CPD frameworks
These frameworks, associated with all articles, prompt drafting of personal learning, reflection and planning.
Save your reflective note into your device or cloud
Fillable PDF frameworks
Adobe reader needed for tablets
Word frameworks - for reflective practice
Click to download
Reflection on a journal article
Stages of reflection on a situation
Reflection of a team, practice or group
External reference on reflection
Reflective practice in health care and how to reflect effectively
Koshy K, Limb C et al. International Journal of Surgical Oncology. 2017 2:e20
Early diagnosis RATs for primary care
UK Risk Assessment Tool
QCancer
UK Early diagnosis programme
Macmillan - early diagnosis
US: National Cancer Institute
PDQ® (Physician Data Query) is NCI's cancer database of peer-reviewed, regularly updated evidence-based, referenced summaries
Women
Breast
Ovarian
Endometrial screening
Endometrial
Cervical
Men
Prostate prevention
Prostate screening
Testicular screening
Penile
Other cancers
Colorectal screening
Colon
Rectal
Liver cancer screening
Renal
Lung
Risk factors
Smoking in cancer care
Cancer research UK
Statistics UK
Statistics World
Mortality UK
Cancer deaths UK
Deaths - selected cancers
Projections
Projected mortality UK
Projections by cancer type
Cancer - Special interest
Articles are complemented with links to external websites. These enable instant access to the current evidence base. They include:
- Links to the US National Cancer Institute's database of peer-reviewed, regularly updated evidence-based summaries
- Links to the results of pre-defined search requests made to PubMed
- Links to the results of pre-defined search requests made to 'NHS Evidence', the database of evidence provided by the UK's National Institute for Health and Care Excellence
Major articles on cancer
 |
|Early detection of cutaneous melanoma improves prognosis
24 Sep 2021
Exposure to intermittent intense sunlight and sunburn (especially in childhood) are the most common modifiable risk factors for melanoma. Individuals with lighter skin tones are at greatest risk (Fitzpatrick skin types I-II). A history of melanoma increases the risk of a further melanoma eight-fold. Approximately 5-10% of melanoma cases are estimated to be familial. The 7-point checklist is recommended by NICE to help determine when a referral is indicated. However, checklists should not be used in isolation as some melanomas will be missed. Amelanotic melanomas, estimated at 10% of all melanomas, remain a challenge.
Prevention, diagnosis and treatment of colorectal cancer
26 Jul 2021
Colorectal cancer is the third most common cancer in both women and men and is the second most common cause of cancer death in the UK. The main symptoms patients with colorectal cancer present with are: persistent blood in faeces; persistent change in bowel habit and persistent lower abdominal pain. Less obvious presentations are unexplained weight loss, tiredness for no reason, general malaise and iron deficiency anaemia found on blood testing.
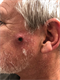 |
|Improving the detection of cutaneous squamous cell carcinoma
25 Jun 2021
Cutaneous squamous cell carcinoma (cSCC) can develop de novo or from pre-existing chronic actinic damage, although the probability and speed of transition from actinic keratosis to cSCC is highly variable. The occurrence of cSCC is related to chronic UV exposure, particularly occupational exposure. Risk factors include fairer skin, significant exposure to sunlight or PUVA. Incidence is also significantly increased in patients who are immunosuppressed. All patients with suspected cSCC should be referred via the two-week wait pathway to dermatology.
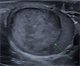 |
|GPs should have a high index of suspicion for testicular cancer
22 Apr 2021
Most men with testicular cancer present with a lump that they have identified in their scrotum. Although the scrotal swelling is usually painless, pain is the first symptom in around 20% of patients, typically a dull or dragging ache in the testicle or a heaviness in the scrotum. NICE recommends that all men who have a non-painful enlargement or change in shape or texture of their testis should be referred urgently to urology using the two-week wait pathway. In men who have unexplained or persistent testicular symptoms, an urgent direct access testicular ultrasound scan should be requested.
