Elnaim R, O’Rourke D, Hill C. Prompt recognition and treatment crucial in pyelonephritis. November/December 2022;266(1863):25-27
Prompt recognition and treatment crucial in pyelonephritis
20 Dec 2022
AUTHORS
Dr Razan Elnaim MB BCh BAO, GPST1, Belfast Health and Social Care Trust, Belfast, UK
Dr Declan O’Rourke MB BCh BAO FRCP FRCPath, Consultant Histopathologist, Belfast Health and Social Care Trust and Honorary Professor of Pathology, University of Ulster, Belfast, UK
Dr Christopher Hill MD FRCP, Consultant Nephrologist, Belfast Health and Social Care Trust, Belfast, UK
Competing interests: None
Article
Acute pyelonephritis is a bacterial infection of the kidney parenchyma that can cause organ damage and be life-threatening. It is associated with systemic symptoms and flank pain which are not usually present in lower urinary tract infections. Patients may also have lower urinary tract symptoms. The severity of the illness can vary from relatively mild to patients presenting with septic shock. Initial assessment should always include checking heart rate and BP to determine whether the patient is haemodynamically unstable. A midstream urine sample or catheter specimen of urine should be obtained before initiating antibiotic therapy. However, if pyelonephritis is suspected empirical treatment should not be delayed while waiting for the urine culture result. Early recognition and aggressive management of sepsis is required to prevent serious complications. Patients should be urgently referred to the emergency department if they are unwell and showing signs of sepsis (hypotension, tachycardia, hypothermia or pyrexia, signs of systemic illness such as rigors). Patients at higher risk of severe disease (elderly comorbid patients or those in other risk groups) may also warrant urgent referral.
Acute pyelonephritis is a bacterial infection of the kidney parenchyma that can cause organ damage and be life-threatening.
Acute pyelonephritis has an estimated incidence of 1 in 830 in England. It is six times more common in females than males.1 It is associated with systemic symptoms and flank pain which are not usually present in lower urinary tract infections (UTIs).
Early recognition and aggressive management of sepsis is required to prevent serious complications.
Bacteria usually gain entry to the urinary tract from the perineal region. Infection of the bladder results in symptoms such as dysuria, frequency, and urgency but does not usually result in systemic symptoms. If there is ascending infection into the kidney it is defined as pyelonephritis.
Haematogenous spread of infection to the kidney can occur occasionally (e.g. septic emboli in endocarditis) but is much less common. Risk factors for pyelonephritis are listed in table 1.
Common symptoms and signs
Patients with acute pyelonephritis classically present with the following:
• Pyrexia - temperatures often exceed 38.5°C
• Costovertebral (renal) angle pain and tenderness
• Anorexia, nausea, and vomiting
Patients may also have lower urinary tract symptoms such as frequency, urgency and dysuria. The severity of the illness can vary from relatively mild to patients presenting with septic shock. Initial assessment should always include checking heart rate and blood pressure to determine whether the patient is haemodynamically unstable.
The classic signs and symptoms observed in adults are often absent in children, particularly neonates and infants. In children, two years of age and younger, the most common symptoms of UTI are failure to thrive, feeding difficulty, fever, and vomiting. When fever is present, pyelonephritis should be included in the differential diagnosis.
Elderly patients may present with typical manifestations of pyelonephritis or with non-specific findings such as acute delirium (particularly in those with underlying cognitive impairment).
Diagnosis
Initial diagnosis is based on history and examination. Dipstick urinalysis can be helpful if positive for leucocytes and/or nitrites. It is important to note that some bacteria do not cause nitrite release (e.g. Enterococcus or Pseudomonas species) so it has lower sensitivity but good specificity as a test. Dipstick urinalysis may be less useful in certain patient groups such as those with an indwelling catheter or those aged over 65 years.
In these circumstances, a working diagnosis should be made on the basis of history and examination findings. Common causative organisms for pyelonephritis are shown in table 2.
A midstream urine sample (MSSU) or catheter specimen of urine (CSU) should be obtained before initiating antibiotic therapy. However, if pyelonephritis is suspected empirical treatment should not be delayed while waiting for the urine culture result. It is often difficult to obtain an MSSU from infants so a clean catch specimen is an acceptable alternative.
Imaging is not usually required unless:
• The patient is severely ill
• There is a concern about renal tract obstruction
• There is evidence of acute kidney injury
• The patient has failed to respond despite 48 hours of appropriate antimicrobial therapy
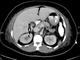
Renal tract ultrasound is useful as an initial step to rule out hydronephrosis. However, CT scanning is the optimal imaging choice for detecting evidence of complications of severe pyelonephritis.2
Management
Patients who are unwell and showing signs of sepsis (hypotension, tachycardia, hypothermia or pyrexia, signs of systemic illness such as rigors) should be urgently referred to the emergency department. Patients who are at higher risk of severe disease (elderly comorbid patients or patients in one of the categories listed in table 1) may also warrant urgent referral.
Empirical antibiotic therapy should be based on local formularies and microbiological guidance. In general, antibiotics such as co-amoxiclav, cefalexin or ciprofloxacin are good oral agents to use if the patient does not require hospitalisation.4 If the patient needs to be admitted to hospital intravenous antibiotics are usually indicated. Most treatment regimens will continue for 7 to 10 days.
Once antibiotic sensitivities are known, antimicrobial therapy can be rationalised if required so it is very important to check the MSSU result. Ideally, patients should be reviewed after 48 hours of initial treatment or earlier if their condition deteriorates. If there is no evidence of improvement at 48 hours, they may require referral to the emergency department.
A negative urine culture result may reflect a number of factors including prior antibiotic therapy or poor sampling technique but it should always prompt a reassessment to ensure there is no alternative diagnosis.
Special cases
Patients with indwelling catheters may always have positive urine cultures due to the development of a biofilm on the catheter's interior surface. CSU samples should only be sent if patients have symptoms and/or signs in keeping with
a likely urinary infection. Indwelling catheters may also need to be changed if pyelonephritis is confirmed to reduce the risk of early recurrence or treatment failure.
Patients who are pregnant may need to be assessed at their maternity unit as pyelonephritis increases the risk of premature labour.
Immunocompromised patients may require longer courses of antibiotics and preferential use of directly bactericidal antibiotics such as beta-lactams, quinolones or aminoglycosides.
In polycystic kidney disease the cysts can become infected and the infection does not behave like typical pyelonephritis. These patients usually require longer courses of antibiotics which will penetrate the wall of the infected cyst.
Early and late complications are shown in table 3.
Chronic pyelonephritis
Recurrent episodes of pyelonephritis, especially in childhood, result in cortical scarring, see figure 2.
Recurrent infections reduce the number of functioning nephrons which, in turn, causes hyperfiltration in the remaining glomeruli. Over time, this causes damage to the glomeruli and eventually glomerulosclerosis. As more glomeruli are damaged, the hyperfiltration injury to the remaining ones increases. In 2020, chronic pyelonephritis accounted for 5.3% of all patients commencing renal replacement therapy (dialysis or kidney transplantation) in the UK.7
Conclusion
Pyelonephritis is usually characterised by flank/renal angle pain, pyrexia, nausea and vomiting. Patients may or may not have lower urinary tract symptoms. It can be severe and result in life-threatening complications.
Early institution of appropriate antimicrobial therapy reduces the risk of complications. Recurrent episodes of pyelonephritis can result in progressive chronic kidney disease.
REFERENCES
1 Chivima B. Pyelonephritis. Nurs Stand 2014;28(23):61
2 National Institute for Health and Care Excellence. Clinical Knowledge Summary: Acute pyelonephritis. NICE. 2021
3 Efstathiou SP, Pefanis AV, Tsioulos DI et al. Acute pyelonephritis in adults: prediction of mortality and failure of treatment. Arch Intern Med 2003;163(10):1206-12
4 National Institute for Health and Care Excellence. NG111. Pyelonephritis (acute): antimicrobial prescribing. NICE. London. 2018
5 Acute pyelonephritis. BMJ Best Practice. https://bestpractice.bmj.com/topics/en-gb/3000111
6 Graversen HV, Nørgaard M, Nitsch D, Christiansen CF. Preadmission kidney function and risk of acute kidney injury in patients hospitalized with acute pyelonephritis:
a Danish population-based cohort study. Plos One 2021;16(3):e0247687
7 UK Renal Registry (2022) UK Renal Registry 24th Annual Report – data to 31/12/2020, Bristol, UK https://ukkidney.org/audit-research/annual-report
ARTICLE IN PDF
EXTERNAL WEBLINKS
For patients

 = Registered users
= Registered users = Paid-up subscribers
= Paid-up subscribers