Tidman M J. Improving the management of rosacea in primary care. Practitioner 2014;258 (1775):27-30
Improving the management of rosacea in primary care
23 Oct 2014
AUTHORS
Dr Michael J. Tidman MD FRCP (Edin) FRCP (Lond), Consultant Dermatologist, Department of Dermatology, Royal Infirmary of Edinburgh, Edinburgh, UK
Article
Rosacea, also termed acne rosacea, is a common chronic inflammatory disorder.
It is more common in women than men and although it affects all ethnic groups it is seen more frequently in fair-skinned individuals. The condition usually occurs in the middle years of life, although rarely children and adolescents may be affected.
Rosacea only very occasionally involves areas other than the face, and tends to localise to the cheeks, forehead, chin and nose, sometimes showing marked asymmetry.
The term rosacea does not define a single clinical pattern, rather a variety of manifestations that may occur individually or co-exist with each other, and that may evolve over time.1
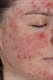
It is usually characterised by erythematous papules, pustules and occasionally plaques (papulopustular rosacea) which fluctuate in severity, typically on a background of erythema and telangiectasia, see figure 1.
In some individuals, facial redness can be prominent and permanent (erythemato-telangiectatic rosacea) see figure 2.
An important distinguishing feature from acne is a lack of comedones.
An uncomfortable accentuated blush reaction, with stinging, burning and pruritic sensations, may accompany rosacea. This is often triggered by stimuli such as hot drinks, alcohol, spicy food, warm weather, cold wind, strenuous exercise and emotion. Rosacea may be exacerbated by sunlight in some individuals, and a rosacea-like eruption is a potential side effect of corticosteroid therapy.
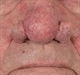
Hypertrophy of facial sebaceous glands, sometimes with fibrotic changes, may result in unsightly thickening of the skin (phymatous rosacea). Men, in particular, may develop marked enlargement and distortion of the nose, rhinophyma, see figure 3. In extreme cases, it may cause nasal obstruction. Occasionally, the predominant feature of rosacea is swelling of the eyelids and firm oedematous changes elsewhere on the face, referred to as lymphoedematous rosacea or Morbihan’s disease. It is not uncommon for rosacea sufferers to manifest features of seborrhoeic dermatitis as well.
Involvement of the eyes (ocular rosacea) is an important, underdiagnosed complication that may result in significant ocular morbidity, including blepharoconjunctivitis, chalazion, keratitis and corneal ulcers.2 There is often no correlation between the degree of ocular and cutaneous rosacea, and ocular rosacea may occur alone.1
A rare granulomatous form of rosacea has been described, acne agminata or lupus miliaris disseminatus faciei, manifesting as small inflammatory or flesh-coloured papules that resolve to leave scars.
Rosacea is a disfiguring condition that can have a major psychosocial impact,3 and its detrimental effect on emotional health and quality of life is frequently overlooked. The fact that it is often mistakenly associated with excessive alcohol consumption may lead to stigmatisation and serve to compound emotional distress.
Causes
The pathophysiology of rosacea is complex and still poorly understood.
It is presumed to involve a genetically determined dysfunction of both the neurovascular structures in the skin and the cutaneous elements of the innate and adaptive immune systems when an individual with rosacea is exposed to certain environmental and microbiological stimuli.4
The possible role of microbial agents continues to be debated.5 Increased colonisation of Demodex mites in skin affected by rosacea is well established: their aetiological significance is uncertain, but Bacillus oleronius, which is hosted by Demodex folliculorum mites, can produce pro-inflammatory mediators.4 There has also been speculation regarding a pathogenic role for Helicobacter pylori infection in the gastrointestinal tract, and there is some evidence that H. pylori eradication may have a beneficial effect on rosacea.6
Diagnosis
In the majority of cases, the diagnosis of rosacea is made without difficulty on the basis of the clinical features, although a dermatoscope to visualise micropustules and telangiectasia can be useful. Acne can usually be differentiated from rosacea by the presence of comedones, the involvement of extra-facial areas and the absence of flushing in the former disorder.
