psoriasis which makes the diagnosis of PsA challenging. It is important to do a thorough clinical assessment, take a family history and actively look for evidence of psoriasis: this includes examining nails, the scalp, intergluteal region and umbilicus.
-1.32.42-pm.jpg) |
|GPs play a vital role in identifying and managing juvenile idiopathic arthritis
24 Sep 2018
Juvenile idiopathic arthritis (JIA) affects approximately 1-4 per 1,000 children under the age of 16. Girls are more commonly affected than boys. It is a heterogeneous condition, even within JIA categories, ranging from insidious arthritis affecting one to two joints to florid and life-threatening systemic arthritis. All patients with suspected JIA should be referred urgently to a specialist paediatric rheumatology team. Coordinated, multidisciplinary care within a specialist team is required to achieve optimal outcomes.

