Mental health - Special interest
Mental health in older people
Diagnosing anxiety disorders in older adults can be challenging
25 Jan 2021
In older adults, the prevalence of anxiety disorders is higher among those with other health problems, and those in hospital and care settings. A primary depressive disorder should be excluded whenever an older person presents with anxiety symptoms for the first time, and comorbid anxiety often indicates a more severe presentation of depression. Around four in five patients have a comorbid physical disorder. Medical conditions can mimic symptoms of, predispose to, or even directly precipitate an anxiety disorder, and may colour its symptomatology or limit treatment options.
 |
|Identifying the cause of late life psychosis
23 Jan 2020
Late life psychosis may be caused by organic conditions including: delirium, dementia, drug intoxication or withdrawal, or a general medical condition. In these situations there should be evidence of a temporal relationship between the psychosis and the underlying condition. Around 60% of older adults presenting with new onset psychosis have an identifiable underlying organic cause. If an underlying medical condition can be excluded, and there is no evidence to support a diagnosis of delirium or dementia, then the cause of psychosis may be functional. This is more likely if there is a family or personal history of mental illness.
Psychiatry symposium
 |
|Assessing and managing depression in patients with dementia
24 Jun 2022
The relationship between depression and dementia is complex. Depression appears to be an independent risk factor for incident dementia, conferring a two-fold increase in dementia risk. Depression may represent an early sign or prodromal feature of dementia. The association between depression and dementia appears to strengthen as the interval between the two disorders shortens. Depression may also be a consequence of dementia.
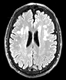 |
|Diagnosis and management of vascular dementia
24 Jun 2022
Vascular dementia describes chronic progressive impairment of cognitive function arising from cerebrovascular injury. The presentation of vascular dementia is often insidious, with disorganisation, loss of drive, irritability, mental rigidity, difficulties with planning and problem solving, emotional lability and other mood changes, and sometimes inappropriate or disinhibited social behaviour. Physical examination may identify gait impairment, bradykinesia, rigidity, and focal neurological signs.
Paediatric mental health
 |
|Optimising the management of depression in children
24 Jul 2020
In a large meta-analysis, the prevalence of depression was twice as common in adolescents (5.7%) than children (2.8%). The 2:1 female to male ratio of depression seen in adults becomes apparent from the age of 12 years. Three quarters of children aged 3-17 years with depression also have anxiety, and almost half have associated behaviour problems. Depression should be treated by child and adolescent mental health services unless the episode is mild and of < 2-3 months’ duration.
 |
|Diagnostic assessment key in autism spectrum disorder
22 Jun 2020
Autism spectrum disorder (ASD) is a complex pervasive neurodevelopmental disorder with an estimated lifetime prevalence of 1%. ASD presents across a wide range of intellectual ability and persists throughout life. Core symptoms include abnormal social interaction and communication, restricted and repetitive interests or activities, associated with lack of cognitive flexibility, and unusual sensory responses. ASD is highly heritable and polygenic. The male:female ratio of ASD is 3:1. Although the behavioural presentation has a childhood onset, approximately 40% of children with ASD are undiagnosed.
PTSD
 |
|Treating psychological trauma in the real world
23 Jan 2020
After a potentially traumatic event (PTE), many individuals experience either no distress or only transient distress, while others suffer considerable morbidity and may develop post-traumatic stress disorder (PTSD). Around one-third of people experiencing a PTE will develop PTSD, though this varies depending on the type of traumatic event and rates of PTSD are higher with type 2 trauma. Type 2 trauma involves repeated traumatic experiences over extended periods. Although PTSD symptoms can be present acutely, the diagnosis requires the persistence of symptoms for at least one month and the symptoms should cause functional impairment.
Identifying patients with complex PTSD
01 Aug 2016
Type 2 or complex trauma results from multiple or repeated traumatic events occurring over extended periods. Complex trauma is often associated with other adversity and stressors such as neglect, loss or deprivation. For many individuals these traumas occur at a developmentally vulnerable time with the perpetrator often in a caregiving role. Patients who have experienced complex trauma should be assessed for the core symptoms of PTSD. In addition, patients should be assessed for disturbances in the three domains of emotional dysregulation, negative self-concept and interpersonal disturbances.
Women's mental health
Prompt detection vital in postpartum mood disorders
24 Jun 2019
Common mental health disorders affect around one in five women during pregnancy and the first year following childbirth. Depression and anxiety disorders are the most prevalent mental health disorders during this period as they are at other times of life. It is important to distinguish postnatal depression from baby blues, which is common and requires no treatment, although it is a potential risk factor for postnatal depression. Postpartum psychosis affects 1 in 1,000 women and can develop very quickly in the first two weeks postpartum, often requiring urgent admission to a specialised mother and baby unit. One in six women with bipolar disorder will develop postpartum psychosis.
 |
|Be vigilant for perinatal mental health problems
23 Mar 2015
The postnatal period appears to be associated with higher rates of adjustment disorder, generalised anxiety disorder, and depression. Women who have a history of serious mental illness are at higher risk of developing a postpartum relapse, even if they have been well during pregnancy. Postnatal depression is more severe than baby blues, follows a chronic course and may relapse outside the perinatal period. Bipolar disorder may present as a first depressive episode in pregnancy or the postnatal period. In the postpartum period women have a high risk of severe relapse.
Editorials
 |
|What is the role of the Edinburgh Postnatal Depression Scale?
22 Mar 2021
The optimal cut-off score of the Edinburgh Postnatal Depression Scale is 11, a systematic review and meta-analysis has found. However 7-8 women out of 10 with a positive screen will not have major depression.
 |
|Loneliness a potential risk factor for depression
21 Feb 2021
Loneliness is associated with an increased risk of developing depression, a longitudinal cohort study has found. The English Longitudinal Study of Ageing (ELSA) recruited 11,391 participants aged 50 years and over who were living in a private household in 2002. Participants were followed up every two years until 2016/17.
Research reviews: Mental health
OCD associated with increased risk of substance use disorder
24 Jun 2022
Patients with obsessive-compulsive disorder (OCD) are nearly four times more likely to develop substance use disorder than those without OCD, a Swedish cohort study has found. This association may be partially attributed to genetic factors, but environmental factors may also be involved.
Discontinuing antidepressants too early raises risk of relapse
27 Oct 2021
Patients who had been taking antidepressants for at least 9 months and felt well enough to stop were more likely to relapse by 52 weeks if their treatment was discontinued compared with those who carried on with their current therapy, a UK primary care study has found.