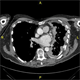 |
|Diagnosis and management of malignant pleural mesothelioma
21 Dec 2020
Mesothelioma accounts for less than 1% of all cancers in England, Wales and Northern Ireland. There are almost 2,500 new diagnoses a year, of which 96% are pleural. The median age at diagnosis for malignant pleural mesothelioma (MPM) is 76 years. The majority of cases occur in men, most commonly following occupational exposure to asbestos. There is a latent period, usually 30-40 years, between exposure and disease development. A chest X-ray is usually the first-line investigation; 94% of patients with MPM have a unilateral pleural effusion, although the chest X-ray may be normal or show another asbestos-related lung disease.
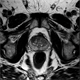 |
|Optimising the management of early prostate cancer
23 Apr 2020
Men born after 1960 in the UK now have a 1 in 6 estimated lifetime risk of being diagnosed with prostate cancer. NICE recommends that men over 50 years old who request a PSA test should be fully counselled about the test beforehand. The test should also be offered to men with LUTS or an abnormal DRE. If the prostate feels malignant on DRE this should trigger a fast track referral to secondary care, via a suspected cancer pathway referral, even if the PSA is normal. Men with PSA values above the age-specific reference range should also be referred to urology urgently, via a suspected cancer pathway referral.
.jpg) |
|Time to diagnosis key in improving lung cancer outcomes
25 Nov 2019
NICE recommends urgent referral via a suspected cancer referral pathway to the two week wait service if: chest X-ray findings suggest lung cancer or if patients aged 40 and over have unexplained haemoptysis. However, studies have indicated that around 20-25% of patients with confirmed lung cancer may have a chest X-ray reported as normal and this figure may be higher for early stage lung cancers. Therefore, the National Optimal Lung Cancer Pathway recommends that where there is a high suspicion of underlying malignancy (but the chest X-ray is normal), GPs should refer patients directly for a CT scan.
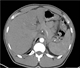 |
|Early detection of liver cancer key to improving outcomes
07 Aug 2019
Hepatocellular carcinoma (HCC) accounts for around 90% of liver cancer cases and intrahepatic cholangiocarcinoma (CC) for 9-10%. Most cases of HCC occur in the context of chronic liver disease with cirrhosis, particularly in those with chronic hepatitis B or C. Other major risk factors include excessive alcohol consumption, obesity and aflatoxins. Overall, 10-15% of cirrhotic patients will develop HCC within 20 years. Patients presenting with an upper abdominal mass consistent with an enlarged liver should be referred for an urgent direct access ultrasound scan within two weeks.
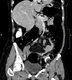 |
|Diagnosing and managing colorectal cancer
25 Jul 2018
Colorectal cancer is the fourth most common cancer in the UK and is the second most common cause of cancer deaths. Most cancers are thought to develop from colonic adenomas and incidence is strongly related to age. The majority of cancers are left sided and typically present with a change in bowel habit, blood in the stool or colicky abdominal pain. Rectal cancers can present with fresh red bleeding and large tumours can cause tenesmus (the intense and frequent desire to defecate, with little or no stool passed). Right-sided cancers most often present with anaemia. In both right- and left-sided cancers occasionally the patient may notice an abdominal mass or inexplicable weight loss.
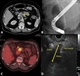 |
|Improving outcomes in pancreatic cancer
25 Jul 2018
The combination of an aggressive disease, vague presenting symptoms and insensitive standard diagnostic tests is a key factor contributing to poor outcomes with only 15% of patients with pancreatic cancer having operable disease at diagnosis. The NICE guideline on referral for suspected cancer recommends urgent referral via a suspected cancer pathway referral if the patient is aged 40 and over with jaundice. It also recommends that an urgent direct access computerised tomography (CT) scan referral should be considered in patients aged 60 and over with weight loss and any of the following: diarrhoea; back pain; abdominal pain; nausea; vomiting; constipation; new onset diabetes. Pancreatic cancer requires a CT scan for diagnosis.
