Ross A, Conaghan PG. Optimising the management of osteoarthritis. Practitioner November/December 2022;266(1863):21-24
Optimising the management of osteoarthritis
20 Dec 2022
AUTHORS
Dr Alexandra Ross BMBS BMed Sci, Clinical Research Fellow, Leeds Institute of Rheumatic and Musculoskeletal Medicine, University of Leeds, Leeds, UK
Professor Philip G. Conaghan MBBS PhD FRACP FRCP, Professor of Musculoskeletal Medicine, Leeds Institute of Rheumatic and Musculoskeletal Medicine, University of Leeds, NIHR Leeds Biomedical Research Centre, Leeds, UK
Competing interests
Professor Philip Conaghan was a member of the development group for the NICE guideline on osteoarthritis (NG226). Dr Alexandra Ross has no competing interests
Acknowledgement
The views expressed in this article are those of the authors and not necessarily those of NICE5
Article
History and examination are sufficient to diagnose OA in most cases. Joint pain and stiffness (lasting ≤ 30 minutes in the morning), which is worse with weight bearing or usage, in a patient aged 45 or over, is indicative of OA. On examination, in small joints there may be tenderness, deformity or Heberden’s or Bouchard’s nodes; in hip joints (where pain is felt in the groin and buttocks), restriction of internal rotation; and in knee joints, effusions (including Baker’s cysts), crepitus and bony enlargement. Muscle strengthening and aerobic exercise remain core treatments and exercise should be tailored to the individual. In overweight patients, there is a dose-response relationship between weight loss and improvement in symptoms, particularly for knee OA. Pharmacological therapy should be used ‘at the lowest effective dose for the shortest possible time’ in combination with non-pharmacological therapy. Referral for joint replacement should be based on severity of symptoms and failure of conservative treatment, and should not be influenced by factors such as age, gender or comorbidities.
The global prevalence of osteoarthritis (OA) has increased more than 100% in the past three decades.1 Standardised prevalence in the UK is 10.7%.2
Both genetic and lifestyle factors are important in OA.3 OA is strongly associated with ageing and has a higher incidence and prevalence in women; approximately 18% of women and 10% of men over 60 have OA.4 The strongest identifiable risk factor is often trauma (e.g. anterior cruciate ligament and meniscus injury in the knee), although the relevant exposure may be repetitive minor trauma over a long period, which may explain the relationship between elite sports or certain occupations and OA.
Obesity and muscle weakness are risk factors for OA pain though it is unclear if they are risk factors for incident OA structural pathology. However, both are important targets for intervention.
Diagnosis
NICE published a new guideline on OA in October 2022.5 History and examination are sufficient to diagnose OA in most cases. Joint pain and stiffness (lasting no longer than 30 minutes in the morning), which is worse with weight bearing or usage in a patient aged 45 years or over, is indicative of OA.
On examination, in small joints there may be tenderness, deformity or Heberden’s or Bouchard’s nodes; in hip joints (where pain is felt in the groin and buttocks), restriction of internal rotation; and in knee joints, effusions (including Baker’s cysts), crepitus and bony enlargement.6
It is important to determine if there is functional muscle loss. Inability to open jars or dropping heavy kettles may signify loss of grip strength, and difficulties getting out of the bath or deep chairs may signify loss of quadriceps strength. These findings may indicate reversible and treatable causes of pain which is likely to be caused by tendinitis/OA.
If there is concern about the possibility of inflammatory arthritis (e.g. because of morning stiffness lasting at least 60 minutes or synovial swelling of hand joints), tests for CRP, anti-CCP antibody and rheumatoid factor should be carried out.
The NICE guideline on rheumatoid arthritis states that adults with persistent synovitis should be urgently referred if the smaller joints of the hands and feet or multiple joints are involved or the patient presents more than three months after the commencement of symptoms even if the above blood tests are normal.7
It is important to bear in mind that while first attacks of gout are often in the big toe and mid-foot, other joints may also be affected so previous episodes of gout should be enquired about. Note that serum urate levels may be unreliable (and can be misleadingly lowered) during acute attacks, although CRP levels will generally be elevated.
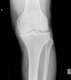
Imaging, especially X-ray, is often not very useful in the diagnosis of OA because of its poor relationship to symptoms.8
Many people with structural abnormalities on X-ray or MRI have no symptoms, so the presence of pathology detected on imaging does not mean this is the cause of symptoms.
Diagnostic tests including imaging may be useful where there is a potential differential diagnosis to consider.
Referral
If a diagnosis of inflammatory arthropathy is considered, patients may require urgent referral to rheumatology for investigations and early treatment, even if blood tests are normal.5
Management of OA involves an inter-disciplinary approach. All patients with OA should be instructed on appropriate muscle strengthening and physical activity, and these should be customised to the individual. This might include referral to physiotherapy, and NICE supports exercise sessions including those where the exercises are part of a treatment package.
Treatment packages involve any of the management options for OA (pharmacological or non-pharmacological) alongside either a behavioural approach or education sessions.
It is important to explain to patients that exercise does not cause further damage in OA and is in fact likely to improve symptoms.
Management
Non-pharmacological therapies
Muscle strengthening and aerobic exercise remain core treatments and exercise should be tailored to the individual.
In overweight patients, there is a dose-response relationship between weight loss and improvement in symptoms, particularly for knee OA, and NICE highlights that 10% weight loss is more likely to achieve greater pain relief than 5%. In addition to improving pain, weight loss is likely to improve function and patients’ quality of life.5 When managing obesity, patients should be advised on ways to improve their diet, with emphasis on nutritional balance and reduced intake for longer term weight change.9
Acupuncture is not recommended by NICE as there is a lack of convincing evidence for efficacy, and potential for adverse effects. Electrotherapies including transcutaneous electrical nerve stimulation (TENS) are now also not recommended.
While walking aids may be helpful for some patients, and help with unsteady gait, there is currently insufficient evidence for the use of other supportive devices such a braces or taping.
The literature in this area is often difficult to interpret, as there are limitations in trial design for devices, for example, difficulty in blinding and much heterogeneity in types of devices.
NICE continues to recommend against the use of glucosamine because of lack of evidence of efficacy. Stem cell therapy is an area of ongoing research and not yet recommended for use in practice.
Pharmacological therapies
Paracetamol is now recommended just for short-term use and when other pharmacological options are not appropriate for the individual; this is based on its lack of efficacy in trials when compared with placebo.
The latest guidance also moves away from the routine use of opioids, because of both limited efficacy data and safety concerns. Strong opioids are not recommended and if weak opioids are used, for example, low-dose codeine, these should only be used short term.
Pharmacological therapy should be used ‘at the lowest effective dose for the shortest possible time’ in combination with the previously mentioned non-pharmacological therapy.
Patients with knee OA may be offered topical NSAIDs and patients with OA affecting other joints may also be offered this despite lesser evidence for other sites. Topical capsaicin has shown some benefits in knee OA but costs more than topical NSAIDs, and no recommendation is made for its clinical use.
Oral NSAIDs reduce pain and are still recommended but should only be used for short-term management because of the risk of adverse effects especially in patients with comorbidities.
The co-prescription of gastroprotective agents should be offered while patients are taking NSAIDs, particularly for those at greater risk of gastrointestinal events.
Intra-articular corticosteroids may be offered as an alternative if the above pharmacological options are not effective, as a shared decision with patients, with the NICE guideline acknowledging that their analgesic effect may be relatively short-lived (only lasting for 2-10 weeks).
No other intra-articular therapies are recommended by NICE.
Some international guidelines, for example, the Osteoarthritis Research Society International (OARSI),10 the American College of Rheumatology (ACR),11 and European Alliance of Associations for Rheumatology (EULAR) - non-pharmacological management,12 have also used systematic literature reviews and expert consensus to derive their recommendations. Generally, they have similar recommendations to NICE but differ on some therapies. Table 1, provides a summary of these different recommendations.
The ACR guideline conditionally recommends the use of cognitive behaviour therapy for hand, hip and knee OA because of its benefits for chronic pain but suggests further research is required to elucidate potential benefits for OA pain. The ACR also recommends that acupuncture may be recommended conditionally because of evidence of efficacy in reducing pain but acknowledges that limitations in study design restrict interpretation of these findings.
The ACR recommends tramadol preferentially over other opioids if required for pain, though the evidence base for this is unclear. OARSI conditionally recommends duloxetine (a serotonin-noradrenaline reuptake inhibitor) for patients with knee OA with concomitant depression. NICE currently does not make a recommendation on the use of antidepressants for OA because of the lack of evidence in treating OA symptoms, though patients with OA and clinical depression will still need appropriate evaluation and treatment.
OARSI conditionally recommends use of intra-articular hyaluronan in knee OA stating that this may be safer and have longer lasting effects than intra-articular corticosteroid injections. NICE guidance still recommends against intra-articular hyaluronan because of the lack of consistent, clinically important benefits across the published literature.
Platelet rich plasma (PRP) injections are not included in the latest NICE guideline but are strongly recommended against by OARSI and the ACR because of lack of quality evidence for their efficacy. Recently Bennell and colleagues conducted a large, well designed, randomised controlled trial comparing PRP injections with placebo in knee OA, and reported no significant difference in pain after one year.13
Tailoring treatment to the patient
The impact on each individual’s physical and mental wellbeing as well as occupation should be taken into account when planning management.
The trajectories of pain may differ depending on the joint affected.
