CPD frameworks
These frameworks, associated with all articles, prompt drafting of personal learning, reflection and planning.
Save your reflective note into your device or cloud
Fillable PDF frameworks
Adobe reader needed for tablets
Word frameworks - for reflective practice
Click to download
Reflection on a journal article
Stages of reflection on a situation
Reflection of a team, practice or group
External reference on reflection
Reflective practice in health care and how to reflect effectively
Koshy K, Limb C et al. International Journal of Surgical Oncology. 2017 2:e20
RENAL MEDICINE
GPs should be vigilant for accelerated progression of CKD
24 Jan 2022
Despite being common, CKD often remains undiagnosed partly because of lack of symptoms until late in the disease process. Late detection of CKD, and hence lack of effective management, increases the risk of progression to end-stage renal disease which often requires renal replacement therapy such as dialysis or transplantation. Derangement in serum creatinine and eGFR will alert a clinician to a patient with potential CKD. Timely referral for specialist nephrology input when required is key.
Suspected nephrotic syndrome warrants urgent referral
24 Jan 2022
Nephrotic syndrome results from dysfunctional glomerular filtration and consists of three clinical features: severe proteinuria (> 3.5 g/24 hr); hypoalbuminaemia (serum albumin < 30 g/L); and peripheral oedema. It may occur in people of all ages. If nephrotic syndrome remains uncontrolled even those with normal kidney function at presentation can develop progressive chronic kidney disease. All patients with suspected nephrotic syndrome should be referred urgently to nephrology.
 |
|Reducing cardiovascular risk pivotal in diabetic kidney disease
21 Feb 2021
Diabetic kidney disease is associated with a very high risk of cardiovascular disease (CVD) and premature mortality from cardiovascular events. There is good evidence that multifactorial interventions that optimise BP, limit proteinuria and minimise cardiovascular risk can reduce morbidity and premature mortality. Early diabetic kidney disease is asymptomatic. Microalbuminuria, defined as a urinary ACR of 3-30 mg/mmol on two occasions three months apart is the earliest clinically detectable indicator of diabetic kidney disease. Excellent glycaemic control can delay onset of microalbuminuria.
Tight blood pressure control key in polycystic kidney disease
21 Feb 2021
Polycystic kidney disease (PKD) has an autosomal dominant mode of inheritance. Despite this 25% of patients will have no known family history and these cases are thought to be due to de novo mutations in the causative genes. PKD can present asymptomatically and should be considered in any patient with renal cysts noted on abdominal imaging, especially if there is a history of hypertension. Patients with PKD may present with hypertension before a decline in eGFR is noted. Cyst haemorrhage, rupture or infection can all present with acute loin pain. PKD can also cause a number of extrarenal complications.
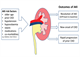
Prompt recognition key in glomerulonephritis
24 Feb 2020
Glomerulonephritis is the second most common cause of end stage renal disease in the UK and the most common cause in those under 35. Some forms can respond well to treatment if diagnosed early. However, if glomerulonephritis goes unrecognised, it can lead to irreversible loss of renal function. Glomerulonephritis can present in a wide variety of ways, ranging from asymptomatic urinary abnormalities to fulminant disease with life-threatening acute kidney injury and extra-renal manifestations. Asymptomatic invisible haematuria is common. In the absence of infection or a urological cause, glomerulonephritis should be considered. Significant proteinuria (> 1 g/day) in the absence of an identifiable cause warrants referral.
 |
|GPs play an important role in identifying acute kidney injury
24 Feb 2020
Acute kidney injury (AKI) is a common complication in hospitalised patients and is associated with an increased risk of chronic kidney disease (CKD) and higher mortality. Two thirds of AKI cases develop in the community prior to hospital admission. AKI may be challenging to recognise because it is typically asymptomatic. It is usually detected incidentally in the setting of another illness when a rise in serum creatinine from baseline is identified. Risk factors for AKI include age 65 or over, diabetes, CKD, neurological or cognitive impairment, heart failure and the use of potentially nephrotoxic medications. Recognition of those at risk should prompt earlier and more frequent testing of U&E during any acute illness.
