Musculoskeletal
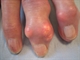 |
|Treat-to-target urate-lowering therapy: the cornerstone of gout management
25 Oct 2022
Gout is a common complex disorder resulting from variable interaction between genetic, constitutional, and environmental factors. Heritability of gout is around 60%, and individual dietary factors account for < 1% of serum urate (SU) variance compared with 24% from the genetic variations currently identified. The most common presentation is a gout flare, characterised by acute onset of one or occasionally more hot, red, swollen joints which are extremely painful. Treat-to-target urate-lowering therapy aims to reduce and maintain urate levels in peripheral joint tissues well below saturation (SU < 360 µmol/L). This prevents further crystal formation and gradually dissolves away existing crystals, after which no further flares occur, and further risk of crystal-induced joint damage is removed.
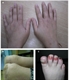 |
|Prompt diagnosis key in improving outcomes in psoriatic arthritis
25 Oct 2022
If left untreated psoriatic arthritis (PsA) can result in progressive, irreversible joint damage causing chronic pain and disability. It is a chronic, autoimmune inflammatory condition that can affect up to 30% of patients with psoriasis. PsA is a multisystem disease affecting other organs such as the eyes, gut and tendons. It is associated with multiple comorbidities such as diabetes mellitus, cardiovascular disease and metabolic syndrome. If PsA is suspected in primary care, routine blood tests should be requested to check for anaemia of chronic disease and raised inflammatory markers. Plain radiographs of hands and feet should be requested prior to referral, although classical changes do not occur early in the disease. If GPs suspect PsA, prompt referral is paramount. Patients should be referred if they have persistent joint symptoms, a positive screening questionnaire (PEST), joint swelling, dactylitis or enthesitis, and/or inflammatory back pain.
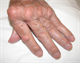 |
|Treating to target will optimise long-term outcomes in RA
24 Nov 2020
Rheumatoid arthritis (RA) classically causes a symmetrical, small joint polyarthritis which left untreated can lead to joint destruction and deformity. NICE recommends that any adult with suspected persistent synovitis of undetermined cause should be referred for a specialist opinion. Patients should be referred urgently (even with a normal acute-phase response, negative anti-CCP antibodies or rheumatoid factor) if any of the following apply: the small joints of the hands or feet are affected; > 1 joint is affected; there has been a delay of ≥ 3 months between onset of symptoms and seeking medical advice.
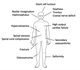 |
|Diagnosis and management of Paget’s disease of bone
24 Nov 2020
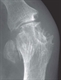
Paget’s disease of bone is a metabolic disease in which focal abnormalities of bone remodelling occur in one or more skeletal sites. The affected bones enlarge and may become deformed and this can lead to complications including bone pain, pathological fractures, secondary osteoarthritis, deafness and nerve compression syndromes. The three main risk factors are age, male gender and family history. People with a first-degree relative with Paget’s disease have a seven-fold increased risk of developing the disease. Patients who have bone deformity or symptoms that might be due to Paget’s disease should be referred to secondary care.
Optimising the management of systemic lupus erythematosus
22 May 2019
Systemic lupus erythematosus (SLE) is a multisystem, autoimmune disease. SLE mainly affects women and causes fatigue, rashes (often associated with photosensitivity), hair loss and inflammatory arthritis. However, it can also affect men in whom it is often more severe with a greater likelihood of renal involvement and a greater degree of organ damage. According to the British Society for Rheumatology guideline, the diagnosis of SLE requires a combination of clinical features and the presence of at least one relevant immunological abnormality.
 |
|Education the key to improving outcomes in gout
22 May 2019
The most common presentation of gout is a flare, characterised by acute onset of one, or occasionally more, hot, red, swollen joints which are very painful and tender. Less common is insidious onset of chronic usage related joint pain, especially in joints already affected by osteoarthritis. Subcutaneous tophi can also be the presentation, particulary in older people. In typical cases, clinical assessment alone is sufficient for diagnosis. Gout is also associated with comorbidities such as nephrolithiasis, chronic kidney disease, metabolic syndrome and heart disease, and increased mortality.
