CPD frameworks
These frameworks, associated with all articles, prompt drafting of personal learning, reflection and planning.
Save your reflective note into your device or cloud
Fillable PDF frameworks
Adobe reader needed for tablets
Word frameworks - for reflective practice
Click to download
Reflection on a journal article
Stages of reflection on a situation
Reflection of a team, practice or group
External reference on reflection
Reflective practice in health care and how to reflect effectively
Koshy K, Limb C et al. International Journal of Surgical Oncology. 2017 2:e20
CARE OF THE ELDERLY
Optimising the recognition of Lewy body dementia
25 May 2022
Lewy body dementia is a heterogeneous condition that is often difficult to treat. It is associated with higher rates of neuropsychiatric symptoms, inpatient admission and carer stress, as well as shorter survival, than other dementia subtypes. Core clinical features are: fluctuating cognition with pronounced variations in attention and alertness; recurrent visual hallucinations; REM sleep behaviour disorder; one or more features of spontaneous parkinsonism. Recurrent visual hallucinations occur in up to 80% of patients.
 |
|Diagnosis and management of acute coronary syndrome
25 May 2022
The term acute coronary syndrome (ACS) describes a range of conditions, including unstable angina, non-ST-elevation myocardial infarction (NSTEMI) and ST-elevation myocardial infarction (STEMI), which are associated with a sudden reduction of blood flow to the heart. Its presentation is broad, and can include chest pain, cardiac arrest, haemodynamic instability, or cardiogenic shock. Urgent assessment of patients presenting with chest pain is crucial to the outcome as ACS treatment is time sensitive.
Diagnosing anxiety disorders in older adults can be challenging
25 Jan 2021
In older adults, the prevalence of anxiety disorders is higher among those with other health problems, and those in hospital and care settings. A primary depressive disorder should be excluded whenever an older person presents with anxiety symptoms for the first time, and comorbid anxiety often indicates a more severe presentation of depression. Around four in five patients have a comorbid physical disorder. Medical conditions can mimic symptoms of, predispose to, or even directly precipitate an anxiety disorder, and may colour its symptomatology or limit treatment options.
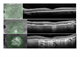 |
|Diagnosis and management of age-related macular degeneration
25 Jan 2021
Age-related macular degeneration (AMD) is a cause of painless, gradual loss of vision. Epidemiological evidence suggests 4-8% of people aged over 65 years in the UK have visually significant AMD. Patients with suspected neovascular AMD (NvAMD) should be seen by ophthalmology within two weeks, and if the diagnosis and progressive disease are confirmed, treatment should commence within the same timeframe. Intravitreal anti-vascular endothelial growth factor (anti-VEGF) agents cause regression of neovascularisation and reduce macular oedema. There is no treatment for dry AMD.
 |
|Identifying the cause of late life psychosis
23 Jan 2020
Late life psychosis may be caused by organic conditions including: delirium, dementia, drug intoxication or withdrawal, or a general medical condition. In these situations there should be evidence of a temporal relationship between the psychosis and the underlying condition. Around 60% of older adults presenting with new onset psychosis have an identifiable underlying organic cause. If an underlying medical condition can be excluded, and there is no evidence to support a diagnosis of delirium or dementia, then the cause of psychosis may be functional. This is more likely if there is a family or personal history of mental illness.
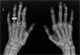 |
|Elderly onset RA: a diagnostic and therapeutic challenge
23 Jan 2020
Elderly onset rheumatoid arthritis (EORA) is defined as rheumatoid arthritis (RA) with age of first onset 65 years or over. It comprises an acute onset proximal or large joint arthritis with a prominent systemic syndrome characterised by constitutional symptoms and a higher ESR than in the younger patient with RA. Investigations should focus on trying to establish the cause and ruling out differential diagnoses. They should include inflammatory markers, serum uric acid, full blood count, rheumatoid factor/anti-CCP antibodies, and X-rays of the affected joint as well as the hands and feet. The possibility of malignancy should always be borne in mind. NICE recommends urgent referral of all suspected cases.
 |
|Diagnosing and treating mood disorders in older people
05 Feb 2019
Depression in older adults is common. Depressive symptoms may be part of a recurrent depressive disorder or experienced for the first time in later life as a result of changes in risk and resilience factors. There is an association between cerebrovascular pathology, vascular risk factors and depression. Physical illnesses, particularly those associated with frailty, are also important risk factors for depression. Depression has a distinct presentation in late life and low mood may not be the predominant presenting symptom. Older patients may present with physical symptoms, apathy, cognitive symptoms, agitation, retardation, fatigue or weight loss.
 |
|Managing arrhythmias in coronary artery disease
23 Jan 2019
A detailed history is essential in patients with coronary artery disease (CAD) to elucidate red flag symptoms necessitating urgent specialist assessment. Red flags include syncope and presyncope, particularly in patients with concomitant left ventricular systolic dysfunction. Palpitations with severe chest pain and breathlessness also warrant urgent assessment. Undiagnosed atrial fibrillation (AF) is common in older populations. LVEF of 35% or less is a predictor of increased risk of sudden death. All patients with CAD should therefore undergo assessment of LVEF, usually by transthoracic echocardiography.
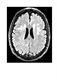 |
|Timely diagnosis of vascular dementia key to management
23 Jan 2018
Vascular dementia is the second most common type of dementia, after Alzheimer’s disease, and accounts for 15% of cases. The core diagnostic features include cognitive impairment in at least two domains (orientation, attention, language, visuospatial function, executive function, motor control and praxis), which affect social or occupational function, together with evidence of cerebrovascular disease (focal neurological signs or neuroimaging). Crucially there should be a temporal relationship between cerebrovascular disease and the onset of cognitive changes.
 |
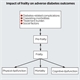
|Pulmonary rehabilitation improves exercise capacity and quality of life
23 Jan 2018
Pulmonary rehabilitation is a multifaceted programme of exercise and education that aims to improve breathlessness, exercise capacity, and quality of life, and aid self-management. Patients with chronic respiratory failure, those on long-term or ambulatory oxygen and patients with anxiety and depression can all benefit from rehabilitation. It is one of the most beneficial and cost-effective treatments for COPD and should be considered a fundamental component of disease management rather than an option.
 |
|Frailty predicts adverse outcomes in older people with diabetes
23 Jan 2017
In older people living with diabetes, geriatric syndromes, which indicate frailty, are emerging as a third category of complications in addition to the traditional microvascular and macrovascular sequelae. Frailty is defined by the presence of three or more phenotypes (weight loss, weakness, decreased physical activity, exhaustion and slow gait speed). Patients may progress from a non-frail to pre-frail or frail state. With timely intervention, there is a greater chance of an individual recovering from pre-frail to non-frail than deteriorating into frailty.
 |
|Depression is linked to dementia in older adults
23 Jan 2017
Depression and dementia are both common conditions in older people, and they frequently occur together. Rather than a risk factor, depression with onset in later life is more likely to be either prodromal to dementia or a condition that unmasks pre-existing cognitive impairment by compromising cognitive reserve. The distinction between depression and early dementia may be particularly difficult. Detailed histories obtained from patients and their relatives as well as longitudinal follow-up are important.
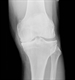 |
|Controlling joint pain in older people
25 Jan 2016
The prevalence of chronic pain in older people in the community ranges from 25 to 76% and for those in residential care, it is even higher at 83 to 93%. The most common sites affected are the back, hip, or knee, and other joints. There is increased reporting of pain in women (79%) compared with men (53%). Common conditions include osteoarthritis and, to a lesser extent, the inflammatory arthropathies such as rheumatoid arthritis. The differential diagnosis includes non-articular pain such as vascular limb pain and nocturnal cramp, some neuropathic pain conditions (such as compressive neuropathies and postherpetic neuralgia), soft tissue disorders such as fibromyalgia and myofascial pain syndromes.
 |
|Anxiety in older adults often goes undiagnosed
25 Jan 2016
Anxiety disorder in the elderly is twice as common as dementia and four to six times more common than major depression. Anxiety is associated with poorer quality of life, significant distress and contributes to the onset of disability. Mortality risks are also increased, through physical causes, especially cardiovascular disease, and suicide. Diagnosing anxiety disorders in older adults remains a challenge because of the significant overlap in symptoms between physical disorders and depression.
 |
|Diagnosis and management of postherpetic neuralgia
22 Jan 2015
Risk factors for postherpetic neuralgia (PHN) include: increasing age; a prodrome of pain before rash onset; the degree of spread of the rash, particularly if it extends beyond a single dermatome; and severity of pain during the acute attack. Forty per cent of patients over 50 and 75% of those over 75 develop PHN following resolution of the rash. Patients with severe pain or those whose condition is affecting their daily activities and function should be referred to a specialist in pain management.
Establishing the cause of memory loss in older people
22 Jan 2015
Common causes of memory loss in older people are mild cognitive impairment, the various types of dementia, and psychiatric illness, mainly depression. Around 10% of patients with mild cognitive impairment progress to dementia each year. NICE guidance suggests examination of: attention, concentration, short- and long-term memory, praxis, language and executive function.
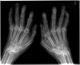 |
|Early recognition improves prognosis in elderly onset RA
22 Jan 2014
Age at onset is particularly relevant in RA as the presentation may differ in elderly onset RA (EORA) compared with young onset RA (YORA). Patients with EORA frequently report a more acute presentation, especially if positive for rheumatoid factor (RF). Fever, fatigue and weight loss appear to be more common in EORA. Although small joints are most frequently involved in the RA population overall, there is common involvement of large joints in EORA and these proximal symptoms may mimic polymyalgia rheumatica (PMR). [With external links to the evidence base]
 |
|Can exercise prevent cognitive decline?
22 Jan 2014
As the tolerability of pharmacological agents decreases with age, exercise may be particularly helpful as a possible treatment or stabiliser of mood and cognitive function in older age. The effects of exercise on reducing depressive symptoms are not dissimilar to the effects of antidepressant drugs and cognitive behaviour therapy. Exercise has a moderate effect on the ability of people with dementia to perform activities of daily living and may improve cognitive function. Midlife exercise may also have an impact on later cognitive function.
Tailor treatment in the older patient with type 2 diabetes
24 Jan 2013
In older people, diabetes is a disabling disease due to the associated vascular complications, multiple comorbidities and the increased prevalence of geriatric syndromes. Because of the complexity of diabetes in old age a comprehensive assessment is important at initial diagnosis, with the aim of preventing loss of autonomy and preserving independence. Cognitive and physical dysfunction are common in older people with diabetes which may affect health outcomes and quality of life. Individual therapeutic targets should take into consideration functional status, life expectancy and patient preferences.
Early diagnosis beneficial in Alzheimer’s disease
24 Jan 2013
A diagnosis of Alzheimer’s disease requires clinical and pathological evidence. In clinical practice, GPs should consider a diagnosis of dementia when a patient presents with functional impairment (e.g. needing a greater level of help with activities of daily living, struggling to manage own finances and bills) in addition to at least two changes in cognitive function e.g. short-term memory, language, reasoning, spatial orientation, or personality change. The patient, friends, family or professional carers should have noticed these changes for at least six months. Early diagnosis enables early, planned intervention, reduces crisis situations, delays planned admission to care homes (and helps prevent unplanned admissions).
 |
|Diagnosing and managing vascular dementia
24 Jan 2012
Vascular dementia (VaD) is common. Pure vascular disease may account for 5–20% of all cases of dementia, while mixed dementia, Alzheimer's disease (AD) with VaD, occurs at least as frequently. It is unusually heterogeneous and frequently overlapping and comorbid with other conditions such as stroke, other cardiovascular and cerebrovascular diseases and their risk factors, as well as AD. There is no specific treatment or cure for VaD, but its proximity to other conditions may make it amenable to interventions at various stages of the disease.
 |
|Tackling anxiety and depression in older people in primary care
23 Jan 2012
Old age is often a time of loss: of physical health, sensory capacity, cognitive function, independence, work, income and social support. The diagnosis of anxiety and depression in older patients is difficult. There is a complex relationship between depression and physical illness, there is uncertainty regarding diagnostic criteria and the PHQ-9 should probably not be used. We are more likely to recognise late life anxiety and depression if we are aware of the risk factors and the less obvious ways in which patients can present.
 |
|Preventing osteoporotic fractures in older people
24 Jan 2011
Until recently, the management of osteoporosis was centred around the use of diagnostic thresholds based on bone mineral density (BMD) measured at the spine or hip by dual x-ray absorptiometry (DXA). This was reflected in UK guidance for the identification of individuals at high fracture risk from the Royal College of Physicians (RCP).The guidance was based on an opportunistic case-finding strategy where physicians were alerted to the possibility of osteoporosis and high fracture risk by the presence of clinical risk factors associated with fracture. This provided a trigger for the measurement of BMD, and treatment was considered in those with a BMD value that lay in the range of osteoporosis as defined by the WHO. Treatment was, however, also recommended for women with a prior fragility fracture without necessarily measuring BMD. Since the development of these guidelines, it has become apparent that the presence of several of the risk factors used to trigger a BMD test is associated with a fracture risk greater than can be accounted for by BMD alone. [With external links to the evidence base]
Tackling dementia in patients with Parkinson’s disease
24 Jan 2011
Cognitive symptoms in patients with Parkinson's disease are associated with more rapid deterioration and eventually, a two-fold increase in mortality. Patients with cognitive impairment place a greater burden on their care givers and many such patients are admitted to nursing homes. Primary care plays a significant role in the recognition of DLB and PDD. Early recognition and referral to a specialist memory clinic can help to educate the patient about their often worrying symptoms and initiate the relevant treatment. Through the involvement of the multidisciplinary team, appropriate care networks can be set up to provide support and education for both patients and carers.
Diagnosing joint pain in older people
20 Jan 2010
Musculoskeletal disease is the most common cause of chronic pain and disability in older people. The prevalence in those over 75 is 83% in the UK. Older adults with arthritis have been reported to make significantly greater use of medical services compared with those without.Joint pathology may lead to reduced mobility, increased risk of falls, low energy, dependency and depression. Chronic pain itself is strongly associated with psychological distress and fatigue. Overall, arthritis places an enormous burden on the individual and on society. Therefore, the importance of correctly diagnosing and managing joint pain in the elderly is paramount and the GP is central to this process. [With external links to the evidence base]
Managing Alzheimer's disease in primary care
01 Jan 2009