Tailoring dialysis modality to the patient
22 Feb 2019
End stage renal disease can be defined as the requirement for kidney transplantation or dialysis therapy. In the UK in 2016, of the 63,162 people receiving renal replacement therapy 53% were renal transplant recipients, 41% were on haemodialysis and 6% were on peritoneal dialysis. Dialysis should be started when: symptoms of uraemia impact on day to day living; the need is indicated by biochemical measures or uncontrollable fluid overload or at an eGFR of 5-7 ml/min/1.73 m2 in the absence of symptoms. The choice of dialysis modality is influenced by the individual’s functional status, social circumstances and confidence.
 |
|Management and prevention of renal and ureteric stones
22 Feb 2019
Kidney stones are common with as many as 1 in 10 people developing a symptomatic stone. Up to 50% of stone formers will have at least one further symptomatic stone in their lifetime. Ureteric colic is unaffected by posture with patients often writhing in seemingly futile attempts to relieve pain. Immediate management comprises effective analgesia while urinalysis is the first step in confirming the diagnosis. One of the challenges facing the GP is to differentiate patients who warrant immediate hospital referral from those who can be seen less acutely.
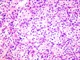 |
|Prompt investigation improves outcomes for kidney cancer
22 Feb 2018
Renal cell carcinoma should be suspected in the presence of: localising symptoms such as flank pain, a loin mass or haematuria; constitutional upset including weight loss, pyrexia and/or night sweats; or unexplained test results. Smoking, obesity and hypertension are common risk factors and all three demonstrate a dose-response relationship with the relative risk of renal cell carcinoma.
 |
|Visible and non-visible haematuria may herald serious disease
22 Feb 2018
Both visible (VH) and non-visible haematuria (NVH) may herald serious pathology e.g. malignancy or vasculitis. All patients with VH or symptomatic NVH should have urinalysis, urinary protein estimation (albumin:creatinine or protein:creatinine ratio), and a renal function test. These should also be requested if asymptomatic NVH persists, i.e. in two out of three samples over 6-8 weeks.
 |
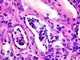
|Diagnosis and management of nephrotic syndrome
22 Feb 2017
Nephrotic syndrome is uncommon in general practice. A GP may only see two or three adult cases in their career. Nephrotic syndrome develops following pathological injury to renal glomeruli. This may be a primary problem, with a disease specific to the kidneys, or secondary to a systemic disorder such as diabetes mellitus. The most common cause in children is minimal change glomerulonephritis. In white adults, nephrotic syndrome is most frequently due to membranous nephropathy whereas in populations of African ancestry the most common cause of nephrotic syndrome is focal segmental glomerulosclerosis (FSGS). Diabetic nephropathy is the most common multisystem disease that can cause nephrotic syndrome.
 |
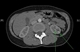
|Pyelonephritis can lead to life-threatening complications
22 Feb 2017
As distinct from cystitis and lower urinary tract infection (UTI), which are much more common, pyelonephritis involves the upper tract with potentially more serious sequelae. It is most commonly caused by bacterial infections, typically ascending from the lower urinary tract; haematological seeding from bacteraemia is less common.
 |
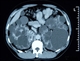
|Managing acute and chronic renal stone disease
22 Feb 2016
The incidence of renal stone disease is increasing globally. In the UK the lifetime risk is estimated to be 8-10%. On a population level, the increase in stone incidence, erosion of gender disparity, and younger age of onset is likely to reflect increasing prevalence of obesity and a Western diet with a high intake of animal protein and salt.
 |
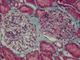
|Optimising the management of polycystic kidney disease
22 Feb 2016
Polycystic kidney disease is the most common inherited renal disorder that results in chronic kidney disease. Clinical features include visible haematuria, loin pain, UTI and hypertension. The typical clinical course is a progressive increase in the number and size of renal cysts associated with gradual loss of kidney function (falling eGFR).
 |
|Improving early detection of chronic kidney disease
23 Feb 2015
Chronic kidney disease (CKD) is defined as either a reduction in measured kidney function (eGFR) or urinary abnormalities (haematuria/proteinuria) or a combination of both, present for more than 3 months. Individuals with newly identified reduced eGFR should have acute kidney injury excluded. All newly identified CKD patients should have blood pressure, dipstick urinalysis, random urine ACR or PCR, glucose, cholesterol and full blood count checked at the earliest opportunity.
 |
|Timely diagnosis and treatment essential in glomerulonephritis
23 Feb 2015
Glomerulonephritis is an important cause of kidney disease and, in the UK, the most common diagnosis in patients receiving chronic dialysis or waiting for kidney transplantation. A key feature is the presence of urinary abnormalities (proteinuria ± haematuria). Timely diagnosis and treatment of glomerulonephritis can help to minimise both the occurrence and severity of complications.
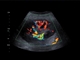
Risk factor control is key in diabetic nephropathy
24 Feb 2014
Prolonged duration of diabetes, poor glycaemic control and hypertension are major risk factors for both diabetic nephropathy and cardiovascular disease. Optimising blood sugar control together with excellent control of blood pressure can reduce the risk of developing diabetic nephropathy. Diabetic nephropathy should be considered in any patient with diabetes when persistent albuminuria develops.
 |
|Renal replacement therapy should be tailored to the patient
24 Feb 2014
End-stage renal disease describes loss of kidney function which is both substantial and irreversible. The form of renal replacement therapy (RRT) instituted should primarily be based on patient preference subsequent to an individually tailored education programme from specialist staff. This programme needs to take into account the patient’s comorbidities and any contraindications to specific modalities of RRT. For those who will be suitable for transplantation, optimum management of diabetes, smoking cessation, weight loss, and general fitness is crucial in facilitating this.
 |
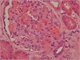
|Tracking down the cause of proteinuria in primary care
21 Feb 2013
Proteinuria originates from the kidney and occurs as a result of injury to either the glomerulus or the renal tubule or both. It is relatively common in the general population with reported point prevalence of up to 8% but the prevalence falls to around 2% on repeated testing. Chronic glomerular injury resulting in proteinuria may be secondary to prolonged duration of diabetes or hypertension. A tubular origin of proteinuria may be associated with inflammation of renal tubules triggered by prescribed drugs or ingested toxins.
 |
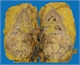
|Early recognition of CKD can delay progression
21 Feb 2013
CKD affects 8.5% of the UK population. Early recognition allows intervention that may delay or avoid progression to end-stage disease and modify the cardiovascular risk associated with CKD. The most frequent specific renal diseases resulting in progressive CKD in the UK are: diabetes mellitus, atheromatous renal vascular disease, glomerulonephritis, chronic pyelonephritis and inherited renal disease.
 |
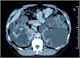
|Early diagnosis improves survival in kidney cancer
24 Feb 2012
Kidney cancers account for 2-3% of all adult malignancies in the UK. The incidence has been increasing which may reflect changing risk factors including a rise in obesity. Early diagnosis improves survival with five-year survival rates for renal cancer of 70-94% for localised tumours, in the UK, but this survival rate falls to 40-70% when cancer has spread beyond the kidney. [With external links to current evidence and summaries]
 |
|Improving recognition of inherited renal disease
23 Feb 2012
The GP is usually the first medical professional to be consulted on a hereditary disease of the kidney. Support for both the patient and their GP should be provided by renal and genetic specialists. Ongoing support in primary care is imperative. The primary care team can provide advice and reassurance to parents with regard to screening children.
 |
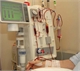
|Which patients with renal colic should be referred?
23 Feb 2011
Renal stone disease is a common, and potentially recurrent, condition that affects 5-15% of the population worldwide.Symptomatic renal stone disease is at least twice as common in men as women.The incidence has risen over two decades and 1-2 people per thousand present with an acute episode of pain caused by renal stones each year. Annually there are more than 12,000 renal stone-related hospital admissions and considerably more GP consultations for management of renal colic. Data from NHS Direct showed that 80% of patients with renal colic symptoms were advised to contact their GP as the first port of call. The challenge for GPs is to identify which cases may be treated safely at home and which need immediate referral to hospital.
 |
|Managing patients on dialysis in the community
22 Feb 2011
There are approximately 50,000 people in the UK on renal replacement therapy (RRT) and this number is increasing each year. In an average GP practice there will be one or two patients currently on RRT and a larger number with progressive chronic kidney disease who will reach end stage renal disease (ESRD). The options for RRT are kidney transplantation, haemodialysis (HD) or peritoneal dialysis (PD). The management of an individual with ESRD may involve all of these modalities during the course of their lifetime. For many patients with ESRD, treatment at home allows greater flexibility and independence than can be facilitated by inpatient HD. Others value the security of receiving their RRT in a hospital environment and would resent the intrusion of dialysis into their home life. All patients appreciate early information about the options for RRT so that they and their family can make an informed decision about the best treatment for them. The aim is to provide personalised information to patients at least three months before they need to begin RRT.
 |
|Acute pyelonephritis can have serious complications
15 Apr 2010
The incidence of acute pyelonephritis is higher in young women than in men but the incidence in men over 65 years of age is similar to that in older women. Women have up to a 10% risk of recurrent acute pyelonephritis in the year following a first acute episode, the equivalent risk in men is lower at 6%. Acute pyelonephritis may be uncomplicated and resolve without serious sequelae. However, a minority of episodes may be complicated by acute kidney injury, papillary necrosis, renal or perinephric abscess or the development of emphysematous pyelonephritis.
 |
|GPs should be vigilant for glomerulonephritis
14 Apr 2010
Across all age groups, glomerulonephritis is the second most common renal disease leading to end-stage renal disease in the UK, but is relatively more common in those requiring renal replacement therapy under the age of 65. The incidence of glomerulonephritis is reported as 73 cases per million population per year. This equates to one new presentation per GP practice in the UK approximately every other year. With an average 10-year survival of 63%, most practices are likely to have a small number of patients with chronic glomerulonephritis at any one time.
 |
|Evaluating haematuria in primary care
25 Apr 2009
Haematuria is a fairly common problem in general practice with a higher incidence in patients over 40 years old. In adults the reported prevalence of microscopic haematuria varies considerably, ranging from 1 to 20% and is highest in men over 60 years old.3 In younger adults haematuria, particularly if it is transient, may have no obvious underlying cause. In contrast, persistent haematuria may herald the first presentation of serious urological or renal disease and there is an increased risk of malignancy in older patients. Nevertheless, in many patients no diagnosis for haematuria is established despite extensive investigation.
 |
|Renal medicine: Early detection of CKD will reduce heart disease risk
25 Apr 2009
In April 2008, the Department of Health announced a strategy to reduce the adverse effects of vascular disease by focusing on its earlier detection.1 By introducing 'vascular checks' targeting those aged between 40 and 75 years of age, it is estimated that at least 25,000 people a year with diabetes or kidney disease will be diagnosed earlier. With increasing evidence that early treatment of kidney disease can slow, if not prevent, progression to established renal failure, early detection is of clear benefit from a purely renal perspective.
 |
|February 2008: Blood pressure control key in polycystic kidney disease
01 Feb 2008
How can polycystic kidney disease present clinically? What are the criteria for diagnosing PKD? How should GPs manage patients with PKD?
 |
|February 2008: Identifying and managing nephrotic syndrome in adults
01 Feb 2008
What are the main features of nephrotic syndrome? How can proteinuria be treated? How can complications be avoided?
 |
|February 2007: Early recognition the key to CKD
01 Feb 2007
What is the relationship of CVD to CKD? How should you manage dipstick positive proteinuria or haematuria? Which patients need referral and when?
February 2007: Renal stone recurrence can be prevented
01 Feb 2007
What are the common causes of renal stones? How should renal stones be investigated? How can recurrence be prevented?