Diagnosis and treatment of Sjögren’s syndrome
20 Dec 2018
Primary Sjögren’s syndrome is a chronic systemic immune-mediated condition of unknown aetiology characterised by focal lymphocytic infiltration of exocrine (mainly salivary and lacrimal) glands. It affects 0.1-4.6% of the European population and 90% of cases are female. Although it usually presents in the fifth or sixth decade, it can be seen in younger people who tend to present with systemic disease and are less likely to have classical sicca symptoms. Patients should be referred to a rheumatologist to confirm diagnosis, and this may involve scintigraphy/sialography and/or labial gland biopsy.
 |
|Managing low back pain in primary care
20 Dec 2018
Chronic low back pain is a common problem. Lifetime adult prevalence rates vary from 50 to 80%, and around a quarter of adults say they have experienced back pain during the past month. One in 40 report disabling back or neck pain. Each year around 7% of patients consult their GP with back pain. In 65-70% of primary care patients with low back pain there is no known pathoanatomical cause. Their pain is described as nonspecific and is postulated to arise from muscle strain or ligamentous injury. A further 15-20% of patients have mechanical low back pain with an identifiable cause such as degenerative disc or joint disease.
 |
|Prompt diagnosis can prevent joint damage in psoriatic arthritis
20 Dec 2017
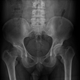
Psoriatic arthritis (PsA) is a chronic, autoimmune inflammatory condition that can affect up to 30% of patients with psoriasis. It is part of the seronegative spondyloarthropathy group of rheumatic diseases which also includes reactive arthritis and ankylosing spondylitis. It can be a multisystem disease affecting the eyes, the gut and the tendons and is associated with comorbidities such as ischaemic heart disease and metabolic syndrome. Early diagnosis is key as structural joint damage can occur within two years of disease onset.
 |
|Early recognition pivotal in the management of spondyloarthritis
20 Dec 2017
The spondyloarthritis group is divided into two main subgroups: axial spondyloarthritis and peripheral spondyloarthritis. These may exist as separate entities or coexist in the same patient. Classically, axial spondyloarthritis presents with insidious onset inflammatory lower back pain, which is typically worse in the morning and after rest, and improves with activity. Peripheral spondyloarthritis can present with peripheral joint pain and/or swelling, swelling of the digits (dactylitis), tendon and entheseal pain that is not secondary to a mechanical cause. Early referral of patients with suspected spondyloarthritis to specialist care is strongly recommended as this can improve long-term outcomes.
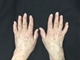 |
|Improving joint pain and function in osteoarthritis
16 Dec 2016
Osteoarthritis has become a major chronic pain condition. It affects more than 10% of adults and accounts for almost 10% of health service resources. The impact of osteoarthritis is amplified by underuse of effective muscle strengthening exercises and a focus on often less effective and poorly tolerated analgesic therapies. Muscle strengthening and aerobic exercise have been shown to improve joint pain and function. Weight loss not only improves joint pain and function but has a myriad of other health benefits.
Diagnosis and management of polymyalgia rheumatica
16 Dec 2016
Polymyalgia rheumatica (PMR) is a common inflammatory condition of unknown aetiology. There is no specific diagnostic test for PMR but the usual pattern is a commensurate rise in CRP and ESR. A small proportion of PMR patients will have normal inflammatory markers. At diagnosis and each follow-up visit it is imperative to consider the potential for associated giant cell arteritis (GCA). If there is any suspicion of GCA, urgent discussion with the rheumatologist should take place that day.
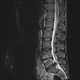 |
|Evaluating the patient with low back pain
22 Dec 2015
In the UK, low back pain is the most common cause of disability in young adults and every year 6-9% of adults consult their GP about back pain. A thorough history and examination is required to exclude an alternative diagnosis, such as pain arising from the hip or trochanteric bursa and to categorise patients as having: serious spinal pathology, nerve root/radicular pain or non-specific back pain.
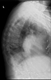 |
|Diagnosis and management of osteoporosis
22 Dec 2015
Osteoporosis is a common condition characterised by low bone mineral density and an increased risk of fragility fractures. It affects up to 30% of women and 12% of men at some point in their lives. The diagnosis of osteoporosis can be confirmed by DEXA but this should only be performed in patients who have an increased risk of fracture on the basis of clinical risk factors. DEXA should be considered if the 10-year risk of major osteoporotic fracture is > 10%.
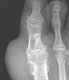 |
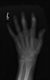
|Patients with gout can be cured in primary care
15 Dec 2014
Gout is associated with comorbidities such as nephrolithiasis, chronic renal impairment, metabolic syndrome, depression and heart disease. It is also associated with increased mortality. Untreated gout can result in disabling irreversible peripheral joint damage and chronic usage-related pain. However, gout is curable. [With external links to the evidence base]
 |
|Early treatment of psoriatic arthritis improves prognosis
15 Dec 2014
Psoriatic arthritis (PsA) is a chronic, autoimmune disease affecting up to 1% of the adult population and up to 40% of those with psoriasis. Around 20% of patients develop PsA before psoriasis, often many years before skin or nail changes. Aggressive treatment of early stage progressive PsA can substantially improve the long-term prognosis.
