CPD frameworks
These frameworks, associated with all articles, prompt drafting of personal learning, reflection and planning.
Save your reflective note into your device or cloud
Fillable PDF frameworks
Adobe reader needed for tablets
Word frameworks - for reflective practice
Click to download
Reflection on a journal article
Stages of reflection on a situation
Reflection of a team, practice or group
External reference on reflection
Reflective practice in health care and how to reflect effectively
Koshy K, Limb C et al. International Journal of Surgical Oncology. 2017 2:e20
United Kingdom
British Cardiovascular Society
Royal College of GPs
Brit. Association of Cardiac Rehabiliation
HeartUK
Brit. Hypertension Society
NHS
NHS Improvement:Heart
NHS Improvement:Stroke
NHS Health Check
Patient information
British Heart Foundation
Sudden Arrhythmia Death Syndromes Foundation
sadsuk.org
Cardiac Risk in the Young
HeartHub.org (AHA)
Cardiomyopathy Association
Arrhythmia Alliance (UK)
Atrial Fibrillation Association
NHS Choices (UK):CHD
Multilingual(Eng., French, Spanish, German, Russian)
Heartfailurematters.org
Syncope Trust and Reflex Anoxic Seizures
STARS(UK)
STARS (US)
Europe
European Society of Cardiology
European Primary Care Cardiovascular Society
European Association of Cardiac Prevention and Rehabilitation
Heart Failure Association
European Forum for Primary Care (EFPC)
European GP Research Network
European Academy of Teachers in GP
European Association for Quality in GP
Wonca Europe
European Society of Hypertension
Eur.Atherosclerosis Society
Riskfactor assessment
Heartscore
World
World Heart Federation
Wonca World - GlobalFamilyDoctors
WHO:cardiovascular
Int. Stroke Society
Int. Soc. of Hypertension
Statistics
Heartstats
Ireland
Cardiovascular medicine - Special interest
Special reports
 |
|Diagnosis and management of hypertension in primary care
24 Feb 2020
NICE stipulates that two of the following are required for the diagnosis of hypertension: clinic blood pressure (BP) 140/90 mmHg or higher and ambulatory BP monitoring daytime average or home BP monitoring average 135/85 mmHg or higher. Evaluation of newly diagnosed hypertension includes an assessment of underlying cardiovascular disease (CVD) risk and target organ damage. Treatment threshold varies with underlying risk. For those at lower risk (< 10% risk of a CVD event over 10 years), drug treatment is not recommended below 160/100 mmHg.
 |
|Detecting and managing pulmonary hypertension
20 Dec 2019
Pulmonary hypertension (PH) is a haemodynamic state where the mean pulmonary artery pressure measured at cardiac catheterisation is 25 mmHg or more. Precapillary PH arises from increased resistance to blood flow in the pulmonary arterioles and postcapillary PH from elevated left atrial pressure. In postcapillary PH the cause is left heart disease whereas precapillary PH may be caused by any other form of PH. Patients develop symptoms only when the disease is advanced. Symptoms at presentation are non specific. Adults almost always present with breathlessness and may also complain of exercise-induced dizziness or syncope and angina. An echocardiogram is the best investigation to ascertain the probability of PH.
Cardiovascular Symposium
Prompt diagnosis and treatment will improve heart failure outcomes
27 Oct 2021
The majority of new diagnoses of heart failure (HF) are made only after the patient has deteriorated to the point of requiring hospital admission. Within a month of admission with HF, 1 in 4 patients who survive to discharge will be readmitted, and 1 in 8 will die. Ischaemic heart disease is the most common cause of HF, accounting for at least half of diagnoses: following a heart attack, 1 in 3 patients will develop HF within 5 years. Hypertension, diabetes and obesity are also associated with an increased risk of HF.
Detecting and managing atrial fibrillation in primary care
27 Oct 2021
Atrial fibrillation (AF) is often diagnosed as an incidental finding during a routine medical check. The prevalence increases with age and the presence of CVD further increases the risk of AF. Around 15-30% of patients with AF are asymptomatic. When patients present to their GP the most common symptoms of AF include: palpitations, chest pain, breathlessness and a reduction in exercise/functional capacity. To establish a diagnosis of AF, rhythm documentation with an ECG showing at least 30 seconds of AF is required.
 |
|Suspected cardiac syncope requires urgent investigation
27 Oct 2020
Around 40% of people experience a syncopal event during their lifetime. Cardiac syncope accounts for 10% of presentations. Incidence rises significantly with age. Assessment should be systematic: a thorough history, physical examination including lying and standing BP and 12-lead ECG. The medical history and physical examination are key. If following initial assessment cardiac syncope is suspected patients should be referred for urgent specialist cardiovascular assessment or emergency admission.
