The Practitioner
The Practitioner has contributed to the international clinical literature, with over 12,000 entries in PubMed and other major databases. The final issue of The Practitioner (1868-2022) was published at the end of 2022 (Issue No. 1863). However, the website of The Practitioner continues as the Journal's Archive, allowing subscribing institutions and individuals to access issues published in 2009-2022, and as a point of reference for the supply of article PDFs going back to 1868.
Symposium articles
Early diagnosis the main driver to improving outcomes in lung cancer
20 Dec 2022
Earlier diagnosis of lung cancer improves outcomes for two main reasons. First, the disease stage may be earlier allowing more chance of curative-intent treatment. Second, patients may be fitter at presentation. Functional status is one of the most important independent predictors of survival. Lung cancer is caused by smoking in 80-85% of cases. Patients who do not have smoking-attributable lung cancer are often diagnosed late. So it is important to refer patients who have persistent symptoms either for chest X-ray, or when symptoms persist and no alternative diagnosis is found, refer for consideration of CT.
 |
|Diagnosing asthma in school-age children can prove challenging
20 Dec 2022
Asthma is the most common chronic respiratory condition affecting children in the UK. There is no single gold standard test to confirm the diagnosis and both overdiagnosis and underdiagnosis are common. Asthma should be suspected in any child presenting with episodes of wheeze, especially recurrent episodes of wheeze. Clinical diagnosis alone often results in misdiagnosis; all children from the age of five years under investigation for asthma in primary care should have access to spirometry, bronchodilator reversibility and FeNO testing.
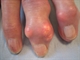 |
|Treat-to-target urate-lowering therapy: the cornerstone of gout management
25 Oct 2022
Gout is a common complex disorder resulting from variable interaction between genetic, constitutional, and environmental factors. Heritability of gout is around 60%, and individual dietary factors account for < 1% of serum urate (SU) variance compared with 24% from the genetic variations currently identified. The most common presentation is a gout flare, characterised by acute onset of one or occasionally more hot, red, swollen joints which are extremely painful. Treat-to-target urate-lowering therapy aims to reduce and maintain urate levels in peripheral joint tissues well below saturation (SU < 360 µmol/L). This prevents further crystal formation and gradually dissolves away existing crystals, after which no further flares occur, and further risk of crystal-induced joint damage is removed.
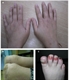 |
|Prompt diagnosis key in improving outcomes in psoriatic arthritis
25 Oct 2022
If left untreated psoriatic arthritis (PsA) can result in progressive, irreversible joint damage causing chronic pain and disability. It is a chronic, autoimmune inflammatory condition that can affect up to 30% of patients with psoriasis. PsA is a multisystem disease affecting other organs such as the eyes, gut and tendons. It is associated with multiple comorbidities such as diabetes mellitus, cardiovascular disease and metabolic syndrome. If PsA is suspected in primary care, routine blood tests should be requested to check for anaemia of chronic disease and raised inflammatory markers. Plain radiographs of hands and feet should be requested prior to referral, although classical changes do not occur early in the disease. If GPs suspect PsA, prompt referral is paramount. Patients should be referred if they have persistent joint symptoms, a positive screening questionnaire (PEST), joint swelling, dactylitis or enthesitis, and/or inflammatory back pain.
Special reports
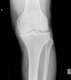 |
|Optimising the management of osteoarthritis
20 Dec 2022
History and examination are sufficient to diagnose osteoarthritis (OA) in most cases. Joint pain and stiffness (lasting no longer than 30 minutes in the morning), which is worse with weight bearing or usage, in a patient aged 45 or over, is indicative of OA. Muscle strengthening and aerobic exercise remain core treatments and exercise should be tailored to the individual. Pharmacological therapy should be used ‘at the lowest effective dose for the shortest possible time’ in combination with non-pharmacological therapy. Referral for joint replacement should be based on severity of symptoms and failure of conservative treatment, and should not be influenced by factors such as age, gender or comorbidities.