Optimising the management of congenital talipes
23 Oct 2013
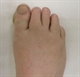
Congenital talipes equinovarus (CTEV) is a condition of the lower limb in which there is fixed structural cavus, forefoot adductus, hindfoot varus and ankle equinus. It is important to differentiate CTEV from a non-structural or positional talipes which is fully correctable. This positional variant occurs about five times as commonly as CTEV. The latter condition does not require casting or surgical treatment. The majority of CTEV cases are picked up at the early baby check or on prenatal ultrasound, and referred to the paediatric orthopaedic service. However, some cases are mistaken early on as the positional variant, and may therefore present to the GP e.g. at the six week check. Urgent referral is warranted as the Ponseti treatment should be started early. [With external links to the evidence base]
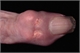
Assessing fracture risk in patients with osteoporosis
23 Oct 2013
In the past the management of osteoporosis centred on the use of diagnostic thresholds based on bone mineral density (BMD) measured at the spine or hip by dual x-ray absorptiometry (DXA). More recently it has been found that the presence of several clinical risk factors is associated with a fracture risk greater than can be accounted for by BMD alone. Assessment of fracture risk therefore needs to take into account specific risk factors that contribute to fracture risk as well as BMD. [With external links to the evidence base]
 |
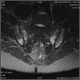
|Diagnosis and treatment of gout in primary care
16 Dec 2011
The prevalence of gout increases with age and up to 7% of men aged over 65 and 3% of women aged over 85 have gout. The risk of gout increases significantly with increasing serum uric acid levels. However, hyperuricaemia is far more common than gout implying that additional risk factors play a role in the development of the disease. Alcohol consumption, especially beer and to a lesser extent spirits, increases the risk of both incident and prevalent gout. Purine-rich foods such as red meat and seafood increase the risk of incident gout significantly, while dairy products and increasing coffee, but not tea, intake were found to be protective. A number of medications are well known to be associated with increased risk of gout. It is well established that gout is frequently associated with the metabolic syndrome which is characterised by hyperuricaemia, hyperlipidaemia, hypertension, diabetes and insulin resistance, and obesity. In addition, dehydration, increasing creatinine levels, and undergoing surgery are known to precipitate gouty flares. [With external links to the evidence base]
 |
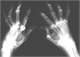
|Early diagnosis crucial in ankylosing spondylitis
16 Dec 2011
Back pain is common with up to 9% of the population consulting their GP with this problem each year. As the vast majority of these patients have non-specific back pain, it is often difficult to identify those with inflammatory disease such as ankylosing spondylitis (AS). It is critical to make this distinction as AS, if untreated, may cause significant morbidity with a substantial socio-economic impact both on the individual and society. Early diagnosis is particularly important as newer therapies are able to contain this condition and even induce remission in some cases. AS affects about 0.2-0.5% of the population. It is at least twice as common in men than women and most often manifests in the third to fifth decades. It is estimated that up to 5% of patients with chronic lower back pain in primary care have inflammatory disease. Diagnosis is usually delayed at least partly through lack of awareness of this condition. [With external links to the evidence base]
 |
|Disease remission the goal of therapy in rheumatoid arthritis
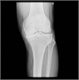
20 Dec 2010
Rheumatoid arthritis was Previously considered a severe systemic disease leading to inexorable decline. However, the outlook for patients has altered dramatically over the past few years with disease remission now the therapeutic goal. This is dependent on a number of critical interventions and the role of the GP is pivotal in the process. Without early recognition and rapid referral by the GP the ability to achieve the desired outcome of disease remission would be greatly hindered. A recent article in this journal highlighted the benefits of intensive therapy with tight control of disease. [With external links to the evidence base]
 |
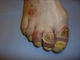
|Optimising pain control in osteoarthritis
20 Dec 2010