Other conditions that may be confused with rosacea include chronic photodamage, sarcoidosis, systemic lupus erythematosus, dermatomyositis, polymorphic light eruption, cutaneous B-cell lymphoma, carcinoid syndrome and adverse drug reactions, particularly with tyrosine kinase inhibitors and epidermal growth factor receptor inhibitors.7 Very occasionally, a skin biopsy for histological evaluation may be considered.
Management
When managing a chronic condition such as rosacea, for which there is no cure, it is important to provide adequate education and explanation, preferably backed up by written information, for example, the patient information leaflet produced by the British Association of Dermatologists (see Useful information box, p30), so that patient expectations regarding degree of improvement and the time scale to achieve this are realistic. Always bear in mind the psychological aspects of rosacea.
Mild/moderate papulopustular rosacea
The twice daily topical application of either 0.75% metronidazole, gel or cream, or 15% azelaic acid gel can be an effective and safe treatment for mild to moderate rosacea.8 However, neither preparation is recommended for long-term use (beyond a matter of months), but, once remission has been induced, they can subsequently be used intermittently when there is flaring of the condition. Both have the potential for skin irritation, although they are generally well tolerated.
Azelaic acid is a dicarboxylic acid, and as such has a mild depigmenting action that can be useful in combating the post-inflammatory hyperpigmentation that may occur in dark-skinned individuals.
Second-line topical therapies for rosacea include erythromycin, clindamycin, benzoyl peroxide, permethrin, retinoids and calcineurin inhibitors.8
Moderate/severe papulopustular rosacea
Tetracycline and oxytetracycline are licensed for the treatment of moderate to severe rosacea, and erythromycin and other macrolide antibiotics are an alternative if tetracyclines are contraindicated. Other tetracyclines are not licensed for rosacea, except for a recently introduced low-dose (40 mg daily), modified-release formulation of doxycycline, which takes advantage of its anti-inflammatory action at a sub-antibiotic dose:9 not only is this regimen effective, but it is also associated with fewer adverse effects.9
Systemic antibiotic therapy may be usefully combined with topical treatment to achieve a quicker response.9 Patients should be warned that these topical and oral anti-inflammatory measuresdo not improve erythema and telangiectasia, nor help symptoms of flushing.
In secondary care, oral isotretinoin therapy may benefit inflammatory rosacea recalcitrant to the standard therapies available in primary care, although, in contrast to its use in acne, prolonged remissions are unlikely.
Ocular rosacea
Involvement of the external eye surfaces by rosacea usually necessitates ophthalmological advice, and requires a combination of eyelid hygiene measures, oral antibiotics and ocular lubricants. Topical corticosteroids applied to the outer eye should be used only under specialist supervision.
Erythematotelangiectatic rosacea
This pattern of rosacea is particularly associated with flushing, and it is generally recommended that drugs that have a tendency to aggravate the blush reaction, for example, calcium channel blockers, be avoided when possible. Clonidine and beta-blockers, used off-label, may be helpful in managing this aspect of rosacea, although there is no firm evidence base for these treatments.
Laser surgery and intense pulsed light are proven physical methods of reducing the telangiectasia and, to a lesser extent, the erythema.10
Until recently, no effective treatment for the vascular changes was available in primary care, but this has changed with the introduction of brimonidine gel. Brimonidine is a selective alpha-2 adrenoceptor agonist that induces transient cutaneous vasoconstriction, and is newly approved for the treatment of persistent facial erythema associated with rosacea.8
Applied up to once a day, on an as required basis, it rapidly lightens the background redness of rosacea, and its effect lasts up to 12 hours. However, telangiectasias, lacking concentric smooth muscle in their walls, do not respond, and may be more obvious against the vasoconstricted skin.10
It is reasonably well tolerated, but some individuals experience exacerbation of flushing, pruritus and irritation of the skin.
It is contraindicated in those taking monoamine oxidase inhibitors and in patients on tricyclic or tetracyclic antidepressants.
Phymatous rosacea
Phymatous rosacea can be treated effectively by debulking and sculpturing of the affected areas with appropriate lasers or electrosurgery.10
Self-help measures
• Rosacea is often associated with ‘sensitive’ skin, and patients should be advised to avoid abrasive products and to use a non-comedogenic emollient to combat dryness
• Topical corticosteroid preparations should not be used, despite their apparent initial improvement of facial redness
• If flushing is pronounced, known trigger factors should be avoided, where possible
• A high sun protection factor sunscreen should be recommended when appropriate11
• For women, disguising reddened skin with make-up can be very helpful: in the case of florid erythema, cosmetic camouflage agents, available on prescription, are effective
Referral
Referral, on a routine basis, to a dermatologist should be considered if:
• The diagnosis is in doubt
• Papulopustular rosacea has not responded to a combination of topical and oral treatment after 8-12 weeks
• Flushing, phymatous changes, erythema and telangiectasia are causing emotional distress
Referral to an ophthalmologist should be considered:
• Urgently, if keratitis is suspected
• Routinely, if ocular symptoms do not respond to standard primary care treatment
Referral to a plastic or laser surgeon should be considered if:
• There is significant rhinophyma, particularly if it is causing nasal obstruction
Conclusion
Rosacea is a common inflammatory disorder, the aetiology of which remains poorly understood. Significant improvement can be achieved by treatments available in primary care. Consideration should always be given to the possibility of ocular involvement and the psychological impact of cutaneous rosacea.
REFERENCES
1 Del Rosso JQ, Thiboutot D, Gallo R et al. Consensus recommendations from the American Acne & Rosacea Society on the management of rosacea, part 1: a status report on the disease state, general measures, and adjunctive skin care. Cutis 2013;92(5):234-40
2 Vieira AC, Mannis MJ. Ocular rosacea: common and commonly missed. J Am Acad Dermatol 2013;69 (6 Suppl 1):S36-41
3 Moustafa F, Lewallen RS, Feldman SR. The psychological impact of rosacea and the influence of current management options. J Am Acad Dermatol 2014;pii:S0190-9622(14)01523-0
4 Steinhoff M, Schauber J, Leyden JJ. New insights into rosacea pathophysiology: a review of recent findings. J Am Acad Dermatol 2013;69(6 Suppl 1):S15-26
5 Holmes AD. Potential role of microorganisms in the pathogenesis of rosacea. J Am Acad Dermatol 2013;69(6):1025-32
6 Kutlubay Z, Zara T, Engin B et al. Helicobacter pylori infection and skin disorders. Hong Kong Med J 2014;20(4):317-24
7 Olazagasti J, Lynch P, Fazel N. The great mimickers of rosacea. Cutis 2014;94(1):39-45
8 Del Rosso JQ, Thiboutot D, Gallo R et al. Consensus recommendations from the American Acne & Rosacea Society on the management of rosacea, part 2: a status report on topical agents. Cutis 2013;92(6):277-84
9 Del Rosso JQ, Thiboutot D, Gallo R et al. Consensus recommendations from the American Acne & Rosacea Society on the management of rosacea, part 3: a status report on systemic therapies. Cutis 2014;93(1):18-28
10 Tanghetti E, Del Rosso JQ, Thiboutot D et al. Consensus recommendations from the American Acne & Rosacea Society on the management of rosacea, part 4: a status report on physical modalities and devices. Cutis 2014;93(2):71-6
11 Del Rosso JQ, Thiboutot D, Gallo R et al. Consensus recommendations from the American Acne & Rosacea Society on the management of rosacea, part 5: a guide on the management of rosacea. Cutis 2014;93(3):134-8

 = Registered users
= Registered users = Paid-up subscribers
= Paid-up subscribers