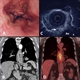 |
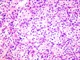
|Diagnosis and management of oesophageal cancer
22 Feb 2018
Oesophageal cancer commonly presents with dysphagia or odynophagia and can be associated with weight loss and vomiting. Referral for urgent endoscopy should always be considered in the presence of dysphagia regardless of previous history or medication. NICE recommends urgent referral (within 2 weeks) for direct access for upper GI endoscopy in patients with dysphagia and those aged 55 years or over with weight loss and any of the following: upper abdominal pain, reflux, or dyspepsia.
 |
|Prompt investigation improves outcomes for kidney cancer
22 Feb 2018
Renal cell carcinoma should be suspected in the presence of: localising symptoms such as flank pain, a loin mass or haematuria; constitutional upset including weight loss, pyrexia and/or night sweats; or unexplained test results. Smoking, obesity and hypertension are common risk factors and all three demonstrate a dose-response relationship with the relative risk of renal cell carcinoma.
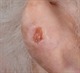 |
|Improving detection of non-melanoma skin cancer
05 Aug 2015
Basal cell carcinomas (BCCs) and squamous cell carcinomas (SCCs) are clinically and pathologically distinct and both are locally invasive. However, while BCCs rarely metastasise, SCCs have the potential to do so especially when they arise on the ears or lips. Patients with one non-melanoma skin cancer (NMSC) have a higher risk of developing another NMSC and of malignant melanoma.
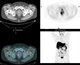 |
|New developments in metastatic prostate cancer therapy
23 Apr 2015
Advanced prostate cancer remains an incurable and lethal disease. Innovation continues to provide new hope for patients with advanced disease, with improved survival while maintaining quality of life. As patients live longer with increasing treatment options, education of all healthcare professionals involved in their care is crucial in ensuring holistic care for this complex disease.
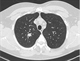 |
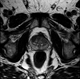
|Early diagnosis pivotal to survival in lung cancer
24 Nov 2014
Lung cancer is the most common cause of cancer death, both in the UK and worldwide. There has been little change in survival over the past 20 years, with increasing evidence that there are disparities in outcomes between the UK and other comparable healthcare systems. It has been postulated that this is due to an excess of early deaths, delays in diagnosis are thought to contribute to this problem. A recent study showed that 30% of patients with lung cancer die within the first 90 days and they have seen their GP on average five times in the four months before diagnosis, suggesting there may be opportunities to diagnose these patients earlier in the disease process. The challenge GPs face is to identify and refer those at risk as early as possible and to maintain a high index of suspicion if symptoms persist. [With external links to current evidence base]
 |
|GPs could play key role in prostate cancer survivorship programmes
24 Nov 2014
More than 80% of men diagnosed with prostate cancer can expect to survive for at least five years. Up to 87% of men with prostate cancer may have unmet supportive care needs. Patients regularly cite psychological and sexual issues as the most significant. Poor functional outcomes after treatment such as incontinence and erectile dysfunction have a major impact on quality of life. The key elements of a survivorship programme are: education, intervention, surveillance and co-ordination of care. Interventions which may improve immediate care include: structured holistic needs assessment and care planning, treatment summaries and cancer care reviews, patient education and support events and advice about, and access to, physical activity schemes. [With external links to the evidence base]
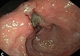 |
|Early endoscopy improves survival in gastric cancer
25 Jul 2014
Gastric cancer often presents late and the mortality ratio remains one of the highest compared with more common cancers. Early diagnosis improves survival in this potentially curable cancer. Dysphagia, weight loss and age over 55 are significant predictors of cancer. All patients presenting with dyspepsia and either alarm features or known conditions that increase the risk of gastric cancer should be referred for urgent endoscopy. Given that the majority of gastric cancer cases occur in people over 55, urgent endoscopy is also recommended in patients in this age group with new uncomplicated dyspepsia prior to treatment, even without alarm symptoms or if the symptoms respond to treatment. [With external links to current evidence base]
