CPD frameworks
These frameworks, associated with all articles, prompt drafting of personal learning, reflection and planning.
Save your reflective note into your device or cloud
Fillable PDF frameworks
Adobe reader needed for tablets
Word frameworks - for reflective practice
Click to download
Reflection on a journal article
Stages of reflection on a situation
Reflection of a team, practice or group
External reference on reflection
Reflective practice in health care and how to reflect effectively
Koshy K, Limb C et al. International Journal of Surgical Oncology. 2017 2:e20
CARDIOVASCULAR MEDICINE
Prompt diagnosis and treatment will improve heart failure outcomes
27 Oct 2021
The majority of new diagnoses of heart failure (HF) are made only after the patient has deteriorated to the point of requiring hospital admission. Within a month of admission with HF, 1 in 4 patients who survive to discharge will be readmitted, and 1 in 8 will die. Ischaemic heart disease is the most common cause of HF, accounting for at least half of diagnoses: following a heart attack, 1 in 3 patients will develop HF within 5 years. Hypertension, diabetes and obesity are also associated with an increased risk of HF.
Detecting and managing atrial fibrillation in primary care
27 Oct 2021
Atrial fibrillation (AF) is often diagnosed as an incidental finding during a routine medical check. The prevalence increases with age and the presence of CVD further increases the risk of AF. Around 15-30% of patients with AF are asymptomatic. When patients present to their GP the most common symptoms of AF include: palpitations, chest pain, breathlessness and a reduction in exercise/functional capacity. To establish a diagnosis of AF, rhythm documentation with an ECG showing at least 30 seconds of AF is required.
 |
|Suspected cardiac syncope requires urgent investigation
27 Oct 2020
Around 40% of people experience a syncopal event during their lifetime. Cardiac syncope accounts for 10% of presentations. Incidence rises significantly with age. Assessment should be systematic: a thorough history, physical examination including lying and standing BP and 12-lead ECG. The medical history and physical examination are key. If following initial assessment cardiac syncope is suspected patients should be referred for urgent specialist cardiovascular assessment or emergency admission.
 |
|Diagnosis and management of abdominal aortic aneurysm
27 Oct 2020
Risk factors for abdominal aortic aneurysm formation include: smoking, increasing age, and family history. Men over the age of 65 are most commonly affected, with an abdominal aortic aneurysm present in approximately 1%. As the condition is normally asymptomatic, most patients have their aneurysms discovered through the screening programme or incidentally via other imaging investigations. Patients with a new diagnosis of an abdominal aortic aneurysm should be referred to their local vascular service.
 |
|More patients could benefit from referral for cardiac rehabilitation
25 Nov 2019
Cardiac rehabilitation is a combination of medical and behavioural interventions designed to facilitate recovery and prevent future cardiovascular disease events. A cardiovascular prevention and rehabilitation programme (CPRP) is a critical element within the management pathway for most patients with heart disease and has a particularly strong evidence base for those with either symptomatic atherothrombotic vascular disease or heart failure. Following acute MI and/or coronary revascularisation, attending and completing a CPRP is associated with an absolute risk reduction in cardiovascular mortality from 10.4% to 7.6%.
 |
|Reducing stroke risk in patients with atrial fibrillation
25 Nov 2019
Stroke is the most debilitating complication of atrial fibrillation (AF). AF-related strokes account for 20-25% of all strokes and are generally more severe and disabling and more likely to recur. Oral anticoagulation (OAC) remains the cornerstone of AF management with a clear prognostic benefit. It reduces stroke risk by two-thirds and mortality by a quarter. The decision to anticoagulate is taken irrespective of the pattern and duration of AF (paroxysmal, persistent or permanent). A large evidence base supports the use of OAC in men with a CHA2DS2-VASc score of 2 or more and women with a score of 3 or more. Hence, in the absence of absolute contraindications, OAC is strongly recommended.
 |
|Tracking down and treating the cause of syncope
22 Oct 2018
Syncope is a transient loss of consciousness (T-LOC) caused by cerebral hypoperfusion, characterised by a rapid onset, short duration and spontaneous complete recovery. It needs to be differentiated from other conditions that can cause T-LOC such as seizures, trauma, hypoglycaemia, and psychogenic causes. Three principal types of syncope can be identified: reflex or neurally mediated, orthostatic hypotensive and cardiac. The common denominator of all these conditions is low systemic BP causing global cerebral hypoperfusion.
Managing stable angina in primary care
22 Oct 2018
Around 50% of people diagnosed with ischaemic heart disease present with stable angina as the first symptom. The likelihood of a diagnosis of angina increases with the number of cardiovascular risk factors present. A resting 12-lead ECG is recommended for all patients with suspected angina. However, a normal result does not exclude the presence of underlying coronary artery disease.