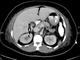 |
|Prompt recognition and treatment crucial in pyelonephritis
20 Dec 2022
Acute pyelonephritis is a bacterial infection of the kidney parenchyma that can cause organ damage and be life-threatening. It is associated with systemic symptoms and flank pain which are not usually present in lower urinary tract infections. Early recognition and aggressive management of sepsis is required to prevent serious complications. Patients should be urgently referred to the emergency department if they are unwell and showing signs of sepsis (hypotension, tachycardia, hypothermia or pyrexia, signs of systemic illness such as rigors). Patients at higher risk of severe disease (elderly comorbid patients or those in other risk groups) may also warrant urgent referral.
 |
|Management of chronic mild to moderate asthma in adults
25 Oct 2022
Although classically asthma is characterised by variable airflow obstruction and inflammation, leading to symptoms of breathlessness, wheeze, chest tightness and cough, it can present with a broad spectrum of symptoms that have a wide differential diagnosis. Clinical examination is frequently entirely normal and clinical history alone is not sufficient to diagnose asthma. There is over-reliance on short-acting beta-agonists and a widespread underuse of inhaled corticosteroids. In mild to moderate disease, fluctuating symptoms can lead to an over-reliance on short-acting reliever treatment at the expense of preventative inhaled steroids. This risks the concealment of deteriorating symptoms and the potential build-up of critical airways inflammation.
 |
|Diagnosis and management of type 1 diabetes in adults
26 Sep 2022
Autoimmune destruction of the pancreatic beta cells leads to onset of type 1 diabetes (T1D). Although T1D can occur at any age, 85% of patients are diagnosed under the age of 20. Patients usually present with typical features of thirst, polyuria, weight loss and hyperglycaemia, with or without ketosis. In adults, symptoms are similar to those in children but there is a wider differential diagnosis. The presence of certain other autoimmune diseases, in the patient or relatives, is highly suggestive of an autoimmune cause of diabetes.
 |
|Improving outcomes in preterm labour and birth
26 Sep 2022
Preterm birth is a key determinant of adverse infant outcomes. A previous preterm birth is the single most important risk factor; however, the majority of preterm births occur in first time mothers. Modifiable risk factors should be identified and addressed, both opportunistically during prepregnancy consultations and at the booking visit. Women at high and moderate risk of preterm birth should be identified at the booking visit and referred to the local or tertiary preterm birth prevention clinic by 12 weeks.
Thorough assessment central to management of low back pain
27 Jul 2022
Low back pain is a symptom with a range of possible causes. Most cases are either mechanical in origin or neurogenic. However, rarer secondary causes must also be considered to ensure serious pathology is not missed. A focused musculoskeletal and neurological examination should be carried out. If both red flag symptoms and radicular features are absent, the back pain is likely to be of mechanical origin and in many cases will resolve with simple management.
Care of the elderly
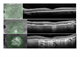 |
|Diagnosis and management of age-related macular degeneration
25 Jan 2021
Age-related macular degeneration (AMD) is a cause of painless, gradual loss of vision. Epidemiological evidence suggests 4-8% of people aged over 65 years in the UK have visually significant AMD. Patients with suspected neovascular AMD (NvAMD) should be seen by ophthalmology within two weeks, and if the diagnosis and progressive disease are confirmed, treatment should commence within the same timeframe. Intravitreal anti-vascular endothelial growth factor (anti-VEGF) agents cause regression of neovascularisation and reduce macular oedema. There is no treatment for dry AMD.
Diagnosing anxiety disorders in older adults can be challenging
25 Jan 2021
In older adults, the prevalence of anxiety disorders is higher among those with other health problems, and those in hospital and care settings. A primary depressive disorder should be excluded whenever an older person presents with anxiety symptoms for the first time, and comorbid anxiety often indicates a more severe presentation of depression. Around four in five patients have a comorbid physical disorder. Medical conditions can mimic symptoms of, predispose to, or even directly precipitate an anxiety disorder, and may colour its symptomatology or limit treatment options.
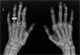 |
|Elderly onset RA: a diagnostic and therapeutic challenge
23 Jan 2020
Elderly onset rheumatoid arthritis (EORA) is defined as rheumatoid arthritis (RA) with age of first onset 65 years or over. It comprises an acute onset proximal or large joint arthritis with a prominent systemic syndrome characterised by constitutional symptoms and a higher ESR than in the younger patient with RA. Investigations should focus on trying to establish the cause and ruling out differential diagnoses. They should include inflammatory markers, serum uric acid, full blood count, rheumatoid factor/anti-CCP antibodies, and X-rays of the affected joint as well as the hands and feet. The possibility of malignancy should always be borne in mind. NICE recommends urgent referral of all suspected cases.
