Special Interest: Diabetes
Editorials
 |
|Diabetes triples risk for occlusive vascular events in women
25 Mar 2019
Diabetes is known to increase the risk of occlusive vascular events, and this is one of the main causes of premature death associated with the condition. A recent meta-analysis of nearly one million individuals has shown that the risk of occlusive events in diabetes is doubled for men but tripled for women. Importantly, this study was able to control for other major vascular risk factors.
 |
|Fish oil supplements fail to lower cardiovascular risk in diabetes
22 Nov 2018
Dietary supplementation with n-3 fatty acids (fish oils) in patients with diabetes is not associated with a reduction in cardiovascular events, a large randomised controlled study has found. ‘These findings, together with results of earlier randomised trials involving patients with and those without diabetes, do not support the current recommendations for routine dietary supplementation with n-3 fatty acids to prevent vascular events,’ the study authors conclude.
Major articles related to diabetes
 |
|Reducing cardiovascular risk pivotal in diabetic kidney disease
21 Feb 2021
Diabetic kidney disease is associated with a very high risk of cardiovascular disease (CVD) and premature mortality from cardiovascular events. There is good evidence that multifactorial interventions that optimise BP, limit proteinuria and minimise cardiovascular risk can reduce morbidity and premature mortality. Early diabetic kidney disease is asymptomatic. Microalbuminuria, defined as a urinary ACR of 3-30 mg/mmol on two occasions three months apart is the earliest clinically detectable indicator of diabetic kidney disease. Excellent glycaemic control can delay onset of microalbuminuria.
 |
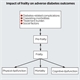
|Improving pain control in diabetic neuropathy
22 Mar 2017
Diabetic neuropathy is thought to affect 1.9% of the world’s population and 50% of patients with a diagnosis of diabetes mellitus which would equate to 2.25 million people in the UK. The term diabetic neuropathy includes multiple distinct clinical entities that have been classified under the broad headings of focal and multifocal neuropathies and symmetrical neuropathies. Peripheral diabetic neuropathy, a chronic distal symmetrical predominantly sensory neuropathy, is the most common form of diabetic neuropathy. The common presentation is of painful symptoms originating in the feet, that then spread to the knees before involving the distal portion of the upper limbs in a ‘glove and stocking’ distribution.
 |
|Frailty predicts adverse outcomes in older people with diabetes
23 Jan 2017
In older people living with diabetes, geriatric syndromes, which indicate frailty, are emerging as a third category of complications in addition to the traditional microvascular and macrovascular sequelae. Frailty is defined by the presence of three or more phenotypes (weight loss, weakness, decreased physical activity, exhaustion and slow gait speed). Patients may progress from a non-frail to pre-frail or frail state. With timely intervention, there is a greater chance of an individual recovering from pre-frail to non-frail than deteriorating into frailty.
 |
|Set individualised targets for patients with type 2 diabetes
23 Sep 2016
In type 2 diabetes regular physical activity totalling 30 minutes most days of the week improves muscle insulin sensitivity, lipid profile and blood pressure although a total of 60-75 minutes a day is required for weight reduction and better metabolic profiles. NICE guidelines acknowledge the need for individualised treatment targets. Lowering HbA1c is beneficial in reducing microvascular complications and may have macrovascular benefits in the long term. However, intensive glycaemic control in the elderly with more advanced disease may not have similar benefits and poses a risk due to hypoglycaemia.
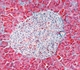 |
|Improving the detection and management of type 1 diabetes
25 Jan 2016
Type 1 diabetes affects around 370,000 adults in the UK, about 10% of all those diagnosed with diabetes. In type 1 diabetes there is a lack of beta cell insulin secretion as a result of autoimmune destruction of the beta cells. However, patients are not affected by insulin resistance, and so do not routinely experience the features of metabolic syndrome that occur in type 2 diabetes. It is therefore important to classify the type of diabetes correctly and to recognise that type 1 diabetes is a condition with its own management requirements. Structured education is the cornerstone of care providing tools to allow effective self-management.
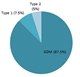 |
|Improving outcomes in diabetes in pregnancy
21 May 2015
One in 250 pregnancies in the UK involves diabetes. The majority of cases (87.5%) are gestational diabetes, 7.5% are type 1 and 5% are type 2 diabetes. Diabetes in pregnancy is associated with a five fold increase in risk of stillbirth and a two-fold increased risk of congenital defects compared with the general maternity population. Women with gestational diabetes have a significant lifetime risk of developing type 2 diabetes, hence diabetes screening must be undertaken on an annual basis in primary care.
 |
|Managing patients with type 2 diabetes and obesity
22 Jan 2015
Diabetes risk increases exponentially with increasing BMI particularly if fat accumulates centrally and/or in the skeletal muscle, liver and other organs such as the pancreas. Those with diabetes and co-existing obesity, particularly if it is severe, are also at risk of other obesity-related conditions, such as cardiovascular disease, obstructive sleep apnoea, joint pain, many cancers and depression. Supporting patients to lose weight should be considered a key goal of diabetes care for all overweight and obese patients with type 2 diabetes.
Risk factor control is key in diabetic nephropathy
24 Feb 2014
Prolonged duration of diabetes, poor glycaemic control and hypertension are major risk factors for both diabetic nephropathy and cardiovascular disease. Optimising blood sugar control together with excellent control of blood pressure can reduce the risk of developing diabetic nephropathy. Diabetic nephropathy should be considered in any patient with diabetes when persistent albuminuria develops.