Improving uptake of cardiac rehabilitation
23 Oct 2017
Data from the National Audit of Cardiac Rehabilitation show that 50% of eligible MI, PCI, and CABG patients do attend cardiac rehabilitation and that figure continues to rise, but the rates for stable angina and heart failure remain low. There is evidence that programmes which have a basis in psychoeducation (goal setting, self-monitoring, relapse prevention) are more likely to achieve long-term behaviour change than those based simply on delivering a fixed agenda of exercise and education. A recent Cochrane review of exercise-based cardiac rehabilitation continues to show the benefit of exercise prescription in terms of cardiovascular mortality, hospital readmission rates, and quality of life.
 |
|Assessment and management of CVD risk in adults
23 Oct 2017
Cardiovascular disease (CVD) affects seven million people in the UK alone. Modifiable risk factors for CVD include smoking, abnormal lipid profile, hypertension, diabetes, abdominal obesity, psychosocial factors, diet, alcohol consumption, and lack of physical activity. The INTERHEART study concluded that these factors account for more than 90% of the risk of MI worldwide. Well validated studies have suggested that QRISK2 is a better predictor of a patient’s ten-year risk of CVD compared with the traditionally used Framingham equation.
Prompt diagnosis of AF lowers risk of complications
24 Oct 2016
Estimates suggest an AF prevalence as high as 2% in adults with an exponential relationship with increasing age. Opportunistic screening for silent AF is recommended in at-risk groups. AF is associated with a 1.5-2 fold increased risk of death, and is responsible for 20-30% of all strokes. The CHA2DS2-VASc risk stratification score is recommended to assess stroke risk in patients with AF. Risk of severe bleeding with warfarin should also be assessed using the HAS-BLED score.
 |
|Early recognition vital in acute coronary syndrome
24 Oct 2016
Acute coronary syndrome (ACS) includes both ST (STEMI) and non ST elevation (NSTEMI) MI, and unstable angina. Patients with ACS typically present with chest pain; classically central chest pain that radiates to the left arm. Additional symptoms include dyspnoea, nausea, sweating and syncope. However, patients can present atypically with gastric symptoms. These are often more common in patients with diabetes, women and the elderly. A 12-lead ECG should be performed if possible within 10 minutes of presentation or ideally at first contact with the emergency services.
 |
|Underestimating risk in women delays diagnosis of CVD
21 Mar 2016
CVD remains the most common cause of mortality in women. There has been an increase in the prevalence of MI in women aged 35 to 54, while a decline in prevalence was observed in age-matched men. Although men and women share classic cardiovascular risk factors the relative importance of each risk factor may be gender specific. The impact of smoking is greater in women than men, especially in those under 50. Diabetes is a more potent risk factor for fatal CHD in women than men.
Management of heart failure with preserved ejection fraction
21 Oct 2015
Heart failure affects nearly one million people in the UK. Half of these patients have normal, or near normal, left ventricular ejection fraction and are classified as heart failure with preserved ejection fraction (HFpEF). Newer imaging techniques have confirmed that systolic function in HFpEF patients is not completely normal, with reduced long axis function and extensive but subtle changes on exercise. Patients are likely to be older women with a history of hypertension. Other cardiovascular risk factors, such as diabetes mellitus, atrial fibrillation and coronary artery disease are prevalent in the HFpEF population.
Playing it safe:exercise and cardiovascular health
21 Oct 2015
Regular physical activity controls acquired cardiovascular risk factors such as obesity, diabetes mellitus, hypertension and hyperlipidaemia. Exercise is generally associated with a 50% reduction in adverse events from coronary artery disease. Active individuals are at lower risk of developing certain malignancies including cancer of the prostate and the colon, osteoporosis, depression and dementia. Individuals who exercise regularly extend their life expectancy by three to seven years. Healthy individuals should engage in 150 minutes of moderate-intensity aerobic exercise per week. Even lower volumes of exercise confer health benefits, which is highly relevant to individuals with established cardiac disease including heart failure.
 |
|Diagnosis and management of inherited cardiomyopathies
23 Oct 2014
Inherited heart conditions are the most common cause of sudden cardiac death in those under the age of 35 and the leading cause of non-traumatic death in young athletes. In many cases the first manifestation of an inherited cardiomyopathy can be a sudden cardiac arrest. Other presentations include chest pain or breathlessness during exertion, palpitations and syncope. Hypertrophic cardiomyopathy is the most common inherited heart disease affecting 1 in 500 of the population. Some patients may exhibit severe left ventricular hypertrophy, others may show nothing more than an abnormal ECG.
 |
|Have a high index of suspicion for atrial fibrillation
23 Oct 2014
The lifetime risk of atrial fibrillation (AF) for men and women over the age of 40 is about 25%. The condition affects around 800,000 people in the UK, of which it is estimated that 250,000 are undiagnosed. A rapid heart rate may result in palpitations, dyspnoea or chest tightness, whereas loss of atrial contractility may lead to fatigue and reduced exercise capacity. In patients with a confirmed diagnosis of AF, three areas need to be considered: stroke risk, symptoms, and risk of tachycardia cardiomyopathy.