 |
|Diagnosis and management of abdominal aortic aneurysm
27 Oct 2020
Risk factors for abdominal aortic aneurysm formation include: smoking, increasing age, and family history. Men over the age of 65 are most commonly affected, with an abdominal aortic aneurysm present in approximately 1%. As the condition is normally asymptomatic, most patients have their aneurysms discovered through the screening programme or incidentally via other imaging investigations. Patients with a new diagnosis of an abdominal aortic aneurysm should be referred to their local vascular service.
 |
|More patients could benefit from referral for cardiac rehabilitation
25 Nov 2019
Cardiac rehabilitation is a combination of medical and behavioural interventions designed to facilitate recovery and prevent future cardiovascular disease events. A cardiovascular prevention and rehabilitation programme (CPRP) is a critical element within the management pathway for most patients with heart disease and has a particularly strong evidence base for those with either symptomatic atherothrombotic vascular disease or heart failure. Following acute MI and/or coronary revascularisation, attending and completing a CPRP is associated with an absolute risk reduction in cardiovascular mortality from 10.4% to 7.6%.
 |
|Reducing stroke risk in patients with atrial fibrillation
25 Nov 2019
Stroke is the most debilitating complication of atrial fibrillation (AF). AF-related strokes account for 20-25% of all strokes and are generally more severe and disabling and more likely to recur. Oral anticoagulation (OAC) remains the cornerstone of AF management with a clear prognostic benefit. It reduces stroke risk by two-thirds and mortality by a quarter. The decision to anticoagulate is taken irrespective of the pattern and duration of AF (paroxysmal, persistent or permanent). A large evidence base supports the use of OAC in men with a CHA2DS2-VASc score of 2 or more and women with a score of 3 or more. Hence, in the absence of absolute contraindications, OAC is strongly recommended.
 |
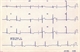
|Tracking down and treating the cause of syncope
22 Oct 2018
Syncope is a transient loss of consciousness (T-LOC) caused by cerebral hypoperfusion, characterised by a rapid onset, short duration and spontaneous complete recovery. It needs to be differentiated from other conditions that can cause T-LOC such as seizures, trauma, hypoglycaemia, and psychogenic causes. Three principal types of syncope can be identified: reflex or neurally mediated, orthostatic hypotensive and cardiac. The common denominator of all these conditions is low systemic BP causing global cerebral hypoperfusion.
Atrial fibrillation
 |
|Reducing stroke risk in patients with atrial fibrillation
25 Nov 2019
Stroke is the most debilitating complication of atrial fibrillation (AF). AF-related strokes account for 20-25% of all strokes and are generally more severe and disabling and more likely to recur. Oral anticoagulation (OAC) remains the cornerstone of AF management with a clear prognostic benefit. It reduces stroke risk by two-thirds and mortality by a quarter. The decision to anticoagulate is taken irrespective of the pattern and duration of AF (paroxysmal, persistent or permanent). A large evidence base supports the use of OAC in men with a CHA2DS2-VASc score of 2 or more and women with a score of 3 or more. Hence, in the absence of absolute contraindications, OAC is strongly recommended.
 |
|Managing arrhythmias in coronary artery disease
23 Jan 2019
A detailed history is essential in patients with coronary artery disease (CAD) to elucidate red flag symptoms necessitating urgent specialist assessment. Red flags include syncope and presyncope, particularly in patients with concomitant left ventricular systolic dysfunction. Palpitations with severe chest pain and breathlessness also warrant urgent assessment. Undiagnosed atrial fibrillation (AF) is common in older populations. LVEF of 35% or less is a predictor of increased risk of sudden death. All patients with CAD should therefore undergo assessment of LVEF, usually by transthoracic echocardiography.
Children and adolescents
 |
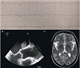
|Diagnosing heart disease in children and adolescents
22 Jun 2017
Heart disease in children and adolescents can be congenital, in which structural defects of the heart and major blood vessels are present from birth, acquired, whereby disease develops during life, or genetic, including diseases affecting the heart muscle, electrical system or the aorta. The incidence of congenital heart disease has decreased over the past 30 years, with approximately 1 in 180 babies born with congenital heart disease in the UK each year. Several cardiac diseases are genetic and can manifest in childhood. Most are primary cardiomyopathies, ion channel diseases, coronary artery disease from familial hypercholesterolaemia or aortopathies.
Women and cardiovascular risk
 |
|Management of hypertensive disorders in pregnancy
07 Aug 2019
Hypertension is the most common medical complication of pregnancy, affecting 8-10% of pregnancies in the UK. It is associated with risks to both the woman and the fetus, with increased risks of pre-eclampsia, preterm delivery, fetal growth restriction, placental abruption and perinatal death. Any new onset of hypertension after 20 weeks or symptoms or signs suspicious of pre-eclampsia should be referred for same day assessment at a secondary care antenatal assessment unit.
 |
|Underestimating risk in women delays diagnosis of CVD
21 Mar 2016
CVD remains the most common cause of mortality in women. There has been an increase in the prevalence of MI in women aged 35 to 54, while a decline in prevalence was observed in age-matched men. Although men and women share classic cardiovascular risk factors the relative importance of each risk factor may be gender specific. The impact of smoking is greater in women than men, especially in those under 50. Diabetes is a more potent risk factor for fatal CHD in women than men.
Research Reviews by GP with special interest
 |
|Diabetes raises risk of cardiovascular mortality in severe aortic stenosis
20 Dec 2022
Diabetes mellitus is strongly associated with death from heart failure and sudden death in patients with severe aortic stenosis (AS), a study from France has found. No such association was seen in patients with mild/moderate AS.
How useful is smartphone technology for detecting AF?
25 Oct 2022
Smartphone applications can allow self-detection of arrhythmias in patients with atrial fibrillation. However, current evidence of their usefulness is based on small low-quality studies, a systematic review and meta-analysis has found.
Loud noise at work and night shifts may raise risk of IHD
26 Sep 2022
Occupational exposure to high levels of noise, greater than 90?dBA, and night shift work appear to be associated with an increased risk of ischaemic heart disease, a population-based study from New Zealand has found. However, no such association was seen for long working hours and sedentary work.
 |
|Do indirect unscheduled care pathways affect outcomes in myocardial infarction?
27 Jul 2022
Indirect unscheduled care pathways were associated with higher mortality in patients admitted with myocardial infarction compared with direct pathways, a retrospective population-based study from Scotland has found.
 |
|All grades of aortic stenosis raise risk of death
24 Jun 2022
Even mild aortic stenosis is associated with an increased risk of mortality, a large study from Australia has found.
Younger age at onset of overweight associated with higher risk of hypertension
25 May 2022
Becoming overweight before the age of 60 was associated with a raised risk of hypertension, in a prospective cohort study. The risk was greatest in those who became overweight between the ages of 18 and 39.
Concomitant steroid therapy raises GI bleeding risk in AF patients on DOACs
25 Apr 2022
Oral glucocorticoids are associated with an increased risk of gastrointestinal bleeding in patients with atrial fibrillation concomitantly treated with direct acting oral anticoagulants, a nationwide study from Denmark has found.
 |
|Novel bleeding risk score for atrial fibrillation patients treated with DOACs
25 Mar 2022
A new, simple risk score for predicting major bleeding in patients with nonvalvular atrial fibrillation treated with direct acting oral anticoagulants (DOACs) has been developed by researchers in Israel.
 |
|Sex differences identified in cardiovascular outcomes
24 Jan 2022
Women who had survived a first coronary event had a significantly lower risk of major adverse cardiovascular events and recurrent coronary heart disease than men, a population-based cohort study has found. However, women had a higher risk of stroke, heart failure, and all-cause mortality compared with men.
Can choice of anticoagulant for AF influence risk of incident dementia?
20 Dec 2021
Dementia and mild cognitive impairment were less common among patients prescribed direct oral anticoagulants for newly diagnosed atrial fibrillation (AF) compared with those prescribed vitamin K antagonists, in a UK cohort study.
 |
|Depression questionnaires fail to reflect patients’ own views of mood changes
20 Dec 2021
Changes in depression questionnaire scores often disagree markedly with patients’ own ratings of changes in their mood, a prospective cohort study has found.
ECG-based tool aids rapid risk assessment for a cardiac cause of syncope
20 Dec 2021
In patients with a syncopal event, a combination of seven ECG criteria enabled a rapid assessment of the likelihood that the event was due to a cardiac cause, in a prospective multicentre trial.
Editorials
 |
|Is exercise as effective as drug therapy in reducing systolic BP?
23 Jan 2019
The systolic blood pressure lowering effect of endurance or dynamic resistance exercise among hypertensive populations appeared similar to that of commonly used antihypertensive medications (ACE inhibitors, angiotensin-2 receptor blockers, beta-blockers and diuretics) in a network meta-analysis.
 |
|Fish oil supplements fail to lower cardiovascular risk in diabetes
22 Nov 2018
Dietary supplementation with n-3 fatty acids (fish oils) in patients with diabetes is not associated with a reduction in cardiovascular events, a large randomised controlled study has found. ‘These findings, together with results of earlier randomised trials involving patients with and those without diabetes, do not support the current recommendations for routine dietary supplementation with n-3 fatty acids to prevent vascular events,’ the study authors conclude.