Tailor treatment in the older patient with type 2 diabetes
24 Jan 2013
In older people, diabetes is a disabling disease due to the associated vascular complications, multiple comorbidities and the increased prevalence of geriatric syndromes. Because of the complexity of diabetes in old age a comprehensive assessment is important at initial diagnosis, with the aim of preventing loss of autonomy and preserving independence. Cognitive and physical dysfunction are common in older people with diabetes which may affect health outcomes and quality of life. Individual therapeutic targets should take into consideration functional status, life expectancy and patient preferences.
 |
|Identifying patients at risk of type 2 diabetes
21 Aug 2012
In July 2012, NICE published guidance on the identification and management of type 2 diabetes in adults who are at high risk. This new NICE guidance dovetails with the NHS Health Check programme. The guidance advises using a validated risk assessment tool to identify patients at risk of diabetes. NICE recommends that high-risk patients should be offered a programme encouraging them to undertake a minimum of 150 minutes of moderate intensity physical activity a week, gradually lose weight to reach and maintain a BMI within the healthy range, increase consumption of whole grains, vegetables, and other foods that are high in dietary fibre, reduce the total amount of fat in their diet and eat less saturated fat.
Clinical reviews of research - by GPwSI diabetes
Lowering blood pressure may prevent the onset of diabetes
27 Jul 2022
Antihypertensive therapy with ACE inhibitors and angiotensin ll receptor blockers lowers the risk of developing type 2 diabetes, a meta-analysis has shown.
 |
|Loneliness associated with increased risk of type 2 diabetes
21 Dec 2020
A study based on the English Longitudinal Study of Ageing (ELSA) suggests that loneliness is an independent risk factor for diabetes.
Long-term PPI use associated with increased risk of type 2 diabetes
24 Nov 2020
Regular use of proton pump inhibitors (PPIs) increased the risk of type 2 diabetes in a cohort analysis of three large American population studies. The risk increased with longer duration of use.
Prediabetes associated with increased risk of CVD and all-cause mortality
27 Oct 2020
A meta-analysis has shown an association between prediabetes and raised risk of all-cause mortality and incident cardiovascular disease in the general population as well as patients with atherosclerotic heart disease.
Diet rich in whole grain foods may lower risk of diabetes
24 Sep 2020
Higher consumption of total whole grain foods, such as oatmeal, dark bread, brown rice or whole grain cereals can reduce the risk of developing type 2 diabetes, analysis of data from three large prospective cohort studies in the USA has shown.
 |
|Healthy lifestyle associated with longer life expectancy free of diabetes
22 Jun 2020
A large cohort study has demonstrated that a healthy lifestyle in midlife can increase life expectancy free of type 2 diabetes, as well as cardiovascular disease (CVD) and cancer.
SGLT2 inhibitors reduce risk of serious renal events
25 May 2020
A Scandinavian observational study has shown that sodium-glucose co-transporter 2 (SGLT2) inhibitors are associated with a significant reduction in serious renal events compared with dipeptidyl peptidase-4 (DPP-4) inhibitors. The study used Scandinavian disease registry data to compare population outcomes in the general diabetic population rather than selected groups of high-risk patients.
 |
|Exercise can improve functional status in diabetic neuropathy
24 Mar 2020
Physiotherapy to improve ankle strength and balance produced sustained improvements in functional status in patients with diabetic peripheral neuropathy, in a study from Singapore.
 |
|Diabetes during pregnancy raises risk of early CVD in offspring
24 Feb 2020
Diabetes of any type in pregnant women increases the risk of early onset cardiovascular disease (CVD) in their childen, a study from Denmark has found.
Is the incidence of diabetes declining?
25 Nov 2019
A recent systematic review, published in the BMJ, has concluded that in countries where data is available the incidence of diabetes has been stable or falling since 2006.
Incidence of type 2 diabetes varies markedly between occupations
24 Oct 2019
Men employed as professional drivers, and manufacturing or agricultural workers were three times more likely to develop type 2 diabetes compared with university teachers and architects, in a national study from Sweden.
Omega-3 fatty acid supplements do not prevent or improve type 2 diabetes
25 Sep 2019
Supplementary long chain polyunsaturated fatty acids (PUFA) such as omega-3 have no effect on the prevention of diabetes or on glucose metabolism, a large meta-analysis commissioned by the World Health Organization (WHO) has found.
 |
|Lack of legacy effect from tight glycaemic control in type 2 diabetes
07 Aug 2019
Adults with type 2 diabetes who had received intensive glucose lowering therapy for nearly six years had a lower risk of cardiovascular events than those who received standard therapy only during the prolonged period in which the HbA1C curves were separated, a study from the US has found. There was no evidence of a legacy effect or a mortality benefit with intensive glucose control 15 years after commencement of the study.
Controlling risk factors in type 2 diabetes reduces excess risk
24 Jun 2019
Patients with type 2 diabetes who have well controlled risk factors have little or no excess risk of stroke, myocardial infarction or death, a retrospective cohort study has found.
 |
|Do 5 alpha-reductase inhibitors raise the risk of type 2 diabetes?
22 May 2019
Finasteride and dutasteride appear to be associated with a modest increase in the risk of developing type 2 diabetes, according to the findings of a retrospective cohort study.
SGLT2 inhibitor produces good glycaemic control in everyday practice
24 Apr 2019
An observational study from Scotland has shown that dapagliflozin produced equivalent improvements in glycaemic control in patients with type 2 diabetes in general practice to those reported in clinical trials.

