Aboshiha J. A case of recalcitrant bacterial conjunctivitis. Practitioner 2013; 257 (1766):25-28
A case of recalcitrant bacterial conjunctivitis
05 Dec 2013
AUTHORS
Mr Jonathan Aboshiha MA(Cantab) MRCS(Ed) FRCOphth, Clinical Research Fellow and Ophthalmology Specialist Registrar, Moorfields Eye Hospital, and UCL Institute of Ophthalmology, London, UK
Article
Eye problems account for around 2% of GP presentations,1 with more than half being given a diagnosis of conjunctivitis.2 In the UK, more than 3 million people now wear contact lenses,3 and this factor may be overlooked unless specifically enquired about in the patient’s ophthalmic history.
The following case highlights the need to ask directly about contact lens wear in all patients presenting with a red eye in primary care.
Case history
A 67-year-old lady presented to our eye casualty department with a six-week history of relapsing-remitting bacterial conjunctivitis. She had initially presented to a walk in clinic with a red right eye and a sticky yellow discharge, and was prescribed a five day course of chloramphenicol drops qds. There had been no change in her vision, and no complaint of a sensation that a foreign body was present. After three days her symptoms resolved, and she stopped using her chloramphenicol drops.
Two days later, the yellow sticky discharge and redness returned and she presented to her optician, who also prescribed a five day course of chloramphenicol drops qds, which again relieved her symptoms. This time she completed the course and was symptom free for a further two days.
She then presented to her GP, with a return of her symptoms. A conjunctival swab was taken and her GP prescribed a further course of chloramphenicol drops. The swab grew an isolate of staphylococcal species that was sensitive to chloramphenicol, and again her symptoms were relieved while she was on the drops.
A few days after completing her antibiotic course the symptoms returned and she presented to the A&E department of her local hospital, where she was again prescribed a course of chloramphenicol eye drops, which once more temporarily relieved her symptoms.
When her symptoms returned for the fifth time in six weeks, she presented to our eye casualty department.
She believed that her problems had all stemmed from the fact that she had not completed her initial five day course of antibiotic eye drops. Only after direct questioning did she mention occasional soft contact lens wear, but said that she had worn them for just one day on only two occasions since her problems had begun. She again denied any foreign body sensation.
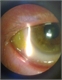
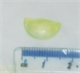
On examination, she had mild conjunctival injection and some sticky yellow discharge at the medial canthus of her right eye. On eversion of her right upper lid, and after instillation of fluorescein drops to check for any corneal epithelial defect, the edge of a soft contact lens was seen protruding from the superior conjunctival fornix, see figure 1. This was removed and found to be half a lens, now stained green with fluorescein (see figure 2).
The remainder of her ophthalmic examination was unremarkable and, importantly, there were no corneal epithelial defects on fluorescein staining and no corneal infiltrates visible on slit lamp examination that might suggest a contact lens-associated microbial keratitis.
On further questioning specifically about her occasional soft contact lens wear, she admitted that about six weeks ago she had noticed that half a contact lens had come out of her eye, but had assumed that the other half had fallen out elsewhere, and had thought nothing more of it. She had not been asked directly about her occasional contact lens wear at any of her four previous medical consultations, and so had not mentioned it before. At none of her previous medical consultations had her lids been everted.
Once the contact lens fragment had been removed, she was prescribed a five day course of chloramphenicol eye drops qds, and a telephone consultation one week later confirmed that all her symptoms had fully resolved.
Discussion
Contact lens wear may cause several ocular complications, ranging from mild dry eye symptoms to contact lens-associated microbial keratitis, which constitutes an ophthalmic emergency.
Contact lens-associated corneal infections can be severe and sight threatening, such as those with the Gram-negative bacterium Pseudomonas aeruginosa, which can rapidly penetrate the cornea,4 or the ubiquitous protozoa Acanthamoeba, which can be introduced to the eye from both soil and water contamination. Consequently, all patients with a history of contact lens wear and red flag symptoms (see table 1) should be referred for an urgent ophthalmic review.
It has been estimated that the annual incidence of contact lens-associated keratitis in developed countries is about 4 per 10,000 in users of daily wear soft contact lenses, the rate being lower in daily wear rigid gas permeable contact lens users, and higher in those using extended wear soft lenses.5 Infections of this nature are, once cultures have been taken, usually treated with intensive topical broad spectrum antimicrobial medication, the nature of which depends on the suspected causative pathogen, and such patients usually require close follow-up under the care of the ophthalmology team.