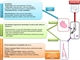 |
|Risk stratification key in patients with syncope
05 Dec 2013
An episode of loss of consciousness is highly likely to be syncope if it is complete, transient, has rapid onset and short duration, with associated loss of postural tone and is followed by a spontaneous and complete recovery without sequelae. The initial assessment in patients with suspected syncope should aim to confirm the syncopal nature of the episode, identify the most likely cause of syncope and stratify the risk of major cardiovascular events or sudden arrhythmic death.
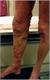 |
|Improving the management of varicose veins
05 Dec 2013
Up to 30% of the UK population are affected by varicose veins. Patients with bleeding varicose veins should be referred to a vascular service immediately. Referral is also indicated in the following cases: symptomatic primary or recurrent varicose veins; lower limb skin changes thought to be caused by chronic venous insufficiency; superficial vein thrombosis and suspected venous incompetence; a venous leg ulcer or healed venous leg ulcer.
Identifying patients at risk of sudden arrhythmic death
24 Oct 2012
Most GPs will encounter at least one case of sudden arrhythmic death syndrome (SADS) during their career. They may have to evaluate a young person at risk of SADS or offer support and screening to family members. GPs are usually the first point of call for families who have experienced the loss of a young relative. In England alone, SADS is responsible for 544 deaths per year. A significant proportion of cases may be preventable. First-degree relatives should be referred to an expert cardiac centre for comprehensive evaluation to identify individuals at risk.
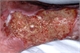 |
|Early diagnosis of peripheral arterial disease can save limbs
24 Oct 2012
The prompt identification and management of patients with peripheral arterial disease (PAD) can improve quality of life, save limbs and reduce cardiovascular events. NICE has published a clinical guideline on lower limb peripheral arterial disease. NICE recommends that a supervised exercise programme is offered to all patients with intermittent claudication. Patients with severe and inadequately controlled symptoms should be referred to secondary care services.
 |
|ABPM is best for diagnosing hypertension in primary care
20 Oct 2011
The diagnosis of hypertension has traditionally been based on clinic blood pressure (BP) but home and ambulatory measurements are better correlated with cardiovascular outcomes. A recent systematic review and cost-effectiveness study found that ambulatory blood pressure monitoring (ABPM) is more accurate than both clinic and home monitoring in diagnosing hypertension. A diagnostic strategy for hypertension using ABPM, following an initial raised clinic reading, would reduce misdiagnosis and be cost saving for the NHS. Only about one in every twenty diagnoses is made with an ABPM machine, and these are largely confined to larger GP practices and specialist units.
 |
|Tailor treatment to the patient in stable angina
19 Oct 2011
Stable angina is a chronic condition which may persist for years. It affects a significant proportion of the population, and is more common with advancing age. According to the 2006 Health Survey for England, angina affects 8% of men and 3% of women aged 55-64 increasing to 14% and 8% respectively for men and women aged 65-74. Symptoms of angina can be alarming and distressing and it is therefore important that patients understand the underlying problem and what therapies are available to improve or abolish their symptoms.
 |
|Chest pain of recent onset requires prompt diagnosis
23 Jun 2010
The new NICE guidance on recent onset chest pain urges GPs to assess the nature and timing of acute pain rapidly and arrange urgent admission for suspected acute coronary syndrome (ACS).
Managing unstable angina and non-ST elevation MI
22 Jun 2010
Acute coronary syndrome (ACS), encompassing unstable angina (UA), non-ST elevation myocardial infarction (NSTEMI), and ST-elevation myocardial infarction (STEMI), is often the result of an acute thrombotic occlusion of the coronary vessels, associated with atheromatous plaque rupture or erosion. ACS is associated with a severely impaired prognosis and requires prompt and efficient specialist treatment. The GP plays a major role in ensuring optimal patient management after hospital discharge and secondary prevention of cardiovascular events.
 |
|Managing familial hypercholesterolaemia
01 Jun 2009
Familial hyper-cholesterolaemia (FH) is a relatively common genetic disorder. The heterozygous form affects 1 in 500 people in the UK, i.e. 0.2% of the population. However, the vast majority of patients remain undiagnosed. FH is a risk factor for the development of premature atherogenesis. All first-degree relatives, not just the children, of FH patients have a 50% risk of having the condition; and should be traced and tested, a process known as cascade testing. Until such services become widely available, the BHF has recommended that, relatives of a patient with FH should be advised to visit their GP to be evaluated and, preferably, referred for a DNA test.
 |
|Cardiac rehabilitation should be tailored to the patient
01 Jun 2009
The'Care closer to home' initiative in the UK has seen a shift of cardiac rehabilitation services from the hospital to a community setting. Community-based services are preferred by many patients and have been shown to be feasible and effective. The traditional hospital-based programme is divided into four phases. The other widely used model is a six-week, home-based programme using written and audiotape materials. Exercise-based CR results in a 20% reduction in all cause mortality and a 25% reduction in total cardiac mortality.

