Preset searches
PubMed -Respiratory medicine
Obstructive sleep apnoea hypopnoea
Tuberculosis primary care review
Upper respiratory tract infections
Lower respiratory tract infections
Respiratory medicine
Early diagnosis the main driver to improving outcomes in lung cancer
20 Dec 2022
Earlier diagnosis of lung cancer improves outcomes for two main reasons. First, the disease stage may be earlier allowing more chance of curative-intent treatment. Second, patients may be fitter at presentation. Functional status is one of the most important independent predictors of survival. Lung cancer is caused by smoking in 80-85% of cases. Patients who do not have smoking-attributable lung cancer are often diagnosed late. So it is important to refer patients who have persistent symptoms either for chest X-ray, or when symptoms persist and no alternative diagnosis is found, refer for consideration of CT.
 |
|Diagnosing asthma in school-age children can prove challenging
20 Dec 2022
Asthma is the most common chronic respiratory condition affecting children in the UK. There is no single gold standard test to confirm the diagnosis and both overdiagnosis and underdiagnosis are common. Asthma should be suspected in any child presenting with episodes of wheeze, especially recurrent episodes of wheeze. Clinical diagnosis alone often results in misdiagnosis; all children from the age of five years under investigation for asthma in primary care should have access to spirometry, bronchodilator reversibility and FeNO testing.
Tailor treatment to the patient with COPD
20 Dec 2021
COPD is characterised by persistent respiratory symptoms and airflow limitation that is due to airway and/or alveolar abnormalities usually caused by significant exposure to noxious particles or gases and influenced by host factors including abnormal lung development. Performance and interpretation of spirometry should be based on clinical suspicion of airway disease in a patient with suggestive symptoms and exposures, where a medical history has been taken and examination performed.
 |
|Managing acute asthma in adults in primary care
20 Dec 2021
Treatment with bronchodilators and oral corticosteroids should be given as soon as possible in an acute asthma exacerbation. In moderate exacerbations, hospital admission is based on multiple factors, including response to initial treatment, known reduction in baseline lung function, history of exacerbations, particularly previous need for critical care involvement, and ability to cope at home. Patients with features of acute severe or life-threatening asthma should be referred to hospital immediately following initial assessment.
 |
|Improving the management of chronic asthma in children
21 Dec 2020
There is no gold standard test to diagnose asthma. As a result, overdiagnosis and underdiagnosis are common especially when relying on history and clinical examination alone. Spirometry and bronchodilator reversibility testing are particularly useful when a child aged 5 years or older is brought to the practice with symptoms. The validated Asthma Control Test for children aged 12 years and over and the Children’s Asthma Control Test for children aged 4-11 years should be used to assess current asthma control based on four-week recall. Asthma control test scores correlate poorly with lung function and measures of airway inflammation such as FeNO in children and should not be used in isolation.
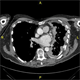 |
|Diagnosis and management of malignant pleural mesothelioma
21 Dec 2020
Mesothelioma accounts for less than 1% of all cancers in England, Wales and Northern Ireland. There are almost 2,500 new diagnoses a year, of which 96% are pleural. The median age at diagnosis for malignant pleural mesothelioma (MPM) is 76 years. The majority of cases occur in men, most commonly following occupational exposure to asbestos. There is a latent period, usually 30-40 years, between exposure and disease development. A chest X-ray is usually the first-line investigation; 94% of patients with MPM have a unilateral pleural effusion, although the chest X-ray may be normal or show another asbestos-related lung disease.
 |
|Detecting obstructive sleep apnoea hypopnoea syndrome
24 Oct 2019
Obstructive sleep apnoea hypopnoea syndrome (OSAHS) is characterised by repeated episodes of partial or complete collapse of the upper respiratory passages, mainly the oropharyngeal tract, during sleep. Obesity is the strongest risk factor for OSAHS; other risk factors include smoking, excessive drinking, sedatives and hypnotics. Habitual snoring, unrefreshing sleep and daytime somnolence suggests the possibility of OSAHS. When this is combined with a partner’s account of nocturnal apnoeas or snoring pauses the diagnosis becomes highly likely. However, negative screening results or the absence of clinical features by themselves should not be used to rule out OSAHS.
 |
|Improving COPD outcomes in primary care
24 Oct 2019
Diagnosis of COPD is based on the presence of airflow obstruction after the administration of a bronchodilator i.e. post-bronchodilator spirometry. However, the National COPD Audit report for 2017-18 found that 59.5% of people hospitalised with a COPD exacerbation in England and Wales had no spirometry result available and in 12% of those who had undergone spirometry the test showed no airflow obstruction. Patients with COPD should be reviewed annually. It is advisable to repeat spirometry if there is a significant change in symptoms. It is important to determine objective measures of breathlessness (MRC dyspnoea score), quality of life (CAT questionnaire) and exacerbations (annual exacerbation and hospitalisation rate) as part of this review.
 |
|Managing mild to moderate asthma in adults
22 Nov 2018
The National Review of Asthma Deaths found that most patients who died were actually considered to have mild to moderate asthma, with 57% of fatal cases not under specialist care at the time of their death. In cases of fatal asthma there was widespread underuse of inhaled corticosteroids and an overreliance on short-acting beta-agonists. Referral to secondary care should take place when there is diagnostic uncertainty or atypical features, the possibility of hypersensitivity to inhaled material or concerns over treatment or exacerbations. Patients who have suffered even a single life-threatening asthma attack should be under specialist supervision.
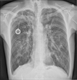 |
|Managing complications of cystic fibrosis in adults
22 Nov 2018
Overall survival has improved dramatically for patients with cystic fibrosis (CF) since the millennium such that median life expectancy now extends into the fifth decade. However, with increasing longevity comes a range of comorbidities, some as complications of the disease itself but others as a consequence of long-term treatments required to manage CF. Chronic infection and inflammation eventually cause irreversible bronchiectasis and decline in pulmonary function, and 90% of CF deaths are caused by progressive respiratory failure.
 |
|Diagnosing and managing cystic fibrosis in children
22 Nov 2018
Cystic fibrosis (CF) is a multisystem genetic disorder affecting around 1 in 2,500 live births in the UK. Although all newborns undergo screening for CF, around 15% of infants will present shortly after birth with meconium ileus and some will already have faltering growth when the screening results are available at 3-4 weeks of age. Infants who present with meconium ileus should be treated with a high index of suspicion for CF until proven otherwise. Mucociliary dysfunction leads to accumulation of mucus in the airways and secondary infection. Respiratory symptoms may be non-specific initially and include cough and wheeziness, frequent respiratory infections and, in older children, sinusitis.
 |
|Improving outcomes in COPD
23 Nov 2017
Cigarette smoking is overwhelmingly the most important risk factor for COPD. In some cases, other factors such as occupation, passive exposure to inhalants and fetal nutrition/low birthweight are also important. The diagnosis should be suspected in symptomatic patients with risk factors, usually cigarette smoking, aged 40 years or above, albeit a majority of people with COPD present when considerably older. The 2017 GOLD guideline recommends that management should be focused on two objectives. First, to relieve symptoms of breathlessness (assessed using the MRC dyspnoea scale) and improve quality of life (assessed by the COPD Assessment Test). Second, to reduce risk assessed by the number of exacerbations and hospitalisations in the previous year.
 |
|Regular review pivotal in chronic asthma in children
23 Nov 2017
The aim of asthma treatment is complete control of symptoms as soon as possible while minimising side effects and inconvenience to the patient. All parents and older children should be offered a written action plan. This should include details of the patient’s regular medicines, how to recognise deterioration and what to do in the event of an attack. Children should be referred to secondary care if: the diagnosis is unclear; control remains poor despite monitored treatment; they have suffered a life-threatening attack or red flag features are present.
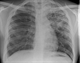 |
|Assessment and management of active and latent TB
24 Nov 2016
Clinically significant disease occurs through progression of primary infection or through later reactivation of latent TB infection (LTBI); this is most likely to occur in the first few years following infection, although late reactivation can occur several decades later, particularly in individuals who become immunosuppressed. Risk of TB acquisition is increased in people who have come to the UK from high incidence countries or who are born in the UK but come from high-risk ethnic minority groups. Other risk groups include those who are homeless, in prison or who misuse drugs or alcohol.
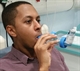 |
|GPs have key role in improving outcomes in acute asthma
24 Nov 2016
Features which indicate a high risk of severe attacks include: previous admission to intensive care, particularly if requiring mechanical ventilation; previous admission with asthma especially in the past year or repeated emergency admissions; history of worsening asthma in January or February; use of three or more classes of asthma medication; heavy use of beta-2 agonists; anxiety traits; and marital stress.
 |
|Optimising the management of patients with difficult asthma
25 Nov 2015
Between 5 and 10% of asthma (depending on the definition used) is categorised as difficult asthma, a term which generally refers to patients who continue to experience symptoms and frequent exacerbations despite the prescription of high-dose asthma therapy. Difficult asthma is an indication for specialist review by an appropriate respiratory physician, but close liaison between primary, secondary and tertiary care is critical.
 |
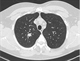
|Improving the diagnosis and management of COPD
25 Nov 2015
COPD is a progressive condition. Therefore, earlier diagnosis allows earlier intervention in particular smoking cessation. Spirometry should be performed in symptomatic current or former smokers (typically ≥ 10 pack years) who are aged at least 35 where COPD is a likely differential diagnosis.
This article online comes with updates and links to recent research and guidance, most notably the GOLD 2017 guide to COPD.
 |
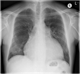
|Early diagnosis pivotal to survival in lung cancer
24 Nov 2014
Lung cancer is the most common cause of cancer death, both in the UK and worldwide. There has been little change in survival over the past 20 years, with increasing evidence that there are disparities in outcomes between the UK and other comparable healthcare systems. It has been postulated that this is due to an excess of early deaths, delays in diagnosis are thought to contribute to this problem. A recent study showed that 30% of patients with lung cancer die within the first 90 days and they have seen their GP on average five times in the four months before diagnosis, suggesting there may be opportunities to diagnose these patients earlier in the disease process. The challenge GPs face is to identify and refer those at risk as early as possible and to maintain a high index of suspicion if symptoms persist. [With external links to current evidence base]
 |
|Improving the management of asthma in adults in primary care
24 Nov 2014
Studies in adult patients have suggested that 30% of those diagnosed with asthma do not have the condition and it is likely that the diagnosis is missed in many others. The BTS/SIGN guideline advocates spirometry after taking the history. If airflow obstruction is present, a trial of treatment can commence, but a firm diagnosis also requires a symptomatic response and an improvement in the measured airflow obstruction. The FeNO level correlates well with airway inflammation, and is therefore a good indicator of asthma and in particular of the likely response to inhaled corticosteroids. The test is especially useful for patients with suggestive symptoms but normal spirometry.
 |
|Diagnosing and managing pulmonary hypertension
12 Dec 2012
Pulmonary hypertension (PH) is defined as an increase in mean pulmonary arterial pressure ≥ 25 mmHg at rest as assessed invasively by right heart catheterisation. It can affect patients at any age and presents with non-specific symptoms. Accurate diagnosis is important as while PH is a potentially lethal disease it is treatable. Identification of the cause of PH is crucial to ensure that the patient receives appropriate management.
 |
|Occupational asthma often goes unrecognised
12 Dec 2012
Occupational asthma is induced de novo by an airborne agent encountered in the workplace. The risk of occupational asthma is greater in those with a prior atopic history. Work-exacerbated asthma is the provocation of pre-existing, or coincidental, disease by one or more irritant exposures at work. Distinguishing occupational from work-exacerbated asthma can be difficult but it is important since the two have very different clinical, occupational and legal implications.
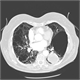 |
|Improving outcomes in lung cancer patients
23 Nov 2011
Lung cancer is the leading cause of cancer mortality in the UK resulting in more than 33,500 deaths in 2008, 4,000 more than for bowel and breast cancer combined. Five-year survival figures are poor but have recently improved from around 5% to 7.5% in men and 8.5% in women.There is evidence of marked variation in the standard of care in England. It has recently been shown that if patients are first referred to a thoracic surgical centre, rather than a hospital that does not have thoracic surgeons on site, they are 51% more likely to have a resection. There are similar findings for other active treatments. By reducing this variation there is scope for marked improvement in outcomes, possibly to levels seen in other countries such as Australia, Canada, Sweden and Norway where five-year survival rates are approximately double. Thus there is a need to encourage lung cancer teams to select patients correctly so that the best treatment can be offered. Improving diagnosis, staging and fitness assessment was a major focus in the recently updated NICE guideline on diagnosis and treatment of lung cancer, published in April 2011. [With external links to current evidence and summaries]
 |
|New tests will improve detection of latent TB
22 Nov 2011
In the UK, after a century of declining incidence, over the past 20 years numbers of cases of active TB have increased substantially. This increase has occurred almost exclusively in individuals born outside the UK. GPs represent the first point of contact with health services for most patients, and it is crucial that GPs are aware of the clinical features of active TB, and that diagnosis can frequently be made using simple and inexpensive tests such as chest X-rays and sputum samples. There is a major focusin the UK on raising awareness of TB in frontline medical staff, through the activities of bodies such as the charity TB Alert, and the Department of Health’s National Knowledge Service TB Project At a local level, information and advice can readily be obtained through the local TB nursing service.
Opportunistic case finding pivotal in diagnosing COPD
23 Nov 2010
Diagnosis, management and delivery of care for patients with chronic obstructive pulmonary disease (COPD) remains an important issue for clinicians. COPD accounts for more than 10% of emergency hospital admissions. The 2008 National COPD Audit showed that the 90-day mortality rate after a COPD hospitalisation was 13.9% and almost one in three patients discharged from hospital were readmitted within three months. Over the past decade a huge number of publications have strengthened the evidence base which is the foundation for COPD management while the development of a National Clinical Strategy for COPD and the 2010 update to the NICE COPD guidelines should help implementation of an evidence-based approach to management. At the time of writing (November 2010) the consultation phase of the National Clinical Strategy had been completed but no publication date had been set.
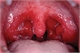 |
|Tackling upper respiratory tract infections
22 Nov 2010
Upper respiratory tract infection (URTI) refers to a wide range of acute illnesses that affect the upper respiratory tract. URTIs are the most common reason for general practice consultations. On average adults suffer two to three such infections per year. Most URTIs are self-managed. A UK study of 516 women aged 20-44 years found that only one in 18 episodes of sore throat led to a general practice consultation. Patients who do seek consultations often benefit from reassurance, education and instructions for symptomatic home treatment. A large proportion of antibiotic prescribing in primary care is for respiratory tract infections. There was a 44% reduction in antibiotic prescribing for respiratory tract infections between 1994 and 2000. The larger part of this reduction was due to lower consultation rates rather than a decrease in prescribing by GPs. Antibiotics are frequently prescribed for resolving symptoms and to prevent complications. Patients' expectations have a significant influence on prescribing, even when their doctor judges that antibiotics are not indicated.There are certain at-risk groups who require immediate antibiotics or further evaluation.
 |
|Obstructive sleep apnoea increases risk of CVD
15 Nov 2009
In OSA, the patient suffers repeated episodes of apnoea caused by narrowing or closure of the pharyngeal airway during sleep. About 2-4% of the middle-aged population have OSA. Although understanding of the condition has improved considerably, it is estimated that 85-90% of sufferers still remain undiagnosed.
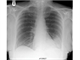 |
|Managing LRTI in adults in the community
15 Nov 2009
Lower respiratory tract infection (LRTI) is a common cause of consultation in primary care. In 2004, approximately 5% of the population consulted their GP about LRTI at least once during the year, a rate comparable with those reported by previous UK studies.
Reducing exacerbations in patients with COPD
19 Nov 2008
More than 27,000 people die from chronic obstructive pulmonary disease (COPD) each year in the UK. It is estimated that there are around 1.5 million adults with COPD, thus a GP practice with approximately 7,000 patients will have up to 200 patients with COPD on its practice list.

