CPD frameworks
These frameworks, associated with all articles, prompt drafting of personal learning, reflection and planning.
Save your reflective note into your device or cloud
Fillable PDF frameworks
Adobe reader needed for tablets
Word frameworks - for reflective practice
Click to download
Reflection on a journal article
Stages of reflection on a situation
Reflection of a team, practice or group
External reference on reflection
Reflective practice in health care and how to reflect effectively
Koshy K, Limb C et al. International Journal of Surgical Oncology. 2017 2:e20
Symposium articles
Each month there is a themed symposium in The Practitioner. The articles are written by specialists and a named GP adviser reviews the articles to ensure their relevance to general practice and to select material that is highlighted in a key points panel. Every year the following specialties are featured in symposia:
• Care of the elderly • Renal medicine • Women's health • Men's health • Psychiatry • Paediatrics • Gastroenterology • Neurology • Cardiovascular medicine • Respiratory medicine • Musculoskeletal medicine
 |
|Diagnosing asthma in school-age children can prove challenging
20 Dec 2022
Asthma is the most common chronic respiratory condition affecting children in the UK. There is no single gold standard test to confirm the diagnosis and both overdiagnosis and underdiagnosis are common. Asthma should be suspected in any child presenting with episodes of wheeze, especially recurrent episodes of wheeze. Clinical diagnosis alone often results in misdiagnosis; all children from the age of five years under investigation for asthma in primary care should have access to spirometry, bronchodilator reversibility and FeNO testing.
Early diagnosis the main driver to improving outcomes in lung cancer
20 Dec 2022
Earlier diagnosis of lung cancer improves outcomes for two main reasons. First, the disease stage may be earlier allowing more chance of curative-intent treatment. Second, patients may be fitter at presentation. Functional status is one of the most important independent predictors of survival. Lung cancer is caused by smoking in 80-85% of cases. Patients who do not have smoking-attributable lung cancer are often diagnosed late. So it is important to refer patients who have persistent symptoms either for chest X-ray, or when symptoms persist and no alternative diagnosis is found, refer for consideration of CT.
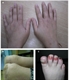 |
|Prompt diagnosis key in improving outcomes in psoriatic arthritis
25 Oct 2022
If left untreated psoriatic arthritis (PsA) can result in progressive, irreversible joint damage causing chronic pain and disability. It is a chronic, autoimmune inflammatory condition that can affect up to 30% of patients with psoriasis. PsA is a multisystem disease affecting other organs such as the eyes, gut and tendons. It is associated with multiple comorbidities such as diabetes mellitus, cardiovascular disease and metabolic syndrome. If PsA is suspected in primary care, routine blood tests should be requested to check for anaemia of chronic disease and raised inflammatory markers. Plain radiographs of hands and feet should be requested prior to referral, although classical changes do not occur early in the disease. If GPs suspect PsA, prompt referral is paramount. Patients should be referred if they have persistent joint symptoms, a positive screening questionnaire (PEST), joint swelling, dactylitis or enthesitis, and/or inflammatory back pain.
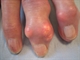 |
|Treat-to-target urate-lowering therapy: the cornerstone of gout management
25 Oct 2022
Gout is a common complex disorder resulting from variable interaction between genetic, constitutional, and environmental factors. Heritability of gout is around 60%, and individual dietary factors account for < 1% of serum urate (SU) variance compared with 24% from the genetic variations currently identified. The most common presentation is a gout flare, characterised by acute onset of one or occasionally more hot, red, swollen joints which are extremely painful. Treat-to-target urate-lowering therapy aims to reduce and maintain urate levels in peripheral joint tissues well below saturation (SU < 360 µmol/L). This prevents further crystal formation and gradually dissolves away existing crystals, after which no further flares occur, and further risk of crystal-induced joint damage is removed.
Diagnosis and management of epilepsy in adults
26 Sep 2022
According to the International League Against Epilepsy, epilepsy can be diagnosed if any of the following criteria are met: at least two unprovoked seizures occurring on separate days (seizures within 24 hours count as one event); one unprovoked seizure with at least a 60% risk of recurrence over the next ten years on the basis of associated clinical factors (such as a recent stroke or brain tumour); diagnosis of a specific epilepsy syndrome. Convulsive events should be described rather than given a label. The EEG can establish the diagnosis of epilepsy and distinguish between focal and primary generalised epilepsy. An MRI brain scan is usually mandatory.
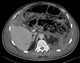 |
|Prompt diagnosis and treatment will improve outcomes in acute pancreatitis
27 Jul 2022
Any patient presenting with acute abdominal pain should be assessed for a possible diagnosis of acute pancreatitis. A thorough history of the presenting illness is needed to determine the onset, duration, progress and nature of the pain. In acute pancreatitis the pain typically presents as severe epigastric pain radiating to the back and is worsened by movement, and classically leaning forwards alleviates the pain.
Managing cardiovascular risk key in non-alcoholic fatty liver disease
27 Jul 2022
Most people living with non-alcoholic fatty liver disease (NAFLD) are thought to remain undiagnosed and many are asymptomatic. Obesity, hypertension, type 2 diabetes and hyperlipidaemia are risk factors for NAFLD, and NAFLD is considered to be the liver component of metabolic syndrome. Cardiovascular risk should be stratified for all NAFLD patients and any cardiovascular risk factors managed aggressively. Patients should be given lifestyle advice aimed at weight loss and increased physical activity.
 |
|Assessing and managing depression in patients with dementia
24 Jun 2022
The relationship between depression and dementia is complex. Depression appears to be an independent risk factor for incident dementia, conferring a two-fold increase in dementia risk. Depression may represent an early sign or prodromal feature of dementia. The association between depression and dementia appears to strengthen as the interval between the two disorders shortens. Depression may also be a consequence of dementia.
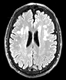 |
|Diagnosis and management of vascular dementia
24 Jun 2022
Vascular dementia describes chronic progressive impairment of cognitive function arising from cerebrovascular injury. The presentation of vascular dementia is often insidious, with disorganisation, loss of drive, irritability, mental rigidity, difficulties with planning and problem solving, emotional lability and other mood changes, and sometimes inappropriate or disinhibited social behaviour. Physical examination may identify gait impairment, bradykinesia, rigidity, and focal neurological signs.
Optimising the recognition of Lewy body dementia
25 May 2022
Lewy body dementia is a heterogeneous condition that is often difficult to treat. It is associated with higher rates of neuropsychiatric symptoms, inpatient admission and carer stress, as well as shorter survival, than other dementia subtypes. Core clinical features are: fluctuating cognition with pronounced variations in attention and alertness; recurrent visual hallucinations; REM sleep behaviour disorder; one or more features of spontaneous parkinsonism. Recurrent visual hallucinations occur in up to 80% of patients.
 |
|Diagnosis and management of acute coronary syndrome
25 May 2022
The term acute coronary syndrome (ACS) describes a range of conditions, including unstable angina, non-ST-elevation myocardial infarction (NSTEMI) and ST-elevation myocardial infarction (STEMI), which are associated with a sudden reduction of blood flow to the heart. Its presentation is broad, and can include chest pain, cardiac arrest, haemodynamic instability, or cardiogenic shock. Urgent assessment of patients presenting with chest pain is crucial to the outcome as ACS treatment is time sensitive.
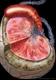 |
|Prompt diagnosis of epididymo-orchitis can prevent complications
25 Apr 2022
Epididymo-orchitis is an inflammation of the testis and epididymis, generally of infectious origin. In young men epididymo-orchitis is most often associated with sexually transmitted infections. In those aged over 35 the causative pathogens are more likely to be non-sexually transmitted coliform organisms associated with urinary tract infections. Other causes include viral infections such as mumps in immunocompromised, non-immunised or prepubescent males, local trauma, and medication such as amiodarone.
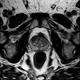 |
|Improving the early detection and management of prostate cancer
25 Apr 2022
Prostate cancer is the most common cancer in men in the UK. In men with possible symptoms of prostate cancer, an assessment of LUTS, relevant risk factors and past medical history is essential. NICE recommends performing a DRE; this will give an impression of prostate size. If the prostate feels malignant on DRE this should trigger a fast-track referral to secondary care, via a suspected cancer pathway referral even if the PSA is normal. A PSA test should also be offered to men with LUTS or an abnormal DRE.
 |
|Complications following termination of pregnancy
25 Mar 2022
Serious complications during or after termination of pregnancy are rare. However, they can be associated with significant morbidity and mortality, and occasionally can complicate future pregnancies. The risk of pelvic infection is around 10% and this is usually due to exacerbation of a pre-existing infection. The most common causes of bleeding include: retained products of conception; infection and trauma to the cervix or uterus, especially at > 10 weeks’ gestation.
GPs have key role in identifying women at risk of pre-eclampsia
25 Mar 2022
Pre-eclampsia is an important cause of maternal morbidity and mortality. It is a multisystem disorder of pregnancy characterised by new onset hypertension after 20 weeks’ gestation, usually accompanied by proteinuria. If a urine dipstick is positive for protein, the amount should be quantified: a protein: creatinine ratio = 30 mg/mmol is abnormal. There should be a high index of suspicion for pre-eclampsia if there is biochemical disturbance consistent with the diagnosis or evidence of fetal growth restriction when plotted on a customised growth chart.
 |
|Diagnosis and management of osteogenesis imperfecta
24 Feb 2022
Osteogenesis imperfecta is a group of rare inherited skeletal disorders characterised by a greatly increased risk of fragility fractures. The reduction in bone strength is due to defects in its material properties and mineralisation. Low trauma fractures typically start in infancy e.g. as a consequence of falling when learning to walk. Rarely mild osteogenesis imperfecta can present for the first time during adulthood. Diagnosis is primarily clinical, based on a history of multiple low trauma fractures during infancy and childhood, and other clinical features.
Optimising the management of children with cystic fibrosis
24 Feb 2022
Cystic fibrosis (CF) is an autosomal recessive disorder resulting from two disease-causing mutations in the cystic fibrosis transmembrane regulator (CFTR) gene located on chromosome 7. CFTR is a chloride and bicarbonate channel found in sweat glands and the epithelial cells of the respiratory and digestive tracts. CF is the most common life-limiting genetic disorder in the UK, diagnosed in one in every 2,500 babies. The median age of death in the UK has been rising steadily and is 36 years. Most deaths in young people are the result of rapidly progressing lung disease. Use of CFTR modulators has resulted in a step change in CF management, improved lung function and will help to improve survival. CFTR modulator therapy targets the underlying CFTR defect.
GPs should be vigilant for accelerated progression of CKD
24 Jan 2022
Despite being common, CKD often remains undiagnosed partly because of lack of symptoms until late in the disease process. Late detection of CKD, and hence lack of effective management, increases the risk of progression to end-stage renal disease which often requires renal replacement therapy such as dialysis or transplantation. Derangement in serum creatinine and eGFR will alert a clinician to a patient with potential CKD. Timely referral for specialist nephrology input when required is key.