Once a hip joint has become chronically and moderately painful, it is likely that hip replacement becomes an important consideration. Referral for joint replacement should be based on severity of symptoms and failure of conservative treatment, and should not be influenced by factors such as age, gender or comorbidities. Arthroscopic management including lavage should not be used in OA.
Only a relatively small proportion of people with knee OA will require joint replacement and here quadriceps muscle strengthening may be the most appropriate target for most patients together with optimisation of pharmacological therapy.
Individual small joint OA of the fingers may be painful for one to two years while deformity is occurring, and then patients are left with stiff but not painful fingers. However, when loss of grip strength occurs over this painful period of months to years, exercise interventions aimed at grip muscle strengthening is required.
Taking comorbidities into account is clearly important when prescribing drug therapies. For example, NSAIDs should not be prescribed to patients with ischaemic heart disease and can lead to aggravation of hypertension and renal impairment which are common conditions in the typical age group with OA i.e. over 60.14
Monitoring and follow-up
Previous NICE OA guidelines suggested annual follow-up for some patients if they had: multiple joints affected; severe symptoms; comorbidities or been prescribed medications regularly. However, the new NICE guidance emphasises patient-led follow-up for most patients, based on their symptom burden. This reinforces the importance of patient education to enable effective self-management of symptoms.
This should again be tailored to the individual patient. For example, if patients are prescribed NSAIDs, they should be monitored (including blood pressure and renal function) depending on risk.14 In usual practice, patients will already often be reviewed if they have ongoing prescriptions. NICE suggests that optimal follow-up for OA (patient-led versus routine) is an area for future research.
Other areas for future research suggested by NICE include comparing supervised with non-supervised exercise programmes, topical NSAIDs with topical capsaicin, and the use of devices for lower limb OA.
Conclusion
OA management remains challenging with few evidence-based therapies.
The importance of beneficial non-pharmacological therapies, especially muscle strengthening, and increased activity must therefore remain at the forefront of efforts to reduce the impact of this disease on patients.
REFERENCES
1 Long H, Liu Q, Yin H et al. Prevalence trends of site-specific osteoarthritis from 1990 to 2019: findings from the global burden of disease study 2019. Arthritis Rheumatol 2022;74(7):1172-83
2 Swain S, Sarmanova A, Mallen C et al. Trends in incidence and prevalence of osteoarthritis in the United Kingdom: findings from the Clinical Practice Research Datalink (CPRD). Osteoarthritis Cartilage 2020;28(6):792-801
3 Allen KD, Thoma LM, Golightly YM. Epidemiology of osteoarthritis. Osteoarthritis Cartilage 2022;30(2):184-95
4 Glyn-Jones S, Palmer AJR, Agricola R et al. Osteoarthritis. Lancet 2015;386 (9991):376-87
5 National Institute for Health and Care Excellence. NG226. Osteoarthritis in over 16s: diagnosis and management. NICE. London. 2022
6 Katz JN, Arant KR, Loeser RF. Diagnosis and treatment of hip and knee osteoarthritis: a review. JAMA 2021; 325(6):568-78
7 National Institute for Health and Care Excellence. NG100. Rheumatoid arthritis in adults: management. NICE. London. 2020
8 Neogi T. The epidemiology and impact of pain in osteoarthritis. Osteoarthritis Cartilage 2013;21(9):1145-53
9 National Institute for Health and Care Excellence. CG189. Obesity: identification, assessment and management. NICE. London. 2014
10 Bannuru RR, Osani MC, Vaysbrot EE et al. OARSI guidelines for the non-surgical management of knee, hip, and polyarticular osteoarthritis. Osteoarthritis Cartilage 2019;27(11):1578-89
11 Kolasinski SL, Neogi T, Hochberg MC et al. Guideline for the management of osteoarthritis of the hand, hip, and knee. Arthritis Care Res 2020;72(2):149-62
12 Fernandes L, Hagen KB, Bijlsma JWJ et al. EULAR recommendations for the non-pharmacological core management of hip and knee osteoarthritis. Ann Rheum Dis 2013;72(7):1125-35
13 Bennell KL, Paterson KL, Metcalf BR et al. Effect of intra-articular platelet-rich plasma vs placebo injection on pain and medial tibial cartilage volume in patients with knee osteoarthritis: The RESTORE randomized clinical trial. JAMA 2021;326(20):2021-30
14 National Institute for Health and Care Excellence. Clinical knowledge summaries. Scenario: NSAIDs prescribing issues 2020 [Last accessed 27 Oct 2022]
ARTICLE IN PDF
PRESET SEARCHES
British Institute of Musculoskeletal Medicine
Primary Care Rheumatology and Musculoskeletal Medicine Society
PubMed
Osteoarthritis general practice
EXTERNAL WEBLINKS
For patients

 = Registered users
= Registered users = Paid-up subscribers
= Paid-up subscribers