Many current treatments for OA are thought to target the synovium e.g. NSAIDs and this may be why they are effective. Changes in the subchondral bone are also common on MRI and are also associated with pain. At present most data assume that OA pain is nociceptive in origin and there is limited evidence for a neuropathic mechanism. All available treatments for OA are directed at symptom control as there are not yet any widely accepted drugs that can affect the structural progression of OA. Current guidelines recommend a combination of non-pharmacological and pharmacological management. Treatment needs to be adjusted according to individual symptoms, past medical history, comorbidities and lifestyle. NSAIDs, for example, may be inappropriate in a patient with renal impairment, gastrointestinal diseases or a history of ischaemic heart disease.The initial approach centres on self-help and patient-driven treatments and should be started in primary care. This includes: education, advice and access to information. Both verbal information and patient information leaflets should be offered; local strengthening exercises and aerobic fitness training; weight loss in patients who are overweight or obese. [With external links to the evidence base]
 |
|Improving recognition of psoriatic arthritis
17 Dec 2009
Psoriatic arthritis (PsA) is a common form of inflammatory arthritis but is underdiagnosed. Psoriasis affects more than 1.5% of the UK population so a GP with an average list size is likely to care for around 40 patients with psoriasis. Around 15% of these patients will be diagnosed with PsA, but up to 40% of them may have evidence of arthritis if reviewed thoroughly. [With external links to the evidence base]
 |
|GPs have key role in shared care of patients with SLE
15 Dec 2009
Twenty to thirty years ago, the mortality rate for SLE was as high as 50% at five years. The current 20-year survival rate is 80%. GPs play a key role in early referral to specialist centres and subsequent shared care pathways for the management of these patients. [With external links to the evidence base]
Diagnosing shoulder pain
01 Jan 2009
The prevalence of shoulder disorders has been reported to range from 7 to 36% of the population accounting for 1.2% of all GP consultations. Shoulder pain has been said to be the second most common musculoskeletal complaint presenting in primary care. On average GPs are consulted approximately seven times each week for a complaint relating to the neck or upper extremity; three of these consultations will be for new complaints or new episodes. [With external links to the evidence base]
 |
|Exercise vital in patients with osteoarthritis
17 Dec 2008
Osteoarthritis (OA) is the most prevalent joint disease in the uk. it is a common cause of pain and disability and the main reason for hip and knee replacement. Three million GP consultations for OA took place in the UK in 2000, and with the ageing population this figure is set to increase.
Assessment of fracture risk key in osteoporosis
17 Dec 2008
Osteoporotic fractures are a major health problem in older people, affecting one in two women and one in five men over 50. These fractures are associated with significant morbidity and increased mortality, and cost the health services an estimated £1.8 billion annually. Recently, it has been shown that prediction of fracture risk can be improved by the use of clinical risk factors independent of BMD. These risk factors, alone or in combination with BMD measurement, form the basis of the WHO-supported FRAX tool for predicting fracture risk. This is available free online at www.shef.ac.uk/frax and can be used to assess the 10-year probability of a patient developing a major osteoporotic fracture (wrist, spine, hip and humerus) or hip fracture.
 |
|Early diagnosis crucial in polyarthralgia
01 Dec 2007
Polyarthralgia is a common presentation in primary care. While the true incidence is unknown, 35% of a large UK community cohort aged over 55 years reported pain in more than one joint. Polyarthralgia is more common in women and with increasing age. Patients often present a diagnostic and management challenge. However, early assessment and diagnosis is important, as there is increasing evidence of the benefit of early intervention in patients with inflammatory arthritis. A window of opportunity exists where the benefits of early treatment may be significant and long-lasting.
 |
|Gout is a risk factor for cardiovascular disease
01 Dec 2007
Gout develops when monosodium urate crystals (MSU) precipitate in a joint, characteristically causing pain, swelling and erythema. The incidence of gout, in the UK, is 13 per 10,000 patient years. It increases with age to a maximal incidence in patients aged 65-84 years. Gout is approximately twice as common in men. Oestrogenic hormones are thought to have a mild uricosuric effect in premenopausal women. [With external links to the evidence base]
 |
|Managing wound problems following joint replacement
01 Feb 2007
Although total hip replacement (THR) and total knee replacement (TKR) are two of the most successful operations in the UK, a peri-prosthetic joint infection (PJI) is a potentially devastating complication associated with high levels of patient morbidity, substantial financial costs and frustration for clinicians. The use of prophylactic antibacterial agents, ultra-clean air and laminar flow systems has reduced the rates of PJI in THR and TKR from about 10 per cent when the operations were first introduced to 0.5-1 per cent for THR and 1-2 per cent for TKR. 'Ringfencing' of elective arthroplasty beds is also beneficial, but this protocol is not universally applied. However, as the UK's population is ageing the number of primary arthroplasty operations and revisions is rising, and the prevalence of PJI is expected to increase.