Suspected nephrotic syndrome warrants urgent referral
24 Jan 2022
Nephrotic syndrome results from dysfunctional glomerular filtration and consists of three clinical features: severe proteinuria (> 3.5 g/24 hr); hypoalbuminaemia (serum albumin < 30 g/L); and peripheral oedema. It may occur in people of all ages. If nephrotic syndrome remains uncontrolled even those with normal kidney function at presentation can develop progressive chronic kidney disease. All patients with suspected nephrotic syndrome should be referred urgently to nephrology.
 |
|Managing acute asthma in adults in primary care
20 Dec 2021
Treatment with bronchodilators and oral corticosteroids should be given as soon as possible in an acute asthma exacerbation. In moderate exacerbations, hospital admission is based on multiple factors, including response to initial treatment, known reduction in baseline lung function, history of exacerbations, particularly previous need for critical care involvement, and ability to cope at home. Patients with features of acute severe or life-threatening asthma should be referred to hospital immediately following initial assessment.
Tailor treatment to the patient with COPD
20 Dec 2021
COPD is characterised by persistent respiratory symptoms and airflow limitation that is due to airway and/or alveolar abnormalities usually caused by significant exposure to noxious particles or gases and influenced by host factors including abnormal lung development. Performance and interpretation of spirometry should be based on clinical suspicion of airway disease in a patient with suggestive symptoms and exposures, where a medical history has been taken and examination performed.
Prompt diagnosis and treatment will improve heart failure outcomes
27 Oct 2021
The majority of new diagnoses of heart failure (HF) are made only after the patient has deteriorated to the point of requiring hospital admission. Within a month of admission with HF, 1 in 4 patients who survive to discharge will be readmitted, and 1 in 8 will die. Ischaemic heart disease is the most common cause of HF, accounting for at least half of diagnoses: following a heart attack, 1 in 3 patients will develop HF within 5 years. Hypertension, diabetes and obesity are also associated with an increased risk of HF.
Detecting and managing atrial fibrillation in primary care
27 Oct 2021
Atrial fibrillation (AF) is often diagnosed as an incidental finding during a routine medical check. The prevalence increases with age and the presence of CVD further increases the risk of AF. Around 15-30% of patients with AF are asymptomatic. When patients present to their GP the most common symptoms of AF include: palpitations, chest pain, breathlessness and a reduction in exercise/functional capacity. To establish a diagnosis of AF, rhythm documentation with an ECG showing at least 30 seconds of AF is required.
 |
|GPs should be vigilant for Parkinson’s disease
25 Sep 2021
Parkinson's disease is the second most common neurodegenerative disease. Parkinsonism is defined as bradykinesia in combination with at least one of rest tremor or rigidity. Parkinson's disease is a clinical diagnosis. Examination should include gait and posture, decreased blink rate and a lack of spontaneous facial movements. Speech will be hypophonic. Evidence of a resting tremor should be sought and the patient assessed for joint rigidity and bradykinesia. After initial assessment, prompt referral to a neurologist is important to confirm the diagnosis and discuss management.
 |
|History and examination pivotal in diagnosis of Bell’s palsy
24 Sep 2021
Bell’s palsy is the most common cause of facial palsy and presents as a unilateral lower motor neurone facial weakness in association with sensory and parasympathetic dysfunction. Maximal facial weakness occurs within 72 hours and most cases recover over the following few weeks. It is essential to consider alternative causes of acute peripheral facial palsy including: infection, malignancy and autoimmune disease. Urgent referral to neurology or ENT, depending on local referral pathways, is warranted if there is uncertainty about the diagnosis or there are atypical features.
Prevention, diagnosis and treatment of colorectal cancer
26 Jul 2021
Colorectal cancer is the third most common cancer in both women and men and is the second most common cause of cancer death in the UK. The main symptoms patients with colorectal cancer present with are: persistent blood in faeces; persistent change in bowel habit and persistent lower abdominal pain. Less obvious presentations are unexplained weight loss, tiredness for no reason, general malaise and iron deficiency anaemia found on blood testing.
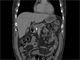 |
|Multidisciplinary care is key in chronic pancreatitis
26 Jul 2021
In chronic pancreatitis chronic inflammation of the pancreas results in irreversible injury and fibrosis. The most common causal factor is excess alcohol consumption. Smoking is an independent risk factor. Gene mutations can lead to hereditary chronic pancreatitis and idiopathic disease, where no clear cause can be identified, accounts for 20-30% of cases. The typical presenting symptom is intermittent or continuous upper abdominal pain which may radiate to the back. The pain is commonly triggered or exacerbated by eating or alcohol consumption.
.png) |
|Juvenile spondyloarthropathies often go unrecognised
25 Jun 2021
Juvenile spondyloarthropathy (JSpA) is an umbrella term encompassing enthesitis-related arthritis, juvenile onset ankylosing spondylitis, juvenile psoriatic arthritis, IBD-related arthritis and reactive arthritis. Initial assessment of any childhood arthropathy should include a full blood count with differentials and inflammatory markers (CRP and ESR), which will be normal in most cases of JSpA, or may reflect a mild inflammatory response and anaemia relating to chronic disease. RF and ANA are characteristically negative. Children with JSpA should be tested for HLA-B27. Children with suspected JSpA should be referred via their GP to a tertiary paediatric rheumatology centre.
 |
|Diagnosis and management of acute asthma in children
25 Jun 2021
Asthma affects 1.1 million children in the UK, and up to 50% experience asthma exacerbations each year. A previous asthma attack is the most important risk factor for future episodes. Modifiable risk factors include poor symptom control, suboptimal treatment regimens, over-reliance on SABAs and poor adherence to preventer therapy. Following an attack all children should receive asthma education as well as an updated personalised asthma action plan. Patients and/or parents must be able to demonstrate correct use of inhalers. A GP review should be carried out within two working days of an asthma attack.
 |
|Diagnosing mild cognitive impairment can prove challenging
25 May 2021
Mild cognitive impairment (MCI) is a heterogeneous clinical syndrome defined as evidence of cognitive decline which is greater than expected for an individual’s age and educational level but which does not significantly impact on activities of daily living. The challenge for clinicians is to distinguish between normal cognition, cognitive decline normal for ageing, subjective cognitive decline, delirium, MCI and dementia. The history should focus on the onset and progression of symptoms. An acute or fluctuating course suggests delirium or another potentially reversible cause.
 |
|Shared care central to management of substance use disorder
25 May 2021
Substance use disorder (SUD) encompasses the use of drugs (illicit and prescription) or alcohol in a way that may cause harm and is difficult to control. Diagnosis is based on clinical history and examination in accordance with ICD-11 criteria which categorise use as hazardous, harmful or dependent. People often see their GP for a medical problem arising from SUD without mentioning substance use. Good rapport and an empathetic attitude can facilitate disclosure.
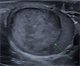 |
|GPs should have a high index of suspicion for testicular cancer
22 Apr 2021
Most men with testicular cancer present with a lump that they have identified in their scrotum. Although the scrotal swelling is usually painless, pain is the first symptom in around 20% of patients, typically a dull or dragging ache in the testicle or a heaviness in the scrotum. NICE recommends that all men who have a non-painful enlargement or change in shape or texture of their testis should be referred urgently to urology using the two-week wait pathway. In men who have unexplained or persistent testicular symptoms, an urgent direct access testicular ultrasound scan should be requested.
 |
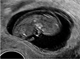
|Thorough assessment key to management of varicocele
22 Apr 2021
Varicoceles are usually asymptomatic but some patients may present with a scrotal swelling or pain. The patient should be examined in both the standing and supine positions, with and without a Valsalva manoeuvre. Patients may also present with primary or secondary infertility, with a varicocele detected on clinical examination or by imaging. Men presenting with infertility should be assessed with a reproductive history, semen analysis and hormone profile, including testosterone, LH and FSH.
 |
|GPs have a key role in the management of miscarriage
22 Mar 2021
First trimester miscarriage affects up to one in four pregnancies. While some women will experience bleeding and pain, others have no symptoms and are given the diagnosis at their 12-13 week booking scan. In 50-85% of cases the cause is due to a spontaneous chromosomal abnormality, most commonly trisomy. Many women suffer from psychological sequelae including PTSD, anxiety and depression. GPs should offer a follow-up appointment to all women who have had a miscarriage to: discuss any questions the woman has regarding her miscarriage; assess the woman’s psychological wellbeing and offer counselling if appropriate.
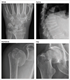 |
|Optimising the assessment and management of osteoporosis
22 Mar 2021
Osteoporosis affects around 40% of women and 13% of men at some point in their lives. While almost any bone can fracture as the result of osteoporosis, the most common sites are the wrist, spine, hip and humerus. The presence of one or more clinical risk factors in individuals aged 50 and over is an indication for a fracture risk assessment. There is a strong evidence base for drug treatment in DXA proven osteoporosis and those with low trauma vertebral fractures.
 |
|Reducing cardiovascular risk pivotal in diabetic kidney disease
21 Feb 2021
Diabetic kidney disease is associated with a very high risk of cardiovascular disease (CVD) and premature mortality from cardiovascular events. There is good evidence that multifactorial interventions that optimise BP, limit proteinuria and minimise cardiovascular risk can reduce morbidity and premature mortality. Early diabetic kidney disease is asymptomatic. Microalbuminuria, defined as a urinary ACR of 3-30 mg/mmol on two occasions three months apart is the earliest clinically detectable indicator of diabetic kidney disease. Excellent glycaemic control can delay onset of microalbuminuria.
Tight blood pressure control key in polycystic kidney disease
21 Feb 2021
Polycystic kidney disease (PKD) has an autosomal dominant mode of inheritance. Despite this 25% of patients will have no known family history and these cases are thought to be due to de novo mutations in the causative genes. PKD can present asymptomatically and should be considered in any patient with renal cysts noted on abdominal imaging, especially if there is a history of hypertension. Patients with PKD may present with hypertension before a decline in eGFR is noted. Cyst haemorrhage, rupture or infection can all present with acute loin pain. PKD can also cause a number of extrarenal complications.
Diagnosing anxiety disorders in older adults can be challenging
25 Jan 2021
In older adults, the prevalence of anxiety disorders is higher among those with other health problems, and those in hospital and care settings. A primary depressive disorder should be excluded whenever an older person presents with anxiety symptoms for the first time, and comorbid anxiety often indicates a more severe presentation of depression. Around four in five patients have a comorbid physical disorder. Medical conditions can mimic symptoms of, predispose to, or even directly precipitate an anxiety disorder, and may colour its symptomatology or limit treatment options.
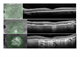 |
|Diagnosis and management of age-related macular degeneration
25 Jan 2021
Age-related macular degeneration (AMD) is a cause of painless, gradual loss of vision. Epidemiological evidence suggests 4-8% of people aged over 65 years in the UK have visually significant AMD. Patients with suspected neovascular AMD (NvAMD) should be seen by ophthalmology within two weeks, and if the diagnosis and progressive disease are confirmed, treatment should commence within the same timeframe. Intravitreal anti-vascular endothelial growth factor (anti-VEGF) agents cause regression of neovascularisation and reduce macular oedema. There is no treatment for dry AMD.
 |
|Improving the management of chronic asthma in children
21 Dec 2020
There is no gold standard test to diagnose asthma. As a result, overdiagnosis and underdiagnosis are common especially when relying on history and clinical examination alone. Spirometry and bronchodilator reversibility testing are particularly useful when a child aged 5 years or older is brought to the practice with symptoms. The validated Asthma Control Test for children aged 12 years and over and the Children’s Asthma Control Test for children aged 4-11 years should be used to assess current asthma control based on four-week recall. Asthma control test scores correlate poorly with lung function and measures of airway inflammation such as FeNO in children and should not be used in isolation.