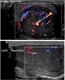 |
|GPs have key role in managing men with testicular cancer
22 Apr 2014
Testicular cancer accounts for 1% of all malignancies in males. However, it is the most frequently occurring solid tumour in men between the ages of 15 and 34 years. Testicular tumours have excellent cure rates, even in those with metastases, as they are extremely sensitive to chemotherapy and radiotherapy. Early diagnosis is, however, very important as treatment is more successful and less intensive, and long-term health consequences can be minimised. [With external links to current evidence and summaries]
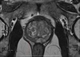 |
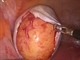
|Optimising the management of early prostate cancer (2014)
22 Apr 2014
A suspicion of a diagnosis of prostate cancer is usually based on either induration or nodularity of the prostate on digital rectal examination or, more commonly, a rise in serum prostate specific antigen (PSA) level. The usual cut-off point for PSA is taken as 4 ng/ml, but in men below 65 a value of more than 2.5 ng/ml should raise suspicion. The Gleason grading of any cancer identified is an important part of the decision-making process concerning the need for active treatment, as opposed to surveillance alone. Gleason pattern 6 cancers are regarded as low risk, Gleason 7 intermediate risk and 8-10 high risk. [With external links to the current evidence base]
 |
|Detecting ovarian disorders in primary care
20 Mar 2014
Ovarian cysts occur more often in premenopausal than postmenopausal women. Most of these cysts will be benign, with the risk of malignancy increasing with age. Symptoms which may be suggestive of a malignant ovarian cyst, particularly in the over 50 age group, include: weight loss, persistent abdominal distension or bloating, early satiety, pelvic or abdominal pain and increased urinary urgency and frequency. [With external links to the current evidence base]
 |
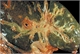
|Prompt diagnosis key in bladder cancer
22 Jan 2014
Bladder cancer is the most frequently diagnosed cancer involving the urinary tract. Delayed diagnosis is associated with high-grade muscle invasive disease which has the potential to progress rapidly, metastasise and is often fatal. Haematuria which is typically intermittent, frank, painless and at times present throughout micturition is the classical and most common presentation of bladder cancer. However, irritative symptoms such as dysuria, urgency, urge incontinence and frequency as well as obstructive symptoms i.e. feeling of incomplete voiding, intermittent stream and straining can also be experienced. [With external links to the current evidence base]
 |
|Improving the detection and treatment of liver cancer
25 Jul 2013
Liver cancer is the sixth most common cancer worldwide. Over the past decade survival in liver cancer has been steadily improving as a result of developments in surgery, transplantation and the introduction of a number of novel local, ablative and molecular targeted therapies. [With external links to current evidence and summaries]
 |
|GPs have key role in early detection of melanoma
24 Jun 2013
Lesions which have a high index of suspicion for melanoma should not be removed in primary care. Patients should be referred urgently to secondary care with a history recording the duration of the lesion, change in size, colour, shape and symptoms.
 |
|Is there a link between BPH and prostate cancer?
25 Apr 2012
GPs are playing an increasing role in managing both prostate cancer and benign prostatic hyperplasia (BPH). More than 70% of men over 70 years are affected by BPH, and prostate cancer is the most common cancer in men in the UK. GPs play an important part in the initial management of men presenting with lower urinary tract symptoms and in addressing concerns regarding prostate cancer and the significance of the patient’s symptoms. While there is no proven causal link between prostate cancer and BPH, associations have been found. BPH may increase the chance of an incidental prostate cancer being diagnosed through PSA testing and other investigations. [With external links to current evidence and summaries]
 |
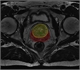
|Postmenopausal bleeding should be referred urgently
21 Mar 2012
All women with postmenopausal bleeding should be referred urgently. Endometrial cancer is present in approximately 10% of cases. First-line investigation is a transvaginal ultrasound scan. A normal TVUS is reassuring, and if examination is normal further investigation is not required, providing the bleeding has stopped. There is no evidence to indicate whether different patterns of postmenopausal bleeding such as one-off bleeding or more frequent bleeds are more likely to be associated with malignancy. [With external links to current evidence and summaries]
 |
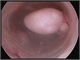
|Improving outcomes in lung cancer patients
23 Nov 2011
Lung cancer is the leading cause of cancer mortality in the UK resulting in more than 33,500 deaths in 2008, 4,000 more than for bowel and breast cancer combined. Five-year survival figures are poor but have recently improved from around 5% to 7.5% in men and 8.5% in women.There is evidence of marked variation in the standard of care in England. It has recently been shown that if patients are first referred to a thoracic surgical centre, rather than a hospital that does not have thoracic surgeons on site, they are 51% more likely to have a resection. There are similar findings for other active treatments. By reducing this variation there is scope for marked improvement in outcomes, possibly to levels seen in other countries such as Australia, Canada, Sweden and Norway where five-year survival rates are approximately double. Thus there is a need to encourage lung cancer teams to select patients correctly so that the best treatment can be offered. Improving diagnosis, staging and fitness assessment was a major focus in the recently updated NICE guideline on diagnosis and treatment of lung cancer, published in April 2011. [With external links to current evidence and summaries]
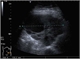 |
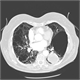
|Improving early detection of ovarian cancer
22 Jun 2011
Ovarian cancer is the fifth most common cancer in women. The incidence has increased over the past 20-25 years, particularly in the 65 and over age group. The outcome for women with ovarian cancer is generally poor, with an overall five-year survival rate of less than 35%. The survival rates for women with ovarian cancer in the UK are significantly lower than the European average. Despite recommendations, published by NICE in 2005, on referral of patients with suspected cancer, the majority of women diagnosed with ovarian cancer are not electively referred via the ovarian cancer two-week pathway. They are often referred to the wrong specialty or present as emergencies. NICE has now published a clinical guideline on the diagnosis and initial management of ovarian cancer. [With external links to current evidence and summaries]
Early detection of melanoma improves survival
01 Oct 2009
The incidence of melanoma has risen over the past 30 years but most of this increase involves early melanomas which have less impact on mortality. This may explain why mortality has not changed in parallel with incidence as flat rates and even downturns have been observed in most Caucasian populations.
Editorials
 |
|Patients at increased suicide risk following cancer diagnosis
22 Feb 2019
Cancer patients are at increased risk of suicide, particularly in the first six months after diagnosis, a national population-based study in England has found. Compared with the general population, cancer patients had a 20% increased risk of suicide; standardised mortality rate (SMR) 1.20. The risk of suicide was highest during the first six months after diagnosis, SMR 2.74 (95% CI: 2.52-2.98), but remained raised for three years.
 |
|Combined oral contraceptive pill lowers ovarian cancer risk
22 Oct 2018
Women who use the combined oral contraceptive pill (COCP) are at reduced risk of developing ovarian cancer, a benefit that persists for several years after cessation, a nationwide cohort study from Denmark has found.
 |
|MP-MRI could improve the diagnosis of prostate cancer
22 Feb 2017
Multi-parametric magnetic resonance imaging (MP-MRI) could play an important role in triaging men with a raised PSA for prostate biopsy and improve the detection of clinically significant prostate cancer, findings from a UK study suggest.
 |
|Active monitoring vs treatment for localised prostate cancer
24 Oct 2016
No significant difference in prostate cancer mortality was seen in men with localised prostate cancer who underwent active monitoring compared with surgery or radiotherapy at ten years’ follow-up in ProtecT, a large UK trial. However, both surgery and radiotherapy were associated with lower rates of metastasis and disease progression. ProtecT seems to support the use of active monitoring/surveillance in low-risk patients, but this does not mean that it is a sensible option for all men newly diagnosed with prostate cancer. Most men in ProtecT had low Gleason grade, low-risk disease and the findings must not be used to push men with more aggressive disease away from active treatment.
 |
|DRE has vital role in early detection of prostate cancer
22 Jan 2015
Digital rectal examination is important, not just for reducing concern in men with urinary symptoms, large prostates and borderline PSA levels, but also because it is recognised that a significant number of men have clinically significant prostate cancer despite a normal PSA. [With external links to the evidence base]
 |
|Obesity, metformin and prostate cancer risk
15 Dec 2014
A total of 104 global studies were reviewed, examining nearly 10 million (9,855,000) men and 191,000 cases of prostate cancer. The analysis concluded that being overweight or obese significantly increases the risk of advanced prostate cancer. The link between obesity and advanced prostate cancer is important for primary care. In order to maximise the benefit from PSA testing of asymptomatic men, we should be trying to target higher-risk men and should now think of adding obesity to that list. [With external links to the evidence base]
 |
|Collaborative care effective in cancer patients with depression
23 Oct 2014
Integrated collaborative care substantially improves outcomes for cancer patients with major depression, a UK study has found. GPs have an important role in recognising depression in cancer patients and should bear in mind the high prevalence of depression when carrying out QOF cancer reviews. This study suggests that treatment is unlikely to be effective unless it incorporates some form of enhanced care. GPs may not have access to collaborative care but can provide case management and liaise with local oncology teams.
 |
|HPV vaccination uptake lowest in young women at greatest risk
22 Apr 2014
Teenage girls most at risk of cervical cancer are least likely to be offered HPV vaccination and, those who are, less likely to complete the course, a cross-sectional study of sexual health service users has found. [With external links to current evidence and summaries]
 |
|Are 5-ARIs suitable for prevention of prostate cancer?
23 Oct 2013
As with the original Prostate Cancer Prevention Trial, the use of a 5-ARI, in this case finasteride, was seen to reduce the incidence of prostate cancer by about a third. Although high-grade cancer was more common in the 5-ARI group, after 18 years of follow-up there was no significant difference in rates of prostate cancer specific survival or overall survival between the two groups. Prescription of finasteride or dutasteride as a chemopreventive agent against prostate cancer cannot be justified on the available evidence. [With external links to current evidence and summaries]
 |
|PSA in men in their 40s predicts risk of prostate cancer death
23 Sep 2013
For many men, three lifetime PSA tests (mid to late 40s, early 50s and at age 60 years) would be sufficient screening to identify the small number of men developing clinically significant prostate cancer, allowing resources to be concentrated on those at higher risk, a study in the BMJ concludes. The European Association of Urology recommends that all men aged 40-45 years should be offered a baseline PSA to ‘initiate a risk-adapted follow-up approach with the purpose of reducing prostate cancer mortality and the incidence of advanced and metastatic cancer’.
PSA at 60 may predict risk of death from prostate cancer
20 Oct 2010
The debate on PSA screening to detect prostate cancer is ongoing. Two large studies published in 2009 gave an unclear message. The European ERSPC trial showed a significant reduction in prostate cancer mortality as a result of screening but with a significant risk of overtreatment in order to save lives (48 additional patients requiring treatment for each life saved). The American PLCO study showed no benefit from screening, but has been criticised for the large amount of PSA testing outside the study in the control arm, contaminating the results and potentially diluting any benefit.A meta-analysis incorporating these two studies and four other randomised controlled trials (a total of 387,286 men), published in the BMJ, has examined the overall evidence for PSA screening. [With external links to current evidence and summaries]
Photoguide
 |
|Skin malignancy
25 Jul 2014
• Acanthosis nigricans • Morphoeic basal cell carcinoma • Primary cutaneous anaplastic large cell lymphoma • Amelanotic melanoma • Dermatofibrosarcoma protuberans • Squamous cell carcinoma [With external links to current evidence and summaries]
Clinical reviews
Does vasectomy increase the risk of prostate cancer?
23 Sep 2014
Vasectomy may be associated with a small increase in absolute risk of prostate cancer, the findings from a large cohort study in the United States suggest. A cohort of 49,405 men taking part in the Health Professionals Follow-Up Study, run by Harvard University, was followed up from 1986 to 2010. During this period 12,321 men (25%) had vasectomies. [With external links to the current evidence base]
Do CT scans in childhood raise cancer risk?
25 Jul 2013
Undergoing CT scans during childhood is associated with a small but significant risk of developing cancer, a large data linkage study from Australia has found. The absolute excess incidence rate for all cancers combined was 9.38 per 100,000 person-years at risk after nearly ten years’ follow-up.