A recent study of Pseudomonas aeruginosa contact lens-associated keratitis has shown that a third of cases identified had been treated with chloramphenicol (which has no activity against this pathogen) before an appropriate broad spectrum antimicrobial was given, and that these cases had suffered more complications and taken longer to resolve.6
Given the potentially serious associated complications, a history of contact lens wear should be asked about in all patients who present with a red eye in primary care, in case the patients do not volunteer this information spontaneously. It is, therefore, not appropriate to treat symptomatic patients who have a recent history of contact lens wear with a course of chloramphenicol eye drops.
Retained contact lenses have also been well documented to cause several ocular complications, such as giant papillary conjunctivitis7 and ulcerative keratitis which may threaten corneal penetration.8 Delays of up to 40 years in diagnosing retained contact lenses have been documented.9
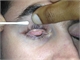
Eversion of the lids, see figure 3, is a simple and useful examination technique that can be carried out in primary care with the aid of a cotton bud stick. Brief videos portraying the technique are readily available on the internet, see Useful information box.
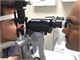
Lid eversion may reveal a hidden sub-tarsal contact lens, which may itself, in the case of soft contact lenses, be made more visible by being stained green after the instillation of fluorescein, as shown in figure 2. Such use of fluorescein may also allow visualisation of any corneal epithelial defect, which would appear bright green when illuminated under a blue light (e.g. with a blue filter attached to a pen torch). However, a careful slit lamp examination by an ophthalmologist is required to exclude this critical finding definitively, see figure 4.
Alternative causes of conjunctivitis, see table 2, may also be a further reason why a bacterial conjunctivitis treated with a course of topical antibiotics fails to resolve quickly. This is most commonly seen in the treatment of viral or allergic conjunctivitis with antibiotic drops. Indeed, the use of topical antibiotics in the treatment of mild to moderate uncomplicated acute infective conjunctivitis, even of bacterial aetiology, is no longer usually indicated.10 A meta-analysis11 looking at primary care treatment of acute infective conjunctivitis with topical antibiotics versus placebo or no treatment found that most patients recovered within a week, regardless of whether antibiotics were used or not.
CONCLUSIONS
This case serves as a reminder to all primary care clinicians to be vigilant for retained foreign bodies as a cause of recalcitrant bacterial conjunctivitis, even in the absence of any foreign body sensation. Such a relapsing-remitting history should prompt a referral to the local ophthalmology department.
All patients presenting with a red eye should be asked specifically about contact lens wear, and causes of conjunctivitis other than bacterial in nature should be borne in mind.
The opportunity should also be taken to look for any of the red flags that may be seen in the context of a contact lens wearer, the presence of which should elicit an urgent referral to an ophthalmologist, as this may herald the onset of a potentially sight-threatening corneal infection.
REFERENCES
1 McDonnell P. How do general practitioners manage eye disease in the community? Br J Ophthalmol 1988;72(10):733-6
2 Sheldrick J, Wilson A, Vernon S, Sheldrick C. Management of ophthalmic disease in general practice. Br J Gen Pract 1993;43(376):459-462
3 www.opticalconfederation.org.uk/downloads/key-statistics/ACLM-Technical-Summary-2012.pdf
4 Jhanji V, Young AL, Mehta JS et al. Management of corneal perforation. Surv Ophthalmol 2011;56(6):522-38
5 Cheng KH, Leung SL, Hoekman HW et al. Incidence of contact-lens-associated microbial keratitis and its related morbidity. Lancet 1999;354(9174):181-5
6 Bourkiza R, Kaye S, Bunce C et al. Initial treatment of Pseudomonas aeruginosa contact lens-associated keratitis with topical chloramphenicol, and effect on outcome. Br J Ophthalmol 2013;97(4):429-32
7 Stenson S. Focal giant papillary conjunctivitis from retained contact lenses. Ann Ophthalmol 1982;14(9):881-85
8 Bhatt PR, Lam FC, Roberts F, Ramaesh K. Peripheral ulcerative keratitis due to a ‘long lost’hard contact lens. Clin Experiment Ophthalmol 2007;35(6):550-2
9 Shams P, Beckingsale A, Sheldrick J, Rose G. An unusual eyelid lump: unsuspected embedded contact lens for up to 40 years. Two cases and literature review. Eye 2011;25 (10):1371-3
10 National Institute for Health and Care Excellence. Clinical Knowledge Summaries: Conjunctivitis - infective: National Institute for Health and Care Excellence http://cks.nice.org.uk/conjunctivitis-infective#! scenario recommendation:2
11 Jefferis J, Perera R, Everitt H et al. Acute infective conjunctivitis in primary care: who needs antibiotics? An individual patient data meta-analysis. Br J Gen Pract 2011;61(590):e542-8

 = Registered users
= Registered users = Paid-up subscribers
= Paid-up subscribers