Musculoskeletal medicine
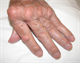 |
|Treating to target will optimise long-term outcomes in RA
24 Nov 2020
Rheumatoid arthritis (RA) classically causes a symmetrical, small joint polyarthritis which left untreated can lead to joint destruction and deformity. NICE recommends that any adult with suspected persistent synovitis of undetermined cause should be referred for a specialist opinion. Patients should be referred urgently (even with a normal acute-phase response, negative anti-CCP antibodies or rheumatoid factor) if any of the following apply: the small joints of the hands or feet are affected; > 1 joint is affected; there has been a delay of ≥ 3 months between onset of symptoms and seeking medical advice.
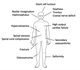 |
|Diagnosis and management of Paget’s disease of bone
24 Nov 2020
Paget’s disease of bone is a metabolic disease in which focal abnormalities of bone remodelling occur in one or more skeletal sites. The affected bones enlarge and may become deformed and this can lead to complications including bone pain, pathological fractures, secondary osteoarthritis, deafness and nerve compression syndromes. The three main risk factors are age, male gender and family history. People with a first-degree relative with Paget’s disease have a seven-fold increased risk of developing the disease. Patients who have bone deformity or symptoms that might be due to Paget’s disease should be referred to secondary care.
Gastroenterology
 |
|Early treatment can arrest or reverse cirrhosis
24 Jul 2020
Around 60,000 people in the UK are estimated to have cirrhosis. It is now the third most common cause of premature death. Decompensation represents a watershed moment for patients with cirrhosis, with the median survival falling from > 12 years for compensated cirrhosis to approximately two years. Patients with cirrhosis should undergo six-monthly ultrasound to screen for the early development of primary hepatocellular carcinoma. They should also undergo an initial upper gastrointestinal endoscopy to screen for varices.
 |
|Tailor treatment to the patient with gallstone disease
24 Jul 2020
Gallstones affect around 15% of adults in the UK. Between 50 and 70% of patients with gallstones are asymptomatic at diagnosis and only 10-25% of these individuals will go on to develop symptomatic gallstone disease. The vast majority (90-95%) of gallstones are cholesterol stones. Obesity is associated with an increased risk of symptomatic gallstones. Patients with symptoms suggestive of gallstones should be offered liver function tests and an abdominal ultrasound.
Psychiatry
 |
|Early recognition key in child and adolescent anxiety disorders
23 Apr 2020
Anxiety disorders are common, highly treatable conditions, with a strong evidence base for cognitive behaviour therapy. In a recent population sample of the under 12s, only 65% of those who met criteria for a diagnosis of an anxiety disorder had sought professional help and only 3.4% had received an evidence-based treatment. Assessment should include an exploration of neurodevelopmental conditions, drug and alcohol misuse, and speech and language problems.
 |
|Treating psychological trauma in the real world
23 Jan 2020
After a potentially traumatic event (PTE), many individuals experience either no distress or only transient distress, while others suffer considerable morbidity and may develop post-traumatic stress disorder (PTSD). Around one-third of people experiencing a PTE will develop PTSD, though this varies depending on the type of traumatic event and rates of PTSD are higher with type 2 trauma. Type 2 trauma involves repeated traumatic experiences over extended periods. Although PTSD symptoms can be present acutely, the diagnosis requires the persistence of symptoms for at least one month and the symptoms should cause functional impairment.
Neurology
Detailed history the cornerstone of epilepsy diagnosis
24 Sep 2020
The incidence of epilepsy in the UK is estimated to be 50 per 100,000 per year and up to 1% of the population have active epilepsy. The diagnosis of epilepsy will usually be made in a neurology clinic. A generalised seizure as part of a generalised epilepsy syndrome may occur without warning but may be preceded by blank spells or myoclonic jerks. A generalised seizure with focal onset may be preceded by an aura. Brain imaging is required in almost all cases where epilepsy is suspected, the only possible exception being people with generalised epilepsies proven on EEG. MRI is the imaging modality of choice.
 |
|GPs should be vigilant for acute deterioration in myasthenia gravis
24 Sep 2020
Myasthenia gravis is an autoimmune disorder of neuromuscular junction transmission. It is relatively rare, with an approximate annual incidence of 1 per 100,000 population, and prevalence of 15 per 100,000 population in the UK. An ocular presentation may include fatiguing ptosis or diplopia. Typically, symptoms ‘fatigue’ (the physical power of the muscle deteriorates rapidly with repeated activity) and become more noticeable as the day progresses. More generalised symptoms include fatiguing difficulty with speech or swallowing. There may be fatiguing weakness of the arms and legs. The diagnosis will usually be confirmed by referral to a neurologist.
Women's health
 |
|GPs have a key role in the management of miscarriage
22 Mar 2021
First trimester miscarriage affects up to one in four pregnancies. While some women will experience bleeding and pain, others have no symptoms and are given the diagnosis at their 12-13 week booking scan. In 50-85% of cases the cause is due to a spontaneous chromosomal abnormality, most commonly trisomy. Many women suffer from psychological sequelae including PTSD, anxiety and depression. GPs should offer a follow-up appointment to all women who have had a miscarriage to: discuss any questions the woman has regarding her miscarriage; assess the woman’s psychological wellbeing and offer counselling if appropriate.
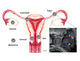 |
|Have a high index of suspicion for ectopic pregnancy
24 Mar 2020
Ectopic pregnancy is estimated to occur in 1-2% of all pregnancies and continues to be the leading cause of maternal mortality in early pregnancy. Most ectopic pregnancies are located within the fallopian tube and carry a risk of tubal rupture and intra-abdominal bleeding. Women with ectopic pregnancy can present in a wide variety of ways, from acute collapse following rupture to asymptomatic and unaware that they are pregnant. Symptoms may include vaginal bleeding and abdominal pain. There may also be non-specific symptoms such as Gl and urinary symptoms, rectal pressure, dizziness, shoulder tip pain, fainting or syncope.
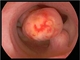 |
|Investigating the cause of heavy menstrual bleeding
25 Mar 2019
Heavy menstrual bleeding has been defined as ‘excessive menstrual blood loss which interferes with a woman’s physical, social, emotional, and/or material quality of life’. Heavy menstrual bleeding affects 25% of women of reproductive age and is estimated to be the fourth most common reason for gynaecological referrals. Women should be asked about pelvic pain which might suggest endometriosis and pressure symptoms which might suggest significant fibroids. Examination is appropriate if there is intermenstrual or postcoital bleeding and, if the woman is actively bleeding, may identify the source of the bleeding.
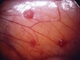 |
|Symptom recognition key to diagnosing endometriosis
22 Mar 2018
Endometriosis affects around one in ten women of reproductive age in the UK. NICE guidance highlights the importance of symptoms in its diagnosis. A normal abdominal or pelvic examination, ultrasound, or MRI should not exclude the diagnosis. Endometriosis should be suspected in women and adolescents who present with one or more of: chronic pelvic pain, significant dysmenorrhoea, deep dyspareunia, period-related or cyclical GI or urinary symptoms, or infertility. If endometriosis is suspected or symptoms persist, patients should be referred for further assessment.
A hundred and fifty years ago
 |
|150 years ago: Dr Anstie’s death and his last teaching in sanitary work
20 Dec 2022
Dr Anstie, during the examination of a septic corpse from the Royal Victoria Patriotic Asylum for Girls, received the puncture which killed him at the age of 41 years. The day after the puncture the writer of this article had a long conversation with him on the state of things which Dr Anstie had observed at this asylum. He made no reference to the wound he had received, and which must then have been beginning to work out its fatal consequences; and the writer left him impressed with the enthusiasm with which he had entered upon a difficult task. His death, a related consequence of the neglect against which he protested, gives a melancholy interest to this his last teaching in sanitary work.
 |
|150 years ago: Chloral: a wolf in sheep’s clothing
25 Oct 2022
Formerly, if Englishmen or Englishwomen had a certain amount of pain, or worry, or sleeplessness, they endured it, and hoped for better times – an opiate being considered a serious matter by most persons. At present the list of available soothers of pain and restlessness has become much larger; and from time to time fresh substances are discovered to possess the required power, and are at first stated to be also ‘quite harmless’. This was especially the case with chloral; but that drug has proved itself a wolf in sheep’s clothing with a vengeance.
Cancer
Maintain a high index of suspicion for kidney cancer
25 Apr 2022
More than 50% of renal cell carcinoma (RCC) cases are detected incidentally on imaging, often at a late stage. Patients may present with mass-related localised symptoms, constitutional symptoms and symptoms of metastatic disease. Ultrasound is the optimal initial investigation to screen individuals with suspected RCC. NICE recommends that patients aged 45 and over with isolated haematuria, in the absence (or following treatment) of a urinary tract infection, are referred for investigation of a potential renal malignancy.
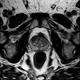 |
|Improving the early detection and management of prostate cancer
25 Apr 2022
Prostate cancer is the most common cancer in men in the UK. In men with possible symptoms of prostate cancer, an assessment of LUTS, relevant risk factors and past medical history is essential. NICE recommends performing a DRE; this will give an impression of prostate size. If the prostate feels malignant on DRE this should trigger a fast-track referral to secondary care, via a suspected cancer pathway referral even if the PSA is normal. A PSA test should also be offered to men with LUTS or an abnormal DRE.
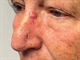 |
|Risk stratification key to management of basal cell carcinoma
27 Oct 2021
Basal cell carcinoma (BCC) is a slow growing, locally invasive malignant epidermal skin tumour. Metastases are very rare and morbidity results from the localised destruction of tissue particularly on the head and neck. Suspected high-risk BCCs on the central face (around the eyes, nose, lips and ears) should be referred for an urgent opinion. BCCs most commonly present on the head and neck and sun-exposed sites but may occur at any body site. Patients will often report a non-healing wound that recurrently bleeds, crusts and scabs but does not heal.
 |
|Early detection of cutaneous melanoma improves prognosis
24 Sep 2021
Exposure to intermittent intense sunlight and sunburn (especially in childhood) are the most common modifiable risk factors for melanoma. Individuals with lighter skin tones are at greatest risk (Fitzpatrick skin types I-II). A history of melanoma increases the risk of a further melanoma eight-fold. Approximately 5-10% of melanoma cases are estimated to be familial. The 7-point checklist is recommended by NICE to help determine when a referral is indicated. However, checklists should not be used in isolation as some melanomas will be missed. Amelanotic melanomas, estimated at 10% of all melanomas, remain a challenge.
Prevention, diagnosis and treatment of colorectal cancer
26 Jul 2021
Colorectal cancer is the third most common cancer in both women and men and is the second most common cause of cancer death in the UK. The main symptoms patients with colorectal cancer present with are: persistent blood in faeces; persistent change in bowel habit and persistent lower abdominal pain. Less obvious presentations are unexplained weight loss, tiredness for no reason, general malaise and iron deficiency anaemia found on blood testing.
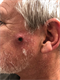 |
|Improving the detection of cutaneous squamous cell carcinoma
25 Jun 2021
Cutaneous squamous cell carcinoma (cSCC) can develop de novo or from pre-existing chronic actinic damage, although the probability and speed of transition from actinic keratosis to cSCC is highly variable. The occurrence of cSCC is related to chronic UV exposure, particularly occupational exposure. Risk factors include fairer skin, significant exposure to sunlight or PUVA. Incidence is also significantly increased in patients who are immunosuppressed. All patients with suspected cSCC should be referred via the two-week wait pathway to dermatology.
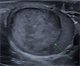 |
|GPs should have a high index of suspicion for testicular cancer
22 Apr 2021
Most men with testicular cancer present with a lump that they have identified in their scrotum. Although the scrotal swelling is usually painless, pain is the first symptom in around 20% of patients, typically a dull or dragging ache in the testicle or a heaviness in the scrotum. NICE recommends that all men who have a non-painful enlargement or change in shape or texture of their testis should be referred urgently to urology using the two-week wait pathway. In men who have unexplained or persistent testicular symptoms, an urgent direct access testicular ultrasound scan should be requested.
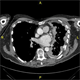 |
|Diagnosis and management of malignant pleural mesothelioma
21 Dec 2020
Mesothelioma accounts for less than 1% of all cancers in England, Wales and Northern Ireland. There are almost 2,500 new diagnoses a year, of which 96% are pleural. The median age at diagnosis for malignant pleural mesothelioma (MPM) is 76 years. The majority of cases occur in men, most commonly following occupational exposure to asbestos. There is a latent period, usually 30-40 years, between exposure and disease development. A chest X-ray is usually the first-line investigation; 94% of patients with MPM have a unilateral pleural effusion, although the chest X-ray may be normal or show another asbestos-related lung disease.
.jpg) |
|Time to diagnosis key in improving lung cancer outcomes
25 Nov 2019
NICE recommends urgent referral via a suspected cancer referral pathway to the two week wait service if: chest X-ray findings suggest lung cancer or if patients aged 40 and over have unexplained haemoptysis. However, studies have indicated that around 20-25% of patients with confirmed lung cancer may have a chest X-ray reported as normal and this figure may be higher for early stage lung cancers. Therefore, the National Optimal Lung Cancer Pathway recommends that where there is a high suspicion of underlying malignancy (but the chest X-ray is normal), GPs should refer patients directly for a CT scan.
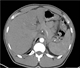 |
|Early detection of liver cancer key to improving outcomes
07 Aug 2019
Hepatocellular carcinoma (HCC) accounts for around 90% of liver cancer cases and intrahepatic cholangiocarcinoma (CC) for 9-10%. Most cases of HCC occur in the context of chronic liver disease with cirrhosis, particularly in those with chronic hepatitis B or C. Other major risk factors include excessive alcohol consumption, obesity and aflatoxins. Overall, 10-15% of cirrhotic patients will develop HCC within 20 years. Patients presenting with an upper abdominal mass consistent with an enlarged liver should be referred for an urgent direct access ultrasound scan within two weeks.
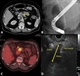 |
|Improving outcomes in pancreatic cancer
25 Jul 2018
The combination of an aggressive disease, vague presenting symptoms and insensitive standard diagnostic tests is a key factor contributing to poor outcomes with only 15% of patients with pancreatic cancer having operable disease at diagnosis. The NICE guideline on referral for suspected cancer recommends urgent referral via a suspected cancer pathway referral if the patient is aged 40 and over with jaundice. It also recommends that an urgent direct access computerised tomography (CT) scan referral should be considered in patients aged 60 and over with weight loss and any of the following: diarrhoea; back pain; abdominal pain; nausea; vomiting; constipation; new onset diabetes. Pancreatic cancer requires a CT scan for diagnosis.
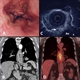 |
|Diagnosis and management of oesophageal cancer
22 Feb 2018
Oesophageal cancer commonly presents with dysphagia or odynophagia and can be associated with weight loss and vomiting. Referral for urgent endoscopy should always be considered in the presence of dysphagia regardless of previous history or medication. NICE recommends urgent referral (within 2 weeks) for direct access for upper GI endoscopy in patients with dysphagia and those aged 55 years or over with weight loss and any of the following: upper abdominal pain, reflux, or dyspepsia.
HASLAM's view
 |
|You don’t have to be solemn to be serious
20 Dec 2022
My dad was a GP. He died when I was a young teenager, and I will never forget his funeral - the huge number of patients who came to say a silent thank you. He was an immense inspiration to me and my career, and one of my abiding memories of him at work as a doctor involves The Practitioner.
 |
|Try sitting in the patient’s chair
25 Oct 2022
If you haven’t tried sitting in the patient’s chair in your consulting room, give it a try. You might be surprised at how it feels.
 |
|Understanding our patients’ priorities is key
26 Sep 2022
‘What would you do, doctor?’ is a question we should be very cautious about answering, without understanding a great deal about the patient’s health beliefs and priorities.
 |
|When music is the best therapy
27 Jul 2022
The great neurologist and author Oliver Sacks once put it perfectly. 'Music can lift us out of depression or move us to tears – it is a remedy, a tonic .... But for many of my neurological patients, music is even more – it can provide access, even when no medication can, to movement, to speech, to life.'
 |
|How do you tackle stress?
24 Jun 2022
Some years ago, I tried using a simple stress diary when I was going through a particularly rough patch. The technique may sound like some sort of Californian psychobabble, but it certainly helped me.
Editorials
 |
|Is there an optimum time of day to take antihypertensive medication?
20 Dec 2022
Evening dosing of antihypertensive medication does not improve major cardiovascular outcomes compared with morning dosing in patients with hypertension, a large UK clinical trial, published in the Lancet, has found.
 |
|Is there a long-term legacy effect of intensive blood pressure control?
25 Oct 2022
The Systolic Blood Pressure Intervention Trial (SPRINT) found that in patients with hypertension who were at increased cardiovascular risk, intensive control (lowering systolic blood pressure (SBP) to < 120 mm Hg) resulted in significant cardiovascular benefit, reducing the risk of incident CVD and all cause mortality, compared with routine BP control (lowering SBP to < 140 mm Hg). However, a secondary analysis showed that this benefit did not persist after completion of the trial.
A hundred years ago
 |
|100 years ago: Sudden death by emotional shock
20 Dec 2022
An event which might cause momentary anxiety to one individual may cause profound dread to another, and hence it is very difficult to state categorically that such and such an event could not possibly have led to the death of an individual. The emotions act very differently in different persons, and again in the same person they act dissimilarly at different times. A healthy woman who was brushing her teeth accidentally swallowed a mouthful of harmless mouth-wash, and died from fright, under the belief that it was poisonous. The bursting into her bedroom in the middle of the night by an insane Irishman in a state of nudity caused the death of a healthy woman of 48 